Introduction
Diabetes mellitus (DM) is an autoimmune disease characte-rized by hyperglycemia accompanied by disturbance in the meta-bolism of carbohydrates, proteins and also lipids [1]. It has been predicted that the prevalence of diabetes would be raised worldwide from 177 million in 2000 to 370 million in 2030 [2]. In Egypt, the prevalence rate of type 1 DM (T1D) among school children in Cairo was 1.09/1000 [3].
In humans, diabetes mellitus is one of the most prevalent conditions with spontaneous manifestations [4]. In animals, T1D can be induced by the administration of diabetogenic inducing drugs such as streptozotocin, alloxan and anti-insulin serum. These agents selectively destroy the Langerhans islet β-cells [5]. The initiation of T1D requires both CD4+ T cells that are insulin reactive and CD8+ T cells that play a major role as β-cell killers [6]. In addition, B cells, natural killer (NK) cells, natural killer T cell (NKT), γδT and macrophages participate in T1D disease progression [7].
NK cells play an important role in direct killing of target cells that are transformed or infected by certain microorganisms [8]. The natural cytotoxicity receptors include NKp46, NKp30, and NKp44 that are expressed on NK cells [9]. NK cells appeared in the pancreas when insulitis progressed to T1D and NKp46 engagement by beta cells lead to degranulation of NK cells [10]. Injection of soluble NKp46 proteins into non-obese diabetic mice during the early phase of insulitis and the pre-diabetic stage prevent the development of T1D [11]. These findings demonstrate that NKp46 has a great role in T1D and highlights potential new therapeutic modalities for this disease.
Regulatory T cells (Tregs) were first described as suppressors of antigen-activated immune responses to self and non-self-antigens [12]. Several markers for Tregs, such as human transcription factor forkhead box P3 (FoxP3), CTLA-4, CD25 and CD127 have been implicated [13]. FoxP3 could be most essential for the development and the maintenance of their suppressive function [14]. Mutations and disruptions of the Foxp3 regulatory pathway lead to organ-specific autoimmune diseases such as T1D [15].
Interleukin 2 (IL-2) is mainly secreted by activated T cells and, to a lesser extent by activated dendritic cells, natural killer (NK) cells, NKT cells, as well as B cells [16]. NK cells and T cells constitutively express receptors (CD122 and CD132), by which they respond to high-dose IL-2 and been activated [17]. Tregs constitutively express the high-affinity receptor for IL-2 (CD25), while this expression on other subsets of T cells is induced merely after activation. Therefore, in the steady state, Tregs respond better to IL-2 than other T cells [18]. This is why low dose IL-2, hypothetically, would preferentially increase Tregs numbers without causing overall immune activation [19]. In fact, Tregs activation has been linked to IL-2 administration in mice and a short course of low-dose IL-2 administration can reverse established disease [20].
Malek and colleagues reported that Tregs from normal individuals were invariably better responders to IL-2 followed by NK cells and memory T cells. Further work is needed to determine heterogeneity of responsiveness to low-dose IL-2 in Tregs as well as other IL-2–responsive cells, especially NK cells [21].
Chitosan is a polymer that is either partially or fully deacetylated chitin. It has been investigated extensively as a potential drug carrier due to its biocompatible characteristics. Therefore, it has been used widely in the medical field [22]. Studies recommended its use to coat other material nanoparticles to increase their bioavailability and decrease their impact on the body [23].
We intended in the present work to evaluate the modulatory effect of low dose IL-2 loaded chitosan nanosphere on NKp46 expressing natural killer cells and to compare this to its effect on foxp-3 expressing T regulatory cells in diabetic male inbreed Balb/c mice.
Material and methods
Experimental animals
A total of 116 BALB/c mice (10-12 weeks old and 20-25 grams weight), were housed in polycarbonate cages inside a well-ventilated room. Each cage contained not more than 5 mice. They were maintained under standard laboratory conditions of temperature (22oC) with light/ dark cycles of 12 hours each where mice had free access to water and pellet diet. The streptozotocin (STZ)-induced diabetic mice were fasting overnight before the start of the experiment [24]. All procedures were performed in accordance with regulations of Medical Research Institute guide for the care and the use of laboratory animals and after the acceptance of the Ethical Committee of the Alexandria University. Mice were purchased from the animal house of the Medical Technology Center, in Medical research institute, Alexandria University. The study was conducted from January to August 2018.
Mice were divided into five groups:
Group I: includes 51 mice induced for T1D, injected with murine recombinant IL-2 loaded into chitosan nanoparticles;
Group II: includes 21 mice induced for T1D, injected with murine recombinant IL-2;
Group III: includes 20 mice induced for T1D, injected with empty chitosan particles;
Group IV: includes11 mice induced for T1D not injected with any formulation as first control group. (control 1: diabetic mice);
Group V: includes 8 mice free from T1D as a second control group (control 2: non-diabetic mice).
Type 1 diabetes mellitus induction protocol
T1D was experimentally induced according to the protocol described by Brosius [25]. Filtered sterilized cold Citrate buffer was added to Streptozocin (STZ) 9200 µl/mg) (STZ, SIGMA, Germany) to a concentration of 5 mg/ml. Citrate buffer (0.1 M): 2 part of sodium citrate (0.1 M) and 3 part of citrate acid (0.1 M), pH adjusted to 4.0 by using NaOH (1 N). Intraperitoneal injection of streptozotocin (200 mg/kg body weight (bw) was used, divided into 5 consecutive daily doses of 40 mg/kg bw each. Negative control mice received freshly prepared sodium citrate buffer by the same route.
Blood from retro-orbital sinus of all mice were collected for assessment of glucose and insulin level. Blood glucose was done by glucometer (mg/dl) while insulin level (pmol/l) was measured by enzyme-linked immunosorbent assay (ELISA).
Preparation of IL-2 loaded chitosan nanoparticles
Low molecular weight chitosan (48 kDa) derived from shrimp shells (Pandalus borealis), was purchased from Primex Co (Iceland]. Interleukin-2 was provided in the form of 200 µg/ml liquid, purchased from BioLegend Company (Netherlands). Chitosan nanoparticles (CSNPs) free or loaded with IL-2 were prepared by ionic gelation method. One mg/ml of low molecular chitosan was dissolved in 1% (w/v) acetic acid and sonicated before the solution become transparent. Triphenyl phosphate (TPP] solution (1 mg/ml) was added drop wise to CS solution (pH = 5), under continuous stirring at 600 rotation per minute (rpm) for 30 minutes at room temperature. CSNPs spontaneously form via the electrostatic attraction between positively charged primary amino groups on chitosan chains and reversely charged polyanions (from TPP).
Recombinant murine interleukin 2 loaded chitosan nanoparticles were prepared according to Bertohold et al. [26]. Recombinant IL-2 with different concentration (0.05-0.1 and 0.33 µIU) were added to sodium sulfate solution (20% w/v). Sodium sulfate solution containing murine recombinant IL-2 was dropped into the acidic chitosan solution and stirred at 500 rpm for 1 h. The resulting opalescent suspension was determined as IL-2 loaded chitosan nanoparticles. Reaction mixture was centrifuged at 15 000 rpm at 4oC for 15 min. The supernatant was decanted and nanoparticles were suspended in sterile distilled water and centrifuged at 15 000 rpm at 4oC for 15 min to separate the nanoparticles.
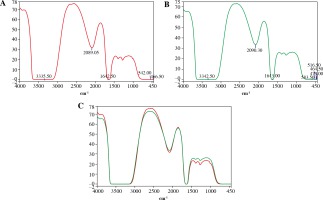
IL-2 encapsulation efficiency of chitosan NP was determined by measuring the difference between the amount of protein incorporated in the nanoparticles preparation medium and the amount of non-entrapped protein remaining in the aqueous medium after the encapsulation process. Protein content in the supernatant was spectrophotometrically determined by universal protein content assay. Characterization of nanospheres was done using scanning electron microscope [27] (Fig. 1), furious transmission Infra-Red (Fig. 2) [28] and Zetasizer [29]. IL-2 loading and encapsulation efficacy of the nanoparticles was around 97%.
Fig. 1
Scanning electron microscope images: showing CSNPs in the upper part of the figure with spherical porous morphology with average diameter of 91.835 nm. Lower part of the figure shows images for CSNPs loaded with IL-2 (spherical porous morphology with average diameter of 276.3175 nm

Fig. 2
FT-IR spectrum of Chitosan using FT-IR spectroscopy (Shimadzu, FT-IR-8400S, Japan). A) The stretching vibration of OH and NH2 groups is centered at 3335.60 cm-1 for CSNPs , the peaks at 2089.05 cm-1 with C-H stretching vibration for CSNPs, C=O vibration appears at 1642.50 cm-1 of acetyl groups in chitosan. The peaks around 542 cm-1 correspond to saccharide structure of chitosan. B) The stretching vibration of OH and NH2 groups is centered at 3342.5 cm-1 (steady state) for CSNPs loaded with IL-2, the peaks at 2090.30 cm-1 with C-H stretching vibration for CSNPs loaded with IL-2, C=O vibration appears at 1643 cm-1 in CSNPs loaded with IL-2. The peaks around 5 583.50 cm-1 for CSNPs loaded with IL-2). C) The two curves are almost identical indicates no change in characters between of CSNPs and CSNPs loaded with IL-2
IL-2 loaded chitosan injection protocol
Following STZ injection (40, 45 or 50 mg/kg/day), IL-2 loaded onto chitosan was prepared with actual dose of 0.05, 0.1 and 0.3 µIU divided into 5 consecutive days administrated by subcutaneous injection according to protocol of klatzmann Abbas [30]. Mice were sacrificed at day 7, 14 and 21 following IL-2/chitosan administration.
Short term culture
Spleens were removed and collected into Petri dishes (7.5 × 1.5 cm; Biosystem S.A., Spain), washed with 1 ml phosphate buffer saline (PBS) (pH = 7.2) then squeezed. PBS was added to cells and centrifuged at 2,000 rpm for 3 minutes. Cell pellet was resuspended, counted and adjusted to 1 × 106/ml in 4 ml complete tissue culture medium composed of RPMI-1640 supplemented with L-glutamine, 10% heat-inactivated fetal calf serum, penicillin (100 IU/ml)and streptomycin (100 µg/ml). Splenocytes were maintained in a short-term culture (48 hours) stimulated with 10 µl of Concavalin A(Con A) (plant mitogen, known for its ability to stimulate mouse T-cell subsets) (Dwyer et al.). Details of the tissue culture protocol were adopted from the standard method developed by Davis [31].
NK and Treg cells expression
Assessment of NK and Treg cells was done using both flow cytometry (Cytomics FC500 flow cytometer) and ELISA. Monoclonal antibodies (mab) were purchased from (eBioscience, San Diego, CA), anti-CD3-FITC, anti-CD4-PE and anti-CD25-FITC or anti-CD56-PE. The frequency of each cell subset was calculated based on the percentage of positive cells in the total lymphocyte gate. For intracellular staining, cells were first labeled with relative marker, fixed, and permeabilized using a fix/perm kit according to the manufacturer’s instructions and then labeled with anti-FOXP3-PE or anti-NKp46-PE mab (PCH101; eBioscience).
NKp46 and Foxp3 were measured also in cell lysate by sandwich ELISA for in vitro quantitative measurement (mybiosource.com/prods/ELISA-Kit/mouse/forkhead-box-P3, NKp46). Following cell culture of mouse spleen Cells, repeated freezing and thawing cycles were done to damage cells and let out the inside components of the cell then Centrifugation at 2000-3000 RPM for approximately 20 minutes was done. The supernatants were collected carefully and centrifuged again when sediments occurred during storage.
In vitro suppressor assay
YAC-1 responder cells (ATCC® TIB160™) acquired from Medical Technology Center in Alexandria University, were co-cultured with isolated NK cells in the absence or presence of Tregs (CD4+CD25+) cells to study the suppressive activity of Tregs. One million of responder cells were labeled by incubating cells with 100 mCi 51Cr for 90 min at 37°C, washing them three times with PBS, and seeding them at 104 cells/well in round-bottom 96- well plates. The previously isolated NK cells were added to each well and cultured together at a ratio of 1 : 0.5, respectively, in RPMI-1640 complete culture medium. After 4 h incubation, 100-ml volumes of supernatant were collected and the amount of 51Cr released was measured using a g counter. NK cells were harvested and assessed for IFN-γ production by ELISA and percentage of responder cells killing. IFN-γ levels were estimated using commercial ELISA (Quantikine R&D system, ELISA kit, USA) according to manufacturer recommendation [32].
Statistical analysis
All analyses were performed using SPSS software (SPSS for windows, version 21.0, Chicago, IL, USA) [33]. The test of normality was done using D’Agstino test. Quantitative data were described using mean and standard deviation for normally distributed data while abnormally distributed data was expressed using median, minimum and maximum. For normally distributed data, comparison between populations was done using t-test and (ANOVA) & Pearson correlation coefficient. For abnormally distributed data, Mann-Whitney test and Spearman correlation were used. p-value smaller than 0.05 or 0.01 indicates statistical significance.
Results
Animal grouping and characteristics
An independent biostatistician (Graphpad Software) was used to calculate sample sizes. The analyses were predetermined (protocol-specific). The present study included 107 mice (93%) used as a model for experimental T1D and 8 (7%) as negative controls. One week following diabetes induction, fifteen diabetic mice were left without any treatment and represented the positive control group. Another 20 (17%) diabetic mice were treated with empty chitosan nanoparticles and 21 (18%) were treated with free IL-2 at concentrations of 0.05, 0.1 and 0.3 uIU/ml. Another 51 (44%) diabetic mice were treated with the same concentrations of murine recombinant IL-2 loaded into chitosan nanoparticles. At weekly intervals after IL-2 treatment, mice from all groups under study were sacrificed.
Blood glucose level was monitored once before and daily after STZ injection until a diabetic status was confirmed. Insulin levels were also measured and used in parallel to animal weight to moni-tor the diabetic status of mice (data not shown).
Effect of different formulations on the expression of NK cells and NKp46
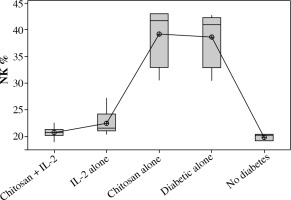
NK cells show significant changes in number in different ani-mal groups (Fig. 3). As we noticed, mice induced for T1D had higher numbers of NKp46+ NK cells (mean ±SD = 38.7 ±5.66%) and had no significant difference from those mice injected with empty chitosan nanoparticles (mean ±SD = 39.20 ±6.02%) (p = 0.999).A significant decrease in NK expression was seen in mice injected with low dose IL-2 (mean ±SD = 22.43 ±2.47%) or low dose IL-2 loaded in chitosan nanoparticles (mean ±SD = 22.43 ±2.47%) with no statistical difference between the latter and the non-diabetic group (mean ±SD =19.823 ±0.652%) (p = 0.988).
Fig. 3
NK cell expression in different groups. Data showed as percentage of expression by FACS. Group I: chitosan + IL-2 represented by 51 diabetic mice treated with chitosan + IL-2 (0.3) µIU, Group II represented by 21 diabetic mice treated with IL-2 alone (0.3) µIU, Group III represented by 20 diabetic mice treated with chitosan alone (empty chitosan), Group IV represented by 11 diabetic mice and Group V represented by 8 non-diabetic mice
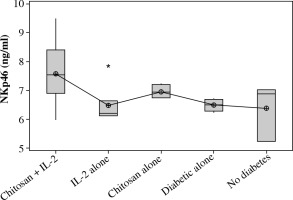
On the other hand a significant increase in cell lysate NKp46 expression was seen in mice injected with IL-2 loaded chitosan than other groups. However, a significant NKp46 expression reduction was noticed in mice injected with low dose IL-2 alone (p = 0.01) (Fig. 4).
Fig. 4
NKp46 in cell lysate in different groups. Data showed as (ng/ml) by ELISA. Group I: chitosan + IL-2 represented by 51 diabetic mice treated with chitosan + IL-2 (0.3) µIU, Group II represented by 21 diabetic mice treated with IL-2 alone (0.3) µIU, Group III represented by 20 diabetic mice treated with chitosan alone (empty chitosan), Group IV represented by 11 diabetic mice and Group V represented by 8 non-diabetic mice
Effect of changes of doses of IL-2 loaded chitosan on NK cell and NKp46 expression
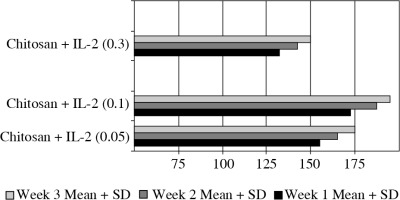
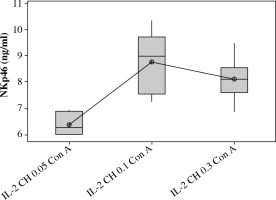
We used three different doses of IL-2 loaded chitosan injections (0.05, 0.1 and 0.3 µIU). A highly statistical reduction in NK cell expression was noticed in mice injected with (0.3) µIU (p = 0.00). A non-significant difference was shown between the two other doses (p = 0.901) (Fig. 5). For NKp46 expression in cell lysate, a statistical elevation was noticed in mice injected with (0.1) µIU and a significant reduction was seen in mice injected with (0.05) µIU (Fig. 6).
Fig. 5
Effect of changes of doses of IL-2 + chitosan on NK cell expression. Data showed as percentage of expression by FACS. Group I: chitosan + IL-2 (0.05) µIU represented by 17 diabetic mice treated with chitosan + IL-2 (0.05) µIU, Group II represented by 17 diabetic mice treated with chitosan + IL-2 (0.1) µIU, Group III represented by 17 diabetic mice treated with chitosan + IL-2 (0.3) µIU
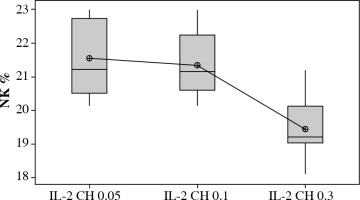
Fig. 6
Effect of changes of doses of IL-2+chitosan on NKp46 in cell lysate in different groups. Data showed as (ng/ml) by ELISA. Group I : chitosan + IL-2 (0.05 µIU) represented by 17 diabetic mice treated with chitosan + IL-2 (0.05 µIU), Group II represented by 17 diabetic mice treated with chitosan + IL-2 (0.1 µIU), Group III represented by 17 diabetic mice treated with chitosan + IL-2 (0.3 µIU)
Effect of duration of treatment with IL-2 loaded chitosan (0.3 µIU) on NK cell and NKp46 expression
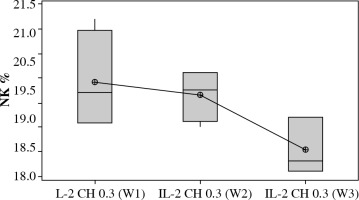
Our results showed a decrease in NK cell expression in the mice injected for three weeks with the dose (0.3 µIU) of chitosan loaded with IL-2 (mean ±SD = 18.537 ±0.584%) but this reduction was not statistically significant between the three groups with different durations (p = 0.105) as shown in Figure 7.
Fig. 7
Effect of duration of treatment with IL-2 loaded chitosan (0.3) µIU on NK cell expression in the three weeks. Data showed as percentage of expression by FACS. Group I: chitosan + IL-2 (0.3 µIU) represented by 7 diabetic mice treated for one week, Group II represented by 6 diabetic mice treated with chitosan + IL-2 (0.3 µIU) for two weeks, Group III represented by 6 diabetic mice treated with chitosan + IL-2 (0.3 µIU) for three weeks
Expression of Foxp3
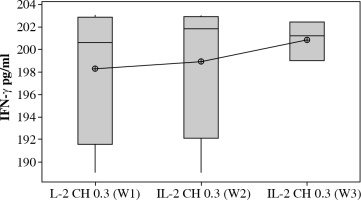
Both Treg cells percentage and cell lysate Foxp3 [ng/ml] were significantly highly expressed in mice injected with IL-2 loaded chitosan than other mice groups (Figs. 8 and 9).
Fig. 8
Treg cell expression in different groups. Data showed as percentage of expression by FACS. Group I: chitosan + IL-2 represented by 51 diabetic mice treated with chitosan + IL-2 (0.3 µIU), Group II represented by 21 diabetic mice treated with IL-2 alone (0.3 µIU), Group III represented by 20 diabetic mice treated with chitosan alone (empty chitosan), Group IV represented by 11 diabetic mice and Group V represented by 8 non-diabetic mice
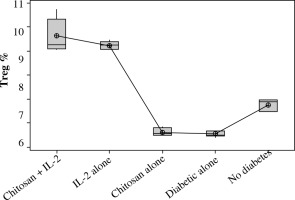
Fig. 9
Foxp3 in cell lysate in different groups. Data showed as (ng/ml) by ELISA. Group I: chitosan + IL-2 represented by 51 diabetic mice treated with chitosan + IL-2 (0.3 µIU), Group II represented by 21 diabetic mice treated with IL-2 alone (0.3 µIU), Group III represented by 20 diabetic mice treated with chitosan alone (empty chitosan), Group IV represented by 11 diabetic mice and Group V represented by 8 non-diabetic mice
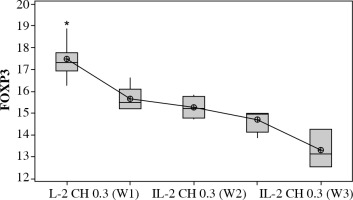
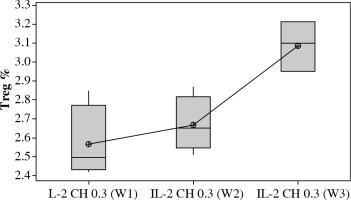
Our results showed a significantly statistical difference elevation with (0.3 µIU) doses as shown in Figure 10. This elevation was the highest in the third week (Fig. 11).
Fig. 10
. Effect of changes of doses of IL-2+chitosan on Treg cell expression. Data showed as percentage of expression by FACS. Group I: chitosan + IL-2 (0.05 µIU) represented by 17 diabetic mice treated with chitosan + IL-2 (0.05 µIU), Group II represented by 17 diabetic mice treated with chitosan + IL-2 (0.1 µIU), Group III represented by 17 diabetic mice treated with chitosan + IL-2 (0.3 µIU)
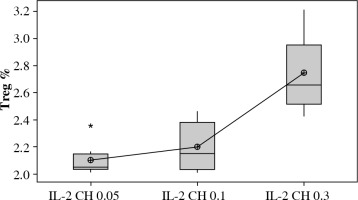
Fig. 11
. Effect of duration of treatment with IL-2 loaded chitosan (0.3 µIU) on Treg cell expression in the three weeks. Data showed as percentage of expression by FACS. Group I: chitosan + IL-2 (0.3 µIU) represented by 7 diabetic mice treated for one week, Group II represented by 6 diabetic mice treated with chitosan + IL-2 (0.3 µIU) for two weeks, Group III represented by 6 diabetic mice treated with chitosan + IL-2 (0.3 µIU) for three weeks
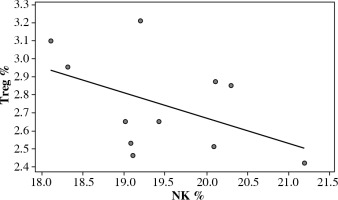
Correlation between Treg and NK expression in low dose IL-2 loaded chitosan (0.3 µIU) injected mice
A statistical significant inverse correlation was found between Treg and NK cell expression in mice treated with IL-2 loaded chitosan with low dose (0.3 µIU) (r = –0.473, p = 0.041) (Fig. 12).
NK cell functional assay
Secretion of IFN-γ by cultured NK cells with Treg cells in the culture supernatant showed significant decrease in those groups treated with chitosan loaded IL-2 (p < 0.00) (Fig. 13). This reduction was not significantly different between different doses (p = 0.586) (Fig. 14). When we compare the dose (0.3 µIU) of chitosan loaded IL-2 in different duration of treatment, an insignificant difference also was found in the level of secreted IFN-γ in the culture supernatant (p = 0.839) (Fig. 15).
Fig. 13
. IFN-γ in cell supernatant of co-cultured NK+Treg in different groups. Data showed as (pg/ml) by ELISA. Group I: chitosan + IL-2 represented by 51 diabetic mice treated with chitosan + IL-2 (0.3 µIU), Group II represented by 21 diabetic mice treated with IL-2 alone (0.3 µIU), Group III represented by 20 diabetic mice treated with chitosan alone (empty chitosan), Group IV represented by 11 diabetic mice and Group V represented by 8 non-diabetic mice
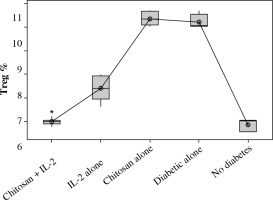
Fig. 14
. Effect of changes of doses of IL-2+chitosan on IFN-γ secretion in culture supernatent. Data showed as (pg/ml) by ELISA. Group I: chitosan + IL-2 (0.05 µIU) represented by 17 diabetic mice treated with chitosan + IL-2 (0.05 µIU), Group II represented by 17 diabetic mice treated with chitosan + IL-2 (0.1 µIU), Group III represented by 17 diabetic mice treated with chitosan + IL-2 (0.3 µIU)
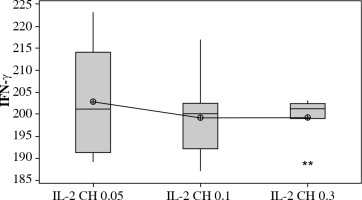
Fig. 15
. Effect of duration of treatment with IL-2 loaded chitosan (0.3 µIU) on IFN-γ in cell supernatant of co-cultured NK+Treg in different groups. Data showed as percentage of expression by FACS. Group I: chitosan + IL-2 (0.3 µIU) represented by 7 diabetic mice treated for one week, Group II represented by 6 diabetic mice treated with chitosan + IL-2 (0.3 µIU) for two weeks, Group III represented by 6 diabetic mice treated with chitosan + IL-2 (0.3 µIU) for three weeks
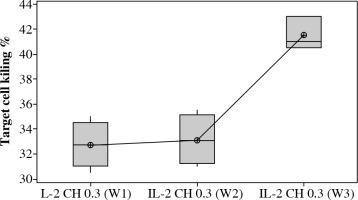
The percentage of target cell killing was significantly lower in mice injected with (chitosan + IL-2) (p < 0.01) and between mice injected with this formulation and mice injected with IL-2 alone (p = 0.043) (Fig. 16). This impairment of killing ability was the significantly decreased with (0.3 µIU) dose of chitosan + IL-2 (p = 0.006). However, a change in the duration of treatment with this dose does not show any significant difference between mice injected for one week (mean ±SD = 32.75±1.85%) or two weeks (mean ±SD =33.13±2.02) with (0.3 µIU) (p=0.954) (Fig. 17).
Fig. 16
. Cytotoxicity suppression assay: Data show target cell killing in co-cultured NK+Treg in different groups. Data showed as percentage of killed cells. Group I: chitosan + IL-2 represented by 51 diabetic mice treated with chitosan + IL-2 (0.3 µIU), Group II represented by 21 diabetic mice treated with IL-2 alone (0.3 µIU), Group III represented by 20 diabetic mice treated with chitosan alone (empty chitosan), Group IV represented by 11 diabetic mice and Group V represented by 8 non-diabetic mice
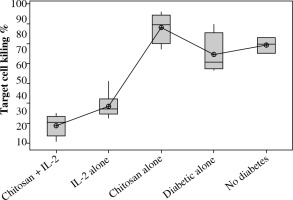
Fig. 17
. Effect of duration of treatment with IL-2 loaded chitosan (0.3 µIU) on suppressive ability of Treg on NK cell in co-cultures. Data show target cell killing in co-cultured NK+Treg in different groups as percentage of killed cells. Group I: chitosan + IL-2 (0.3 µIU) represented by 7 diabetic mice treated for one week, Group II represented by 6 diabetic mice treated with chitosan + IL-2 (0.3 µIU) for two weeks, Group III represented by 6 diabetic mice treated with chitosan + IL-2 (0.3 µIU) for three weeks
Effect of different formulations on the glucose level and weight
This was shown in Table 1 and Figure 18.
Table 1
Effect of treatment on glucose level and weight
Discussion
Autoimmune diabetes (type 1 diabetes) initiation and progression are primarily caused by Teff cells, but NKs have been identified in the pancreas of T1D patients and in experimental mouse models of T1D [34, 35]. At diabetes onset, there is an altered Teff/Treg ratio and increased IFNγ production aggravating autoimmunity in pancreatic microenvironment which is correctable with low dose IL-2 [36].
Grinberg-Bleyer et al. stated the significant role of IL-2 in the non-obese diabetic mice (NOD) pancreatic microenvironment for Treg survival and function. The IL-2 pathway is impaired in NOD mice, and that is accompanied by decreased IL-2 levels [19]. There were suggestions that before the onset of the disease; Tregs consume predominantly IL-2, allowing for normal Treg numbers with appropriate Teff/Treg ratio. Perhaps, Tregs have a competitive advantage in this microenvironment based on their constitutive expression of IL-2Rs that is higher than that expressed on CD25-expressing NKs or on activated T cells [37].
Though, in the pancreatic microenvironment, the decrease in Tregs at disease onset might enable the accumulation of NKs. These IFNγ-producing NKs become activated and aggravate autoimmunity by boosting the responses of autoreactive Teff [38], or if an exceedingly high doses of IL-2 are present [39]. Conversely, an appropriate low dose IL-2 could enhance Tregs and promote regulation on these proinflammatory NKs, which has not yet been studied.
Low-dose IL-2 was studied to selectively stimulate Tregs and their regulatory function. Data emerging from T1D trials with these autologous Tregs demonstrate the limitations of protocols that rely on expanded Tregs infusion without any recipient manipulation. The role of NKs in this context is not established and requires to be understood in order to improve therapeutic strategies aimed at resetting the balance between Teff and Tregs. However, there are contradictory reports about NK involvement in autoimmune diabetes models describing both protective and destructive functions.
Together with their role to contribute to an inflammatory environment, NKs respond to IL-2 and compete for IL-2 during early diabetes development in mice, hence impacting immune-based therapies. So, it is a necessity to unravel the correlations between NK and Treg cells to better understand the controversial role of NKs in diabetes. Thus, we intended at this work to study the regulatory effect of low dose IL-2 in experimentally induced diabetic mice, on NK cell in relation to Treg cell expression.
Unfortunately, a former prescription form of IL-2 (proleukin) has an explicit warning for exacerbation of a variety of autoimmune and inflammatory diseases [40]. Therefore, we created a new mode of delivering the low dose of IL-2 selectively to target cells by using chitosan nanoparticles. Chitosan has received growing attention mainly due to their ability to target specific delivery systems [41].
For this purpose we prepared three formulations of IL-2 with three low doses (0.05-0.1 and 0.3 µIU) loaded on chitosan nanosphere, and injected those at three weekly intervals in three groups of experimentally induced diabetic mice. Our main goal was to evaluate the effect of low dose IL-2 on NK cells as a novel mechanism to set the balance between them and Tregs. This evaluation of NK expression was designed to assess the expression of NK cell in splenocyres as well as the NKp46 level and the NK cell cytotoxicity.
The use of NKp46 marker for identification of bulk NKs would be a very accurate measure of NK. Furthermore, the surface expression of NKp46 was found to be conserved on NK cells across mammalian species. On this basis, NKp46 could be a consistent marker to identify NK cells in different animal models. This comparison was not possible before because of the lack of a common and comprehensive receptor repertoire between dissimilar species [42].
We intended to compare the three doses of IL-2 to find the dose that has caused more NKP46 modulation at this new onset diabetes, then we monitored the statistical differences in levels of NKp46 and Foxp3 – as markers of NK and Treg cells activity respectively- from mice which are injected with other formulations including: IL-2 alone or chitosan alone.
Our observations revealed conflicting results between surface expression of NKp46 on NK cells and their secreted form in cell lysate. While a decrease in the expression of NKp46+ NK cells was noticed in mice treated with the low dose IL-2 loaded in chitosan. This reduction was significantly observed in dose (0.3 µIU) and in mice treated for three weeks. This could be related to findings of Hirakawa et al., which revealed the indirect effects of prolonged exposure to low concentrations of IL-2 on NK cells in vivo [43].
On the other hand, an elevation in secreted level of NKp46 was observed in cell lysate in this group of mice. This could be explained by the findings of Ito et al. who found that NK cells are preferentially expanded by low dose IL-2 in a dose dependent manner but their most prominent expansion observed was at dose level of 200,000 IU/m [44]. Healthy humans express the ligand for the NKp46 receptor [34] and this could be impaired in diabetes. The expression of the NKp46 ligand is stable in functional β cells and therefore β cells are constantly at risk of being attacked by NKs through NKp46-stimulated activation. In vitro, incubation of NKs with β cells leads to NK degranulation and β cell killing. The NKp46 receptor was also found critical in diabetes development in vivo in low dose STZ-diabetes in B6 mice [45].
NK cell’s killing and cytokine secretion ability showed an observed impairment when co-cultured with isolated Tregs. This suppressive capability of Treg was more prominent in mice treated with chitosan + IL-2 formulation. However, it showed no correlation to the dose or duration of this treatment. This indicates a critical role of Tregs in NK homeostasis, activation, and function, predominantly by controlling the availability of IL-2 in the microenvironment. Data from the Mathis group show that in the absence of Treg cells, NKs produce abundant IFN-γ and contribute to the diabetic lesion in NOD mice. NKs were found to be initiators of autoimmune responses by stimulating CD4 T cells [46]. Additionally, IL-2 was the critical link between Treg and NKs in the pancreatic microenvironment [47].
Moreover, our results showed a statistical significant correlation between NKp46 and Foxp3 expression in IL-2 loaded chitosan receiving group of mice with low doses (0.3 µIU). The maximum Foxp3 expression was observed at the dose (0.3) µIU. This comes in non-accordance with Zorn et al. who found that the effect of IL-2 on Foxp3 expression in Tregs was detectable at concentrations as low as 0.1 U/ml, which likely target the high-affinity receptor for IL-2 [48]. Also, in disagreement to our results, Tang et al. found that NOD mice treated with low dose of IL-2 in the form of a IL-2/anti-IL-2 mAb complex led no difference in expression of NK cells [49], but this is obviously due to the different formulation they used. In addition, Baeyens et al. found that administration of low-dose IL-2 alone or combined with rapamycin counteracted IL-2 effects on Treg cells, failed to control IL-2-boosted NK cells, and broke IL-2–induced tolerance in a reversible way [40].
Our group is working nowadays on comprehensive mapping to the IL-2 signaling network to further elucidate the molecular mecha-nisms of IL-2 that could facilitate the development of specific agonists and antagonists to efficiently modulate immune responses.