Introduction
Lumbar degenerative diseases (LDD), which include lumbar spinal stenosis, lumbar disc herniation, spondylolisthesis, and lumbar instability, are common causes of back and leg pain [1–3]. Transforaminal lumbar interbody fusion (TLIF) is commonly used for patients with LDD and the purposes of TLIF are to relieve the symptoms and improve the quality of life [4–6]. Nevertheless, the classical open TLIF is correlated with iatrogenic injury of the paraspinal muscle, resulting in intractable postoperative low back pain [7]. At present, minimally invasive TLIF (MIS-TLIF) is widely used to minimize the soft tissue injury and intraoperative blood loss [8]. MIS-TLIF has shown significantly less blood loss compared with open TLIF [9]. However, MIS-TLIF is usually restricted by a limited working space and it is challenging to visualize deep surgical fields through the tubular retractor [10].
To overcome MIS-TLIF shortcomings, percutaneous endoscopic TLIF (PE-TLIF) has been commonly used for patients with LDD [11–13]. PE-TLIF makes possible a complete endoscopic discectomy, spinal canal and foramina decompression, and interbody fusion via the endoscopic and working portal [14–17]. Although numerous earlier investigations explored the relative efficacies of PE-TLIF and MIS-TLIF in treating LDD [11–18], most of these studies were retrospective in nature. Since multiple factors can sway the outcomes of a retrospective investigation, and introduce unintentional bias, a meta-analysis is recommended to extensively evaluate relevant literature, reduce bias risk, and enhance the overall statistical power of the collective study outcomes.
Aim
Herein, our goal was to compare the safety and clinical effectiveness of PE-TLIF and MIS-TLIF in treating LDD.
Material and methods
Study selection
Our research abided by the guidelines of the Preferred Reporting Items for Systematic reviews and Meta-Analyses [18], and is registered at https://inplasy.com/ (Number: INPLASY202220090).
We screened for relevant publications in scientific databases, namely, PubMed, Embase, Cochrane Library, Wanfang, VIP, and CINK from the date of database establishment to November 2021. Our search terminologies were as follows: ((Endoscopic Lumbar Interbody Fusion) OR (Endo-LIF)) AND ((Minimally Invasive Transforaminal Lumbar Interbody Fusion) OR (MIS-TLIF)).
The following criteria were used to select relevant articles for analysis:
Studies with the following criteria were eliminated from the analysis: (a) single-arm investigations; (b) non-human investigations; and (c) studies without an English title and/or abstract.
Data accumulation
Two separate authors screened eligible publications and collected baseline study data, namely, author, year of publication, country of publication, study format, and quality assessment; and patient data, namely, population size, age, gender, disk range, body mass index (BMI), and follow-up duration; and many treatment-related data. Disagreements were rectified through consultation with a third author.
Quality evaluation
Randomized controlled trials (RCTs) were evaluated using the Cochrane risk of bias tool for the potential bias in performance, attrition, detection, screening, reporting, and so on. Non-RCTs were analyzed via the 9-point Newcastle-Ottawa scale (NOS) for potential selection bias, namely, selection (4 points), comparability (2 points), and exposure (3 points), carrying either high (≥ 7), moderate (4–6), or low (< 4) risk of bias [19].
Endpoints
The endpoints of this meta-analysis included visual analog scale (VAS)-leg, VAS-back, Oswestry Disability Index (ODI), fusion rate, surgical duration, blood loss, complication rates, and postoperative hospitalization.
Statistical analysis
RevMan v5.3 and Stata 12.0 were employed in this study. Dichotomous variables were accumulated depending upon odds ratios (ORs) with 95% confidence intervals (CIs), while continuous variables are accumulated depending upon mean difference (MD) with 95% CIs. Heterogeneity was examined via I2 tests, with I2 > 50% representing marked heterogeneity. Random-effects models were used to analyze marked heterogeneity, while fixed-effects models were used to analyze marked homogeneity. Heterogeneity sources are analyzed through sensitivity assessment. Funnel plot and Egger test are employed for evaluating publication bias risks.
Results
Included studies
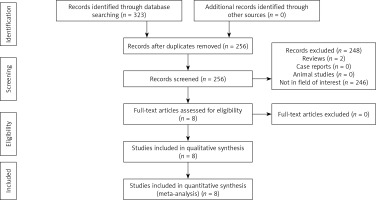
We initially found 323 relative studies by using the research strategy. After step-by-step selection, a total of 8 studies were eligible for analysis (Figure 1, Table I). Seven studies were retrospective [12–18], and 1 study was prospective [11]. Seven studies were from China [11, 12, 14–18], and 1 study was from South Korea [13].
Table I
Baseline data of the included studies
| First author | Year | Countries | Design | Newcastle-Ottawa scale |
|---|---|---|---|---|
| Ao [11] | 2020 | China | Prospective | 8 |
| Dong [12] | 2019 | China | Retrospective | 8 |
| Kim [13] | 2021 | South Korea | Retrospective | 7 |
| Li [14] | 2020 | China | Retrospective | 8 |
| Wen [15] | 2020 | China | Retrospective | 7 |
| Xue [16] | 2021 | China | Retrospective | 7 |
| Zhang [17] | 2021 | China | Retrospective | 8 |
| Zhao [18] | 2021 | China | Retrospective | 7 |
In these 8 included studies, 229 patients underwent PE-TLIF and 258 patients underwent MIS-TLIF (Table II). The mean age, gender ratio, and mean BMI were comparable between PE-TLIF and MIS-TLIF groups in the analyzed studies. The NOS of these studies ranged between 7 and 8.
Table II
Patients’ details in each study
| Authors [ref.] | Disease types | Disk range | Groups | Number of patients | Age [years] | M/F | BMI | Follow-up [months] |
|---|---|---|---|---|---|---|---|---|
| Ao [11] | Degenerative spondylolisthesis | L3-S1 | PE-TLIF | 35 | 52.80 | 16/19 | 24.73 | 12 |
| MIS-TLIF | 40 | 53.68 | 22/18 | 25.08 | 12 | |||
| Dong [12] | Disc herniation, Spondylolisthesis, Spinal stenosis | L3-S1 | PE-TLIF | 28 | 58.3 | 17/11 | 23.3 | 24 |
| MIS-TLIF | 25 | 54.8 | 9/16 | 23.0 | 24 | |||
| Kim [13] | Degenerative/lytic spondylolisthesis | L2-S1 | PE-TLIF | 32 | 70.5 | 17/15 | Unknown | 27.2 |
| MIS-TLIF | 55 | 67.3 | 25/30 | Unknown | 31.5 | |||
| Li [14] | Disc herniation, Spondylolisthesis, Spinal stenosis | L4-S1 | PE-TLIF | 22 | 52.0 | 12/10 | Unknown | 14.9 |
| MIS-TLIF | 30 | 50.7 | 18/12 | Unknown | 14.7 | |||
| Wen [15] | Not given in detail | L4-S1 | PE-TLIF | 20 | 48.33 | 13/7 | Unknown | 12–20 for all |
| MIS-TLIF | 20 | 50.77 | 11/9 | Unknown | ||||
| Xue [16] | Not given in detail | L3-5 | PE-TLIF | 20 | 46.3 | 11/9 | Unknown | 16.1 |
| MIS-TLIF | 20 | 48.4 | 12/8 | Unknown | 15.8 | |||
| Zhang [17] | Degenerative/isthmic spondylolisthesis | L3-S1 | PE-TLIF | 32 | 53.1 | 12/20 | 25.5 | 12 |
| MIS-TLIF | 30 | 55.7 | 14/16 | 24.9 | 12 | |||
| Zhao [18] | Not given in detail | L3-S1 | PE-TLIF | 40 | 56.93 | 37/17 | Unknown | 24 |
| MIS-TLIF | 38 | 57.01 | 20/18 | Unknown | 24 |
Improvement of VAS-leg
Six studies compared the VAS-leg before and after treatment [11–14, 16, 17]. The pooled ΔVAS-leg values are comparable between the 2 groups (MD = –0.31; 95% CI = –0.95–0.33; p = 0.35, Figure 2 A). Significant heterogeneity is found for this endpoint (I2 = 98%). Sensitivity analysis suggests that removing individual studies has no impact on the detected heterogeneity. No obvious publication bias is observed (Egger test, p = 0.597).
Figure 2
Pooled results of: A – improvement of VAS-leg, B – improvement of VAS-back, C – improvement of ODI, D – postoperative analgesic, E – fusion rates, F – operation time, G – intra-operative fluoroscopic time, H – intra-operative blood loss, I – length of incision, J – complication rates, K – time to ambulation, L – hospital stay

Improvement of VAS-back
Six studies compared the VAS-back before and after treatment [11–14, 16, 17]. The pooled ΔVAS-back value is significantly higher in the PE-TLIF group (MD = 1.62; 95% CI: 0.92–2.32; p < 0.00001, Figure 2 B). Significant heterogeneity is found for this endpoint (I2 = 98%). Sensitivity analysis suggests that removing individual studies has no impact on the detected heterogeneity. No obvious publication bias is observed (Egger test, p = 0.188).
Improvement of ODI
Six studies compared the ODI before and after treatment [11–14, 16, 17]. The pooled ΔODI values are comparable between the 2 groups (MD = 3.82; 95% CI: –1.53–9.18; p = 0.16, Figure 2 C). Significant heterogeneity is found for this endpoint (I2 = 98%). Sensitivity analysis suggests that removing individual studies has no impact on the detected heterogeneity. No obvious publication bias is observed (Egger test, p = 0.074).
Postoperative analgesic
Two studies reported the dose of postoperative analgesic [11, 12]. The pooled dose of postoperative analgesic is comparable between the 2 groups (MD = –32.45; 95% CI: –82.74–17.83; p = 0.21, Figure 2 D). Significant heterogeneity is found for this endpoint (I2= 99%). Sensitivity analysis cannot be performed because there are only 2 studies. The funnel plot does not reveal any publication bias.
Fusion rates
Seven studies reported the fusion rates after treatment [11–14, 16–18]. The pooled fusion rates are comparable between the 2 groups (90.4% vs. 90.3%; p = 0.86, Figure 2 E). No significant heterogeneity is found for this endpoint (I2= 0%). No obvious publication bias is observed (Egger test, p = 0.797).
Operation time
All studies reported the operation time. The pooled operation time is significantly lower in the MIS-TLIF group than in the PE-TLIF group (MD = 22.41; 95% CI: 6.48–38.34; p = 0.006, Figure 2 F). Significant heterogeneity is found for this endpoint (I2= 95%). Sensitivity analysis suggests that removing individual studies has no impact on the detected heterogeneity. We observed marked publication bias (Egger test, p = 0.049).
Intra-operative fluoroscopic time
Two studies reported the intra-operative fluoroscopic time [12, 17]. The pooled intra-operative fluoroscopic time is significantly lower in the MIS-TLIF group than in the PE-TLIF group (MD = 14.18; 95% CI: 12.07–16.30; p < 0.00001, Figure 2 G). No significant heterogeneity is found for this endpoint (I2 = 0%). The funnel plot does not reveal any publication bias.
Intra-operative blood loss
Seven studies reported on the intra-operative blood loss [11, 12, 14–18]. The pooled intra-operative blood loss is drastically lower in the PE-TLIF group than in the MIS-TLIF group (MD = –77.48; 95% CI: –127.05–27.92; p = 0.002, Figure 2 H). Significant heterogeneity is found for this endpoint (I2 = 99%). Sensitivity analysis suggests that removing individual studies has no impact on the detected heterogeneity. We observed marked publication bias (Egger test, p = 0.021).
Length of incision
Three studies reported the length of incision [15–17]. The pooled length of incision is significantly lower in the PE-TLIF group than in the MIS-TLIF group (MD = –1.14; 95% CI: –1.74–0.55; p = 0.0002, Figure 2 I). Significant heterogeneity is found for this endpoint (I2 = 78%). The significant heterogeneity disappears (I2 = 0%) when removing Xue’s study [16]. No obvious publication bias is observed (Egger test, p = 0.683).
Complication rates
Six investigations reported the complication rates after treatment [11, 12, 14–17]. The collective complication rates are similar between the 2 groups (5.9% vs. 7.0%; p = 0.60, Figure 2 J). No significant heterogeneity is found for this endpoint (I2 = 0%). No marked publication bias is observed (Egger test, p = 0.733).
Time to ambulation
Four studies reported the data of time to ambulation [12, 13, 15, 17]. The poled time to ambulation is significantly lower in the PE-TLIF group than in the MIS-TLIF group (MD = –0.40; 95% CI: –0.63–0.17; p = 0.0006, Figure 2 K). Significant heterogeneity is found for this endpoint (I2 = 75%). The significant heterogeneity disappears (I2 = 0%) when removing Kim’s study [13]. No marked publication bias is observed (Egger test, p = 0.665).
Hospital stay
Five studies reported the data of time to ambulation [11, 13, 14, 16, 17]. The poled hospital stay time is significantly lower in the PE-TLIF group than in the MIS-TLIF group (MD = –3.03; 95% CI: –4.77–1.29; p = 0.0007, Figure 2 L). Significant heterogeneity is found for this endpoint (I2 = 96%). Sensitivity analysis suggests that removing individual studies has no impact on the detected heterogeneity. No marked publication bias is observed (Egger test, p = 0.400).
Discussion
This meta-analysis compared the clinical efficacy between PE-TLIF and MIS-TLIF for patients with LDD. The purpose of PE-TLIF and MIS-TLIF treatments for LDD is relieving the pain and enhancing quality of life. All the included studies found that VAS-leg, VAS-back, and ODI could be significantly improved by both PE-TLIF and MIS-TLIF. Our meta-analysis reveals that the degree of improvement of VAS-leg and ODI is comparable between PE-TLIF and MIS-TLIF. Furthermore, the need for a postoperative analgesic is also comparable between the 2 groups. These findings may indicate that both PE-TLIF and MIS-TLIF can achieve appropriate clinical effectiveness in patients with LDD. However, the PE-TLIF may achieve a faster recovery of back pain than MIS-TLIF does. This finding may be attributed to the fact that PE-TLIF intervention is associated with reduced surgical trauma to surrounding soft and bone tissues, compared to the MIS-TLIF intervention [16].
Fusion rate is also an important endpoint in this meta-analysis. We found that the collective fusion rate of PE-TLIF is comparable to MIS-TLIF, at approximately 90%. Hence, both PE-TLIF and MIS-TLIF achieve suitable interbody fusion. However, Ao et al. [11] found that MIS-TLIF can achieve a significantly higher fusion rate than PE-TLIF. This finding may suggest inadequate bone graft and expandable cage application [10]. Nonetheless, the results from the retrospective study should be further proven by RCTs.
The pooled operation and intra-operative fluoroscopic time are both significantly higher in the PE-TLIF group. The curette-mediated endplate preparation in PE-TLIF took a considerable amount of time. Since it relies on instrument palpations, without direct vision, and with sequential endoscopic guidance, the endplate preparation required more time than MIS-TLIF [20–22].
Even though PE-TLIF is usually time consuming, it can result in significantly less intra-operative blood loss and better post-operative recovery. These results may be attributed to the shorter length of incision during PE-TLIF.
This meta-analysis shows comparable pooled complication rates between the 2 groups. Furthermore, the pooled complication rates after PE-TLIF and MIS-TLIF are only 5.9% and 7.0%, respectively. These findings indicate that both PE-TLIF and MIS-TLIF are safe for patients with LDD. If some patients experience the severe complication that is an abscess, external drainage is an effective method to treat it [23].
A similar meta-analysis reported insights into unilateral bi-portal endoscopy (UBE) in the treatment of lumbar diseases [24]. The researchers found that UBE surgery could significantly relieve the VAS scores of leg and back [24]. However, that meta-analysis only included single-arm studies [24]. Therefore, we could not find results about the comparison of UBE with other techniques. Our meta-analysis contained 2 commonly used techniques, and this is an advantage over the previous meta-analysis.
Our meta-analysis faced certain limitations. First, our analysis did not include any RCT. Furthermore, the multiple types of diseases and different disk ranges also increase the risk of bias. Therefore, further RCTs should be conducted. Second, there was a lack of homogeneity in surgical interventions and number of channels, which may influence our results. Many endpoints in this meta-analysis demonstrate significant heterogeneity. Third, there is a lack of cost-effective analysis among the included studies. Fourth, all eligible investigations were based in Asia. Therefore, additional comprehensive, global studies are warranted once stent usage becomes more prevalent worldwide.