Dear Editor,
We would like to present a case of successful implementation of venovenous extracorporeal membrane oxygenation (ECMO) in a COVID-19 convalescent. Many experts suggest that during a pandemic ECMO should be applied in strictly defined cases for COVID-19 patients, mainly because of the resource-consuming nature of extracorporeal therapy [1, 2]. Current guidelines state that ECMO is contraindicated after seven days of mechanical ventilation, including in critically ill COVID-19 patients [3]. Extracorporeal treatment in our COVID-19 convalescent was launched at the late stage of severe acute respiratory distress syndrome (ARDS), which was also affected by the onset of septic shock. We believe that this is the first case of ECMO therapy in a COVID-19 convalescent to be described in the literature. Written informed consent from the patient was obtained to present this case.
A 28-year old, previously healthy man was referred to the ECMO centre by the Intensive Care Unit (ICU) of the regional hospital. The patient had been mechanically ventilated due to acute respiratory failure for 12 days.
Before admission to the ICU, he had been treated in an isolation ward because of symptoms of dyspnoea, coughing, and fever, which slowly escalated seven days before hospitalization. At the isolation ward, a qualitative antibody IgG/IgM SARS-CoV-2 rapid test was positive, and a viral test from a nasopharyngeal swab (SARS-CoV-2 RT-PCR test) yielded ambiguous results (only nucleocapsid of the virus was detected). The next two viral tests from a nasopharyngeal swab performed were negative.
Because of respiratory deterioration the patient was then transferred to the ICU. Laboratory tests in the ICU on the admission day showed procalcitonin (PCT) of 0.2 mg L−1, C-reactive protein (CRP) of 122 mg L−1, and white blood cells (WBCs) 8.55 G L−1. The SARS-CoV-2 RT-PCR test from bronchoalveolar lavage performed in the ICU was negative, but the quantitative antibody SARS-CoV-2 test revealed an IgG titre of 10.18 (positive value > 1.1) and IgM titre of 2.835 (positive value > 1.1). The epidemiological history of the patient was eminently positive – the rest of his family from the same household had been positively diagnosed with COVID-19. For the above reasons, the patient in the ICU was treated as a COVID-19 convalescent.
In the ICU, the patient was ventilated using a tidal volume below 6 mL kg−1 of predicted body weight, with a high ratio of inspired oxygen fraction (FiO2). The specific parameters of mechanical ventilation are presented in Table 1. Prone positioning and neuromuscular blocking agents were used only at the beginning of the course and did not improve the patient’s ventilatory status. On day 11, desaturation of arterial blood occurred alongside arterial hypotension. The peripheral blood for microbiological tests was collected (methicillin-resistant Staphylococcus hominis and methicillin-resistant S. epidermidis were detected two days later). The patient fulfilled the criteria of severe ARDS according to the Berlin Definition of ARDS, with his current arterial pO2 of 53 mm Hg, FiO2 of 1.0 and positive end-expiratory pressure (PEEP) of 12 cm H2O. At that stage, the patient was started on an infusion of noradrenaline at a dose of 0.2 μg kg−1 min−1 and was referred to the ECMO centre.
TABLE 1
Respiratory parameters during mechanical ventilation before ECMO
The mobile ECMO team from the ECMO centre assessed that the patient required veno-venous ECMO support. The patient’s Murray score was 3.5, with a RESP score of 3. A transthoracic echocardiogram (TTE) showed good cardiac contractility without signs of right heart pressure overload. Cannulas were inserted percutaneously into femoral veins under real-time ultrasound guidance. The blood flow during ECMO was set at 6.5 L min−1, with a sweep gas flow of 7 L min−1. Immediately after ECMO implementation, the mobile ECMO team transferred the patient to the ECMO centre.
In the ECMO centre, veno-venous ECMO was continued and mechanical ventilation was adjusted with FiO2 0.4, a PEEP of 15 cm H2O, and a driving pressure of 14 cm H2O. A microbiological test of the blood was performed once again. Broad-spectrum antibiotic therapy (meropenem and vancomycin) was terminated when the results proved to be negative. Tracheostomy was performed on day 3, the level of sedation was reduced, and physiotherapy was intensified. A daily TTE confirmed the correct cardiac function, and administration of norepinephrine was stopped on day 4. The SARS-CoV-2 RT-PCR tests were negative twice. No complications of extracorporeal therapy were observed. Anticoagulation during ECMO was managed by the use of unfractionated heparin, maintaining partial prothrombin time at the value of around 100 seconds. ECMO therapy was terminated on day 10, and the patient was finally weaned from the ventilator two days later. Only slight symptoms of neuromuscular weakness were observed during the following days. Computed tomography scans of the patient’s lungs revealed significant improvement (see Figure 1). Three weeks after ECMO discontinuation, the patient finally returned home breathing entirely independently without relevant neurologic dysfunction.
FIGURE 1
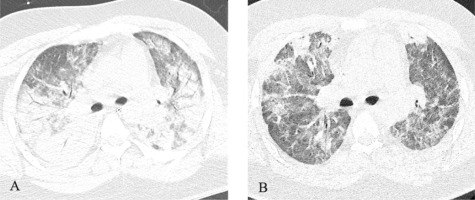
Computed tomography (CT) scans of the lungs. A – CT performed 3 days before ECMO implementation. B – CT performed 4 days after decannulation from ECMO
In this patient, a new bacterial septic shock had been superposed on previously damaged lungs, affected by viral infection with COVID-19. Although our patient was assessed at the late phase of a difficult mechanical ventilation, we decided to deploy extracorporeal therapy, because data describing the evolution of the alterations in the lungs of critically ill COVID-19 convalescents are scarce. Moreover, it was important that the patient’s decompensation seemed to be caused by a new superinfection, which was ultimately confirmed in the ECMO centre.
The Extracorporeal Life Support Organization (ELSO) states that mechanical ventilation with high values of plateau pressure and FiO2 for over seven days is a contraindication for veno-venous ECMO [3]. Hence, in ARDS caused by SARS-CoV-2 infection, ECMO is implemented early. Yang et al. reported that the procedure was usually started after 36 hours of mechanical ventilation [4]. Huette et al. reported a median time of 84 hours of mechanical ventilation before ECMO [5]. Experts suggest that contraindications for ECMO implementation should be weighed flexibly in the COVID-19 pandemic [6].
None of the six viral tests performed during the patient’s hospitalization in various wards was clearly positive. Additionally, an antibody SARS-CoV-2 test revealed a high value of IgG titre, suggesting that the patient had recovered from the acute phase of COVID-19 [7]. In theory, we cannot exclude the possibility of false negative results of viral tests. Despite this, the number of tests (including the SARS-CoV-2 RT-PCR test from bronchoalveolar lavage, which has higher sensitivity and specificity) conducted in various medical wards seems to be sufficient to minimise the risk of false negative results.
Little is known about the clinical picture of COVID-19 convalescents treated in intensive care settings. Two phenotypes of injured lungs have been proposed [8]. Other organs are also affected and the treatment in SARS-CoV-2 infection is only supportive [9–11]. Available reports tend to focus on the final effect of the treatment – i.e. whether the patient was discharged alive. To date, only single long-term follow-ups of COVID-19 convalescents discharged from ICUs have been performed [12]. Hence, decisions regarding application of extracorporeal therapy in COVID-19 convalescents should be taken very cautiously. Age and the presence of chronic comorbidities should be critical criteria of paramount importance [13].




