An aberrant right subclavian artery (ARSA, arteria lusoria) is the most common anomaly or variant of a left-sided aortic arch, with a prevalence of 0.1–1%. It originates distal to the left subclavian artery. Knowledge of cardiovascular anatomy is crucial during orthotopic heart transplantation (OHT) planning, as well as during follow-up interventional procedures such as coronary angiography through the right radial artery (RRA).
To our knowledge, this is the first systematic assessment of the prevalence of ARSA among OHT recipients, beyond individual (four) case reports (Mrochek AG et al., Surg Radiol Anat. 2019; Schwein A et al., Ann Vasc Surg. 2015; Shu S et al., Interact Cardiovasc Thorac Surg. 2022; and Sebastian VA et al., J Card Surg).
We screened 541 OHT recipients. Among them, 257 patients had undergone at least one chest computed tomography (CT) scan. ARSA was identified in two of these patients, resulting in a prevalence of 0.78% (2/257) among those with chest CT imaging.
Patient 1. This patient underwent OHT at the age of 32 due to end-stage heart failure (HF) caused by dilated cardiomyopathy. The procedure was preceded by 18 days of circulatory support with a biventricular assist device. Chest CT performed prior to OHT revealed ARSA (Figure 1 A), as well as moderate pulmonary embolism. Additionally, coronary angiography performed through RRA was complicated by RRA occlusion, which was managed conservatively. During 4 years of follow-up, the patient underwent one further coronary angiography (through transfemoral access) and remained in a stable condition.
Figure 1
Computed tomography angiography of the thoracic aorta (volume-rendered reconstruction). White arrows indicate the aberrant right subclavian artery. A – Patient 1; B – Patient 2
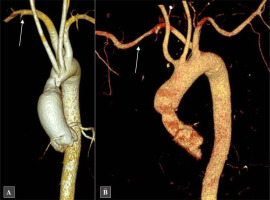
Patient 2. This patient underwent OHT at the age of 54 due to end-stage HF resulting from ischemic cardiomyopathy. A chest CT performed 2 weeks after OHT revealed ARSA (Figure 1 B) and a retrosternal hematoma, which required surgical evacuation via rethoracotomy. Prior to OHT, the patient had undergone one coronary angiography and two percutaneous coronary interventions (PCI) of the left anterior descending artery (LAD) – all through the femoral artery. Over the subsequent 10 years of follow-up, the patient underwent four coronary angiographies (one through the RRA) and one PCI of the LAD via the left radial artery.
To our knowledge, this is the first report to systematically assess the prevalence of ARSA in a larger cohort of OHT recipients. Previous publications were limited to isolated case reports, lacking broader implications or follow-up data. Our report offers several practical insights.
First, since OHT recipients are at increased risk of developing coronary artery vasculopathy, they require regular assessment of the coronary tree using invasive coronary angiography or coronary CT angiography. The presence of ARSA poses a challenge for coronary angiography and PCI through the RRA due to the tortuous course of the aberrant vessel. Both of our patients underwent multiple coronary catheterizations, including procedures through the RRA. One such procedure was complicated by RRA occlusion (not necessarily related to ARSA). Nonetheless, several reports of iatrogenic injury to the ARSA during coronary catheterization via the RRA have been published [1–4].
Second, ARSA can cause tracheobronchial compression, reported in approximately 10% of ARSA cases. Several case reports have described the development of subclavian–esophageal fistulae in the setting of ARSA, leading to massive upper gastrointestinal bleeding, particularly following tracheal or esophageal manipulation after cardiac surgery (although not reported after OHT) [5].
Finally, unlike previous case reports, this study provides the first prevalence estimate of ARSA in OHT patients, along with long-term procedural and clinical outcomes, offering guidance for future diagnostic and interventional strategies.







