Introduction
Stress urinary incontinence (SUI) is a common disease in women, with 50–83% of women older than 65 years reported to be affected. In 6–10% of cases, SUI is estimated to be severe [1]. Mid-urethral slings, including transobturator tape (TOT), tension-free vaginal tape (TVT), tension-free vaginal tape-obturator (TVT-O), and a single incision sling, have been the most popular procedures for the treatment of SUI for the last two decades [2]. Tension-free vaginal tape, which was first described by Ulmsten in 1996, had an 81% cure rate in an 11-year follow-up [3, 4]. Complications, such as vascular injury, bladder perforation, and urinary retention, are rarely seen [5, 6]. Prolene TOT insertion via the retropubic route was developed in 2001 and led to reduced morbidity [7]. Later, an inside-out TVT-O procedure (Gynecar; Ethicon, Inc., NJ, USA) was designed by Delava [8].
Postoperative pain symptoms may be observed in both retropubic and TOT surgery. Although the location and duration of the pain can vary, it is often temporary and is generally felt in the thighs. According to the literature, there is no difference between TVT and TOT procedures in terms of pain intensity and frequency [9, 10]. Although the classical TOT procedure is a minimally invasive technique, we believe that this technique can be further improved. Therefore, we describe a new technique called “modified TOT” (mTOT), which avoids periurethral dissection.
Aim
The aim of this study was to determine whether there was a difference in success and complication rates between the classical TOT procedure and mTOT procedure.
Material and methods
In total, 98 patients who underwent TOT surgery between July 2011 and January 2017 were recruited to this prospectively planned study after receiving approval of the local ethics board. The coin flipping randomization technique was used to assign modified or classical TOT status. Of these 98 patients, 47 patients underwent classical TOT, and 51 patients underwent the mTOT procedure. Preoperatively, patient histories were obtained, and all the patients underwent a physical examination, urine analyses, urine culture and antibiogram, the Marshall-Boney test, and the urethral Q-type test. All the patients completed a 24-h voiding diary and underwent urinary ultrasonography to determine the amount of postvoiding residue. Urodynamics was performed in mixed incontinence patients. All patients also completed the Incontinence Impact Questionnaire-7 (IIQ-7).
The exclusion criteria were previous incontinence surgery, known neurological diseases or findings, physical examination findings of above grade 1 pelvic organ prolapse in the Baden system, urethral mobility below 30° in the Q-type measurement and below 60 cmH2O in the leak point pressure measurement. IIQ-7 scores were obtained preoperatively and 1 month, 6 months, and 1 year after the surgery. Postoperative pain was evaluated using the visual analogue scale (VAS) score on the postoperative first day and at 1 months, 6 months and 1 year after surgery. Patients who underwent the classical TOT procedure were allowed to engage in sexual intercourse after the fourth postoperative week versus the tenth postoperative day among those who underwent the mTOT procedure. Lack of urinary incontinence during the provocation test was considered objective recovery. Average or high IIQ-7 scores were considered subjective failure. All remaining conditions were evaluated as surgical success.
Surgical procedure
The surgical field was sterilized using povidone iodine, and a Foley urethral catheter was placed in the dorsal lithotomy position. After labial retraction, sutures were placed, and the surgical area was widened using a weighted vaginal speculum.
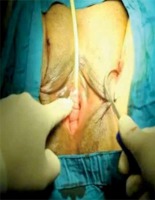
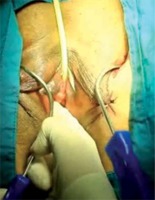
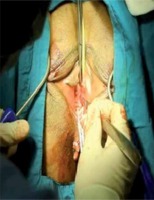
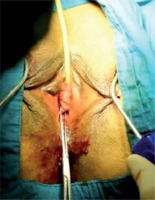
In alignment with the clitoris, 0.5 cm bilateral stab incisions were made inferior to the adductor longus muscle at the genitocrural fold level. Helical needles were inserted and passed through the obturator membrane. Without performing a vaginal incision, the ramus pubis and obturator internus muscles were identified with the index finger of the opposite hand. After locating these structures, the needle was traversed through the obturator membrane, obturator internus muscle, and periurethral endopelvic fascia until it was felt under the vaginal mucosa with the index finger. During this procedure, vaginal anterior wall damage was not observed. In the next step, the needle was pushed until it reached 1.5 cm below the urethral meatus (Photo 1). The same procedure was conducted for the opposite side, so that the needles met 1.5 cm below the urethral meatus (Photos 2 and 3). At this point, a 0.5 cm cut was made, and the needle points were taken outside (Photo 4). The synthetic sling material was attached to the needles, and the needles were backed out. The sling was then brought out through the level of the skin in the groin region. A surgical clamp was placed between the tape and urethra to control the tension. Excess sling material was cut out, and the incisions were closed with 4/0 fast-absorbing sutures. Cystourethroscopy was performed for the first 20 patients who underwent the modified technique. However, cystourethroscopy was later removed from the routine procedure, as no injury was observed. Vaginal tampons were used for the classical technique group to control bleeding but not for the modified technique group. Foley catheters of both groups as well as the vaginal tampons were removed on the first postoperative day. All patients were discharged on the first postoperative day after confirmation post-void residual urine control.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki Declaration and its later amendments or comparable ethical standards.
Informed consent: Informed consent was obtained from all individual participants included in the study.
Statistical analysis
Numerical variables were expressed as median and quantitative variables as frequencies and percentages. The Shapiro-Wilk test was conducted to assess the conformity of the data to a normal distribution. Categorical variables were analyzed by the χ2 or Fisher’s exact test, and continuous variables were analyzed by the Mann-Whitney U test. Statistical analyses were performed using SPSS 21.0 (SPSS Inc., Chicago, IL, USA), and p < 0.05 was considered statistically significant.
Results
Demographic data of the classical TOT and mTOT groups are presented in Table I. There were no between-group differences in mean age, body mass index, parity, previous pelvic surgeries, menopausal status, presence of diabetes mellitus, and hypertension.
Table I
Patients’ characteristics in classical and modified TOT groups
Postoperative complications are shown in Table II. Nerve damage, vascular damage, retropubic hematomas, and bladder-urethra erosion were not observed in either group.
Table II
Postoperative complications
| Variable | Classical TOT | Modified TOT | P-value |
|---|---|---|---|
| Inguinal pain | 3 | 2 | 0.12 |
| Urinary retention | 1 | 1 | 0.91 |
| Dyspareunia | 1 | 0 | 0.26 |
| Urgency | 2 | 2 | 0.88 |
| Total | 7 | 5 | 0.72 |
There were no significant between-group differences in IIQ-7 scores (Table III).
Table III
Changes between preoperative and postoperative scores of IIQ-7
| Variable | Classical TOT | Modified TOT | P-value |
|---|---|---|---|
| IIQ-7 Preop. | 10 (7–5) | 9 (7–15) | 0.74 |
| IIQ-7 1st month | 1 (0–3) | 1 (0–3) | 0.78 |
| IIQ-7 6th month | 1 (0–3) | 1 (0–2) | 0.89 |
| IIQ-7 1st year | 1 (0–2) | 1 (0–2) | 0.81 |
Although there were no between-group differences in postoperative 1-month, 6-month, and 1-year VAS scores, the postoperative first day scores of the mTOT group were significantly lower than those of the classical TOT group (p < 0.05) (Table IV).
Discussion
Since the publication of Ulmstein’s study in 1996, various mid-urethral sling technologies have been used. In the last decade, urethral-type synthetic slings have been used in 83.9% of all incontinence surgery procedures, and 26.9% of these employed the TOT technique [11]. Although techniques for SUI treatment were successful, modified techniques were developed with the aim of obtaining better outcomes, such as reduced morbidity and increased rates of success. In 2009, Lee et al. [12] described the use of a new surgical technique, canal TOT, and Long et al. [13] described the use of another technique, modified prepubic TVT, in 2013 [13]. The results of their studies revealed no superiority between the new techniques when compared with those of classic techniques [12, 13]. In the present study, postoperative pain was significantly lower in the mTOT group on the first postoperative day as compared with that in the classic TOT group. The pain scores of the two groups were not significantly different at postoperative 1 month, 6 months, and 1 year.
The TOT technique described by Delorme et al. in 2001 [7] is preferred due to its ease of use and rapid application. Moreover, intraoperative complication risks are considered to be lower using the TOT technique of Delorme et al. than TVT and modified TVT techniques. The TVT procedure poses a higher risk of bladder, bowel, urethral, and vascular injuries than the TOT procedure, although the success rates with the two procedures are similar [14]. In addition, complications, such as bladder perforation, urethral injury, and retropubic hematomas, have been reported in TOT operations. Surgeons who have experience of such complications suggest that creating a wide tunnel enough for the surgical finger and pushing the needle with the guidance of this finger can decrease the risk of complications. However, this method may damage the neurovascular function of the periurethra, and wide dissection may hinder proper placement of the sling material [4, 5]. Furthermore, after the sling material is placed, it may migrate to distal or proximal areas [15–19]. In the proposed technique described herein, the needle is pushed with the guidance of a finger, feeling it into the submucosa, without performing a dissection. Due to the avoidance of paraurethral dissection and the placement of the sling material at the appropriate level, the migration risk of the sling material to the bladder neck or another location is removed.
Schierlitz et al. [20] studied patients with intrinsic sphincter deficiency and divided them into TOT and TVT groups. Within a 3-year follow-up time, 20% of patients who underwent TOT procedures required further surgery, whereas this figure was only 1.4% in the TVT group. Several reasons have been put forward to explain the difference in outcomes between the two techniques. Firstly, when the sling material is placed during the TVT procedure, the pelvic fascia may be perforated. Secondly, the non-dissected area is longer, which allows better localization and prevents migration of the sling material. As our technique avoids dissection and prevents migration of the material, we believe that its success rate may be close to that of TVT for patients with intrinsic sphincter deficiency.
Patients who underwent the classical TOT procedure were allowed to engage in sexual intercourse after the fourth postoperative week as compared with the tenth postoperative day for patients who underwent the mTOT procedure. In this study, mTOT patients reported less dyspareunia after early sexual activity. The resumption of earlier sexual activity due to the lack of introital wound tenderness is another advantage of our technique.
Conclusions
This modified technique provides the same efficiency and reliability as the classic technique, but is more advantageous in terms of pain reduction and resumption of earlier sexual activity. The limitations of this study were the small number of patients, and the patient groups were not randomly selected. Additional studies, with longer-term follow-ups may provide more insights into the effects of the mTOT procedure.