Breast cancer is the second leading cause of death among women worldwide, and surgery is the mainstay of its treatment [1, 2]. Although marked progress was made in the past decade in the treatment of breast cancer, a significant proportion of women undergoing mastectomy experience significant postoperative pain [3, 4]. It has been estimated that approximately 40% of women experience severe acute pain after mastectomy, and of these, more than half develop chronic pain [5]. Analgesia based on regional anaesthesia and opioid-sparing techniques promotes superior perioperative results and faster recovery, reflecting in greater patient satisfaction, reduced morbidity, and reduced hospital costs [6–8].
Thoracic epidural anaesthesia has been the gold standard for perioperative analgesia in upper abdominal and chest surgeries, including breast procedures [9]. However, this strategy has important limitations, such as the need for the patient to be awake and cooperative. A significant risk of unintentional dural perforation and spinal cord neurological injury is another caveat of this technique. Complications such as haematoma, pneumothorax, and arterial hypotension have also been associated with thoracic epidural anaesthesia [5, 10, 11]. Therefore, many anaesthesiologists do not feel confident in using this anaesthetic approach [12].
Pectoral nerve block types I and II (PECS I/II) have been suggested as analgesic options for breast surgery. Inspired by the infraclavicular block approach, the PECS I/II procedure aims to provoke an anaesthetic blockade of the lateral and medial pectoral nerves, intercostobrachial nerves, the 4th, 5th, and 6th intercostal nerves, and the long thoracic nerves [12]. It is a reproducible and safe technique that optimises analgesia for chest wall procedures, with the advantage of being less invasive than thoracic epidural anaesthesia and with a lower risk of complications [13, 14].
Recent studies have reported a dose-dependent analgesic action of a local anaesthetic, suggesting that higher concentrations are more effective for perioperative analgesia [7, 15–17]. However, lite-rature on the short- and medium-term evaluation of the effects of this blockade in mastectomies is still scarce, and the few existing studies lack an adequate methodology, especially regarding the concentration of the local anaesthetic used. Therefore, the present study aimed to compare the efficacy and safety of PECS I/II block (using a higher dose of a local anaesthetic) with standard general anaesthesia in patients undergoing mastectomy.
METHODS
Study design and registration
This was a parallel, single-centre, single-blind, randomised trial. Blinding occurred at the participant level. The study was conducted at the Hospital de Base do Distrito Federal, a 750-bed reference hospital for tertiary care in Brasília, Distrito Federal, Brazil. All procedures followed the Declaration of Helsinki. The study was approved by the local Research Ethics Committee (Foundation for Education and Research in Health Sciences – Fundação de Ensino e Pesquisa em Ciências da Saúde, Brasília, Brazil) and registered on Plataforma Brasil (http://application.saude.gov.br/plataformabrasil) under the number 90611318.1.0000.5553. The study was also registered at ClinicalTrials.gov (NCT03966326). All participants provided written informed consent at the time of enrolment.
Participants
Procedures and interventions
General anaesthesia
All patients underwent a standardised general anaesthesia procedure. Specifically, after pre-anaes-thetic administration of midazolam, induction was performed with fentanyl, lidocaine, propofol, rocu-ronium, and maintenance with sevoflurane. Fentanyl bolus (1 mcg/kg) was administered when systolic blood pressure (SBP) or heart rate (HR) levels exceeded baseline values by 20%. Two investigators judiciously endorsed this conduct. Ephedrine (5 mg) was administered to increase SBP if it decreased below 90 mmHg, while atropine (0.5 mg) was given in case of bradycardia (HR < 50 beats per minute, bpm). After induction of general anaesthesia, patients assigned to the PECS II group were kept supine and had their arms abducted at 90°. Fentanyl was only given intraoperatively.
PECS I/II
We used ultrasound guidance (SonoSite M-Turbo, USA) in all PECS I/II procedures. More specifically, the high-frequency linear probe was positioned below the clavicle, in the deltopectoral grove parasagittally, pinpointing the pectoral muscles with the axillary artery and vein at the level of the first rib. Next, the probe was displaced distally to the second and third rib space, identifying the pectoralis major, pectoralis minor, and serratus muscles. Using the in-plane technique, we introduced the needle (UniPlex NanoLine, 22 G × 50 mm) between the pectoralis major and minor muscles and gave patients an injection of 10 mL of 0.5% ropivacaine. With the needle insertion into the interfacial plane of the pectoralis minor and serratus anterior, we gave patients an additional injection of 20 mL of 0.5% ropivacaine.
Standardised postoperative analgesic protocol
During the first 24 hours postoperatively, all patients with moderate pain (≥ 3 on the numerical rating scale) were given dipyrone (1 g intravenously [IV]) every 6 hours as the first analgesic. In case of inadequate pain control, tramadol (100 mg IV) was administered as a second analgesic every 6 hours. More specifically, tramadol was administered as needed after dipyrone if the patient had a pain score ≥ 3. We used tramadol because it is a widely used analgesic due to its efficacy and relatively low incidence of adverse effects. Tramadol has been included in the postoperative pain management guidelines at many institutions and is recommended for acute post-mastectomy pain relief [3]. Patients who experienced nausea and/or vomiting received ondansetron (8 mg IV) every 8 hours.
Outcomes
The primary outcome was pain intensity at rest 24 hours postoperatively, measured by a numerical rating scale (NRS) from 0 to 10, with 0 indicating the absence of pain and 10 indicating maximum or unbearable pain. We did not apply formal tests to check for cognitive impairment after surgery. Secondary outcomes included pain intensity at rest and under stress (movement). We evaluated secon-dary pain outcomes at 3 time points: at arrival from the post-anaesthetic recovery room (PACU), at discharge from the PACU, and after 12 hours postoperatively. We also assessed intraoperative mean arterial pressure (MAP), HR, intraoperative consumption of anaesthetics (estimated by the curve of the expired fraction of sevoflurane over time), and perioperative consumption of analgesics (estimated by the consumption of fentanyl, dipyrone, and tramadol). The time in minutes needed for patients to request analgesics was also evaluated. In addition, we assessed the length of stay in the PACU (in minu-tes) and hospital stay (in hours) and the following perioperative adverse events: arterial hypotension, arterial hypertension, tachycardia, bradycardia, nausea, or vomiting. The consumption of antiemetics as a dichotomous variable (yes/no) was also evaluated. We graded the degree of satisfaction of the surgical team using a 4-point Likert scale (dissatisfied, somewhat satisfied, satisfied, or very satisfied). We also graded the degree of bleeding in the surgical field, which was scored by the surgical team using a 6-point scale (0 = no bleeding; 1 = slight bleeding with no suction required; 2 = slight bleeding not treating the surgical site but requiring occasional suction; 3 = slight bleeding that improves for several seconds once suction has occurred; 4 = moderate bleeding hampering visualisation and requiring frequent suctioning; and 5 = severe bleeding requiring constant suctioning). At the end of the follow-up, the patients’ degree of overall satisfaction with perioperative care was also assessed using a 4-point Likert scale (dissatisfied, somewhat satisfied, satisfied, or very satisfied).
Randomisation, allocation concealment, and blinding
We randomised patients 1 : 1 to receive either PECS I/II or standard general anaesthesia (control). The random list was computer-generated via a web platform (www.randomizer.org). We maintained allocation concealment by keeping the allocation sequence inaccessible to all investigators during the recruitment, treatment, and follow-up phases. The investigator responsible for randomisation assigned each patient to one of the treatment groups and informed the anaesthesia team which group the patients belonged to when they arrived in the operating room. Blinding at the level of the surgery team/healthcare providers was not feasible due to ethical concerns because a sham procedure was deemed unacceptable. However, 2 assistant physicians (preceptor and resident) strictly followed the same anaesthesia protocol and procedures for all intraoperative procedures, to mitigate performance bias.
Calculation of sample size
We used data from our previous study conducted at the same institution [4]. Patients who received standard general anaesthesia based on opioids had a mean pain score of 4 (0 to 10 NRS) with a standard deviation of 1.9 in the first 24 hours postoperatively. Assuming a 35% reduction in pain scores, with a type I error of 5% and statistical power of 80%, 29 participants per group would be required. Due to possible losses to follow-up (estimated to be approximately 20%), 40 patients per treatment group were included (80 participants in total).
Statistical analysis
We evaluated the distributions of continuous variables using histograms and QQ plots, and checked normality with the Shapiro-Wilk test. Differences between groups for continuous variables with asymmetric distribution were examined with the Mann-Whitney U test. Variables with an asymmetric distribution were presented as medians (interquartile range, IQR). For variables with an approximately normal distribution, between-group differences were evaluated with Student’s t-test for independent samples. The latter variables were summarised as means (standard deviation, SD). Categorical variables were compared using Pearson’s χ2 with a correction for continuity. Categorical variables were expressed as absolute numbers (percentage). Mixed linear models evaluated continuous variables with repeated measures. Treatment group, time, and the interaction between treatment and time were considered fixed effects, and the model allowed a random intercept for each participant. All estimates were obtained by restricted maximum likelihood. The effects of the intervention were summarised as the mean difference (MD) along with a 95% confidence interval (95% CI) or relative risk (RR) with 95% CI. Statistical analyses were performed using SPSS for Macintosh (Statistical Package for the Social Sciences, Chicago, IL, USA) version 20.0, Stata 14 (StataCorp, TX, USA) and GraphPad Prism 7. A value of P < 0.05 (2 tailed) was considered statistically significant.
RESULTS
Between July 2018 and December 2019, we randomised 80 patients. Of the enrolled patients, 40 were randomly assigned to PECS I/II group and 40 to the control group. Ten patients in each group were lost to follow-up. Therefore, the analysis was based on 60 patients (n = 30 per group) (Figure 1). The baseline characteristics of the study population are shown in Table 1. No cases of postoperative cognitive dysfunction were detected.
TABLE 1
Clinical and sociodemographic characteristics of participants at baseline
Primary outcome
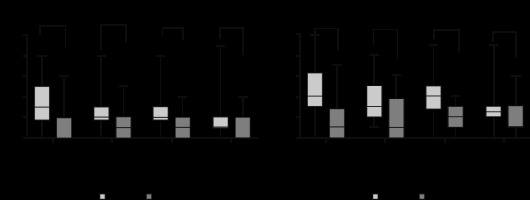
The median pain intensity (IQR) at rest (24 hours after surgery) was significantly lower in the PECS II group compared to the control group: 0 (0 to 1.75) vs. 1 (1 to 2), P = 0.021 (Figure 2).
Secondary outcomes
Pain
Similar results were observed concerning pain under stress (physical movement) (24 hours after surgery): median pain intensity was 1 (1 to 3) in the PECS I/II group vs. 2.5 (2 to 3) in the control group (P = 0.048). Overall, patients in the PECS I/II group had significantly lower pain levels than the control group from admission to the PACU until the first 24 hours postoperatively (Figure 2).
Consumption of analgesics and anaesthetics
Seven (23.3%) of the 30 patients in the PECS I/II group and 25 (83.3%) of the 30 patients in the control group required intraoperative fentanyl (RR: 0.28; 95% CI: 0.14–0.54; P = 0.0002). Furthermore, the mean (SD) intake of fentanyl in micrograms was about 4 times lower in the PECS I/II group: 30 (59.6) vs. 128.3 (103.95), P < 0.001.
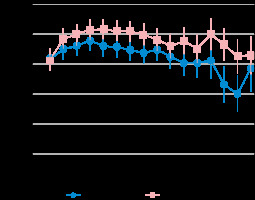
Patients in the PECS I/II group consumed less postoperative dipyrone (1650 mg [862.5] vs. 2550 mg [1003]; P < 0.001) and took longer to request it (401.78 minutes [238.1] vs. 162.75 minutes [169.1]), P < 0.001). Similar results were observed for postoperative tramadol consumption (Table 2). Considering the intraoperative period, the expired fraction of sevoflurane was statistically lower in the PECS I/II group compared to the control group (P for the global test of any difference between groups = 0.012). Statistically significant differences between groups occurred mainly between 1 to 2 hours and later between 3 and 4 hours (Figure 3).
TABLE 2
Secondary outcomes
[i] MD – mean difference, RR – relative risk, PONV – postoperative nausea, vomiting, or both, PACU – post-anaesthesia care unit. In Table 2, for continuous data, Student’s t tests were used. For categorical data, we calculated statistical significance using a Pearson’s χ2 with one degree of freedom (with a continuity correction when necessary).
FIGURE 3
Expired fraction (EF%) of sevoflurane in the intraoperative period. Results are presented as mean (95% confidence interval). Comparisons highlighted with * are statistically significant at the 5% alpha level (i.e. P = 0.020, 0.03, 0.014, 0.021, 0.021, and 0.033, respectively, from the left to the right). Comparisons highlighted with ** are statistically significant at the 0.5% alpha level (i.e. P = 0.0012 and 0.003, respectively)
Safety
The risk of postoperative nausea and/or vomiting was significantly lower in the PECS I/II group compared to the control group (RR: 0.23, 95% CI: 0.07–0.72, P = 0.012). Similar findings were observed for the frequency and amount of ondansetron use (Table 2).
Blood pressure and heart rate levels remained stable in both groups (Supplementary Figure S1), without clinically relevant differences. There was no statistically significant difference in the incidence of hypertension or hypotension, and bradycardia or tachycardia between the treatment groups (Table 2).
PACU time
The mean time (SD) in the PACU of patients in the PECS I/II group was statistically lower than the corresponding time in the control group: 132.4 minutes (49.6) vs. 162.9 minutes (45.4), P = 0.025. Participants in the PECS I/II group also had a shorter mean length of hospital stay (41.2 hours [13.4] vs. 45.1 hours [15.4], P = 0.30), although without statistical significance (Table 2).
Intraoperative bleeding
The surgical team graded the intraoperative bleeding volume as mild in 27 (90%) of 30 patients in the PECS I/II group and in 30 (100%) of the patients in the control group (P = 0.076, Supplementary Table S1). The surgical team satisfaction rate (very satisfied) was higher in the PECS I/II group (80% vs. 13.3%, P < 0.001), as well as the patients’ satisfaction (86.7% vs. 26.7%, P < 0.001) (Supplementary Table S2).
DISCUSSION
Main findings
The present randomised trial demonstrated that PECS I/II block using a high dose of local anaesthetic promotes lower perioperative pain scores 24 hours after mastectomy compared to standard general anaesthesia, as well as leading to reduced intraoperative and postoperative consumption of opioids. Overall, PECS I/II blockade proved to be equally safe as standard general anaesthesia, with no significant differences in haemodynamic and safety outcomes. PECS I/II significantly reduced sevoflurane consumption during surgery.
Comparison with previous studies
PECS I/II is indicated as an analgesic alternative to the thoracic epidural and paravertebral block (BPV) for chest wall and breast surgeries [12, 18–21]. The procedure targets the anaesthesia of the T2–T4 intercostal nerves, going up to T6, after administration of local anaesthetic between the pectoralis major and minor, and serratus muscles. The supine position, in which the block is performed, provides cranial and caudal dispersion of the local anaesthetic to the thoracodorsal, long thoracic, intercostobrachial, pectoral (medial and lateral), and T2–T6 intercostal nerves, which is confirmed by nuclear magnetic resonance images. When compared to other regional blocks, such as BPV or erector spinal block (ESP block), PECS I/II block has equal or greater analgesia potency for mastectomies [19, 22–24]. Furthermore, it has been suggested that PECS I/II block can lead to lower pain scores combined with an opioid-sparing effect.
While our findings corroborate previous reports, it is important to highlight that previous studies suggested that PECS I/II analgesia is more intense in the first 12 hours after surgery [15, 16]. However, our study employed the administration of 0.5% ropivacaine between the pectoralis major and minor muscles (10 mL) and between the pectoralis minor and serratus anterior muscles (20 mL), whereas previous reports used lower doses. For example, Bashandy et al. [16] used 0.25% bupivacaine without vasoconstrictor between the pectoralis muscles (10 mL) and between the pectoralis minor muscles and the serratus muscle (20 mL), while Versyck et al. [15] used 0.25% levobupivacaine in the same volumes. Thus, our findings indicate that higher doses of the local anaesthetic may provide analgesia up to 24 hours postoperatively without compromising the safety profile of PECS I/II block.
Our trial also provides unprecedented evidence that PECS I/II block can reduce the anaesthetics used for the maintenance of anaesthesia. However, Choi et al. [17] did not observe a reduction in propofol consumption when employing 0.5% ropivacaine to block PECS I/II. Because we maintained anaesthesia with sevoflurane, the anaesthetic-sparing effect may depend on the anaesthetic agent and its concentration. The lower consumption of general anaesthetic was concomitant with reduced intraoperative opioid use, consistent with previous studies employing PECS II [16] and PECS I [21] block for mastectomies. This effect, nonetheless, was not observed by Versyck et al. [15]. That study did not take into account the type of mastectomy performed (partial or total) and the presence or absence of axillary clearance in their analyses, which may have introduced significant biases in the outcomes evaluated.
Despite the higher dose of local anaesthetic used in our study than in prior reports [15, 16], our findings corroborate previous evidence that PECS I/II block is associated with a lower incidence of postoperative nausea and vomiting, decreasing the use of ondansetron. This effect is likely to be due to the reduced consumption of opioids and inhaled anaesthetics. Nausea and vomiting were identified as more unpleasant postoperative effects than pain [25], related to a series of common risk factors in patients undergoing mastectomy [26]. Thus, the reduction of these postoperative effects may reflect great clinical benefits for this group of patients. In fact, consistent with a previous study [16], the length of stay in the PACU of patients who received PECS I/II block was shorter than for the control counterparts. Besides optimised analgesia, and reduced opioid consumption and incidence of adverse events, this effect may be associated with the absence of sympathetic and motor nervous blocks, another advantage over paravertebral and epidural blocks [27].
While a shorter length of stay has been previously reported [16], we observed a hospital stay only 3 hours shorter in the PECS I/II block group compared to the control group. However, all patients hospitalised for mastectomy are discharged from the hospital within the same period of the following day in our service, regardless of the shift in which the surgery was performed on the previous day, which may have introduced a bias. The degree of overall satisfaction with the perioperative experience was also higher in patients who received regional anaesthesia. Despite being an outcome with subjective assessment, this finding may reflect the superior analgesic effect observed because pain and discomfort are identified as the most important factors in the quality of postoperative recovery [28].
LIMITATIONS
A major limitation of our study is the lack of blinding at the level of the surgery team/healthcare providers. As recommended by the Ethics Committee, patients in the control group did not receive a PECS I/II sham because the administration of an inactive substance (e.g. 0.9% saline solution) in the blockade planes would only confer additional risks. However, we followed strict and carefully standardised protocols to mitigate performance bias, and the researcher who evaluated the patients postoperatively was unaware of the group to which the participants were allocated. Furthermore, partial block failures were not included in the analysis because they were performed after induction of general anaesthesia. Despite this, pain scores in the first 24 hours were lower in the PECS I/II group. In addition, we changed the measurement approach for our primary outcome. While the initial protocol for pain assessment was based on the visual analogue scale (VAS), all assessments were performed using a numeric rating scale (NRS). Recent evidence suggests that patients, particularly those with less education, with cancer-related pain prefer NRS over VAS [29]. A remarkably high agreement was reported between these 2 tools, suggesting that the change in pain assessment did not impact our main findings [30].
CONCLUSIONS
In summary, our findings indicate that the use of a high dose of local anaesthetic in PECS I/II block can reduce 24-hour postoperative pain intensity compared to standard general anaesthesia for patients undergoing mastectomy, without increasing the incidence of adverse events. Although the pain reduction benefits of PECS block after 24 h may be small, the observed effects are still in the range of a clinically important improvement for acute postoperative pain [31]. PECS I/II was also associated with a statistically significant reduction in sevoflurane consumption during surgery. Currently, long-term postoperative events, such as the incidence, intensity, and risk factors of post-mastectomy pain syndrome, are being evaluated and will contribute to a better understanding of the clinical effects of this anaesthetic approach.