Chylothorax is a rare condition characterized by accumulation of chyle from the lymphatic system within the pleural cavity. It occurs when the thoracic duct or one of its branches is damaged, disrupted, compressed, or obliterated, finally resulting in leakage to the body cavities. Patients most commonly experience breathing difficulties and chest pressure. However, if chyle accumulation is moderate, no alarming symptoms are visible, as the respiratory system can gradually adapt to the increasing fluid volume [1]. Although rare, chylothorax is a potentially severe condition, which arises from traumatic, non-traumatic, or idiopathic causes. To differentiate chylothorax from other thoracic pathologies, further evaluation such as thoracic ultrasound, chest radiography, computed tomography (CT) scan, magnetic resonance imaging (MRI) or conventional lymphangiography may be helpful [1]. Chylothorax management may be very difficult and complex. Therefore, a careful treatment approach and proper diagnosis are crucial to prevent further complications.
A 55-year-old man was admitted to our clinic on October 31st 2024 in a moderate to severe general condition due to intensified dyspnea and lack of physical activity tolerance. From July to September 2024 the patient was treated for pneumonia and pleuritis and given antibiotics. At that time, thoracic radiography revealed the presence of fluid in the pleura. He was transferred from a pulmonological ward in another hospital with a diagnosis of bilateral pleural effusion of chylous nature and right-sided post-thoracentesis pneumothorax. The patient was suspected to have thoracic duct injury. A CT scan did not reveal any pathologies explaining the symptoms’ etiology. In October, the patient was hospitalized and evaluated by a cardiologist, who excluded a cardiological cause of pleural effusion or dyspnea. Finally, 2 days before he was transferred to our clinic, the patient was admitted to the Emergency Room in the previous hospital, where he lost consciousness during pleural fluid drainage (approximately 20 ml of fluid was drained).
Following the patient’s admission to our clinic, a repeat thoracentesis of the right pleural cavity was performed, and approximately 1.5 l of chyle was evacuated. Conservative treatment was initiated, including empirical antibiotic therapy, fluid therapy, a strict diet, and parenteral nutrition. Despite this management, there was no significant decrease in daily lymphatic drainage from the right pleural cavity, which remained between 500 and 1000 ml/day. Given the persistent drainage, the patient underwent medical thoracoscopy for further diagnostic evaluation.
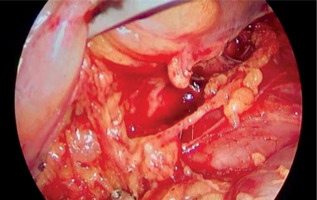
On November 7th 2024, the surgery was performed via right-sided video-assisted thoracoscopic access (VATS), a pleural biopsy was taken, and a wedge resection of a nodule in the lower lobe was performed. No obvious cause of the chylothorax was identified. Therefore, it was decided to ligate the thoracic duct just above the diaphragm (Figure 1). During the postoperative period, there was no significant reduction in chyle output, with drainage volumes remaining at a similar level – 500–1000 ml. Cytological examination of the pleural fluid was performed twice, in November and December; in both cases, no malignant cells were detected. A CT scan of the thoracic and abdominal cavity was performed, revealing the presence of low-density fluid in the left pleural cavity, measuring 3 cm in width, along with atelectatic changes in the adjacent lung tissue. Surgical clips from previous thoracic duct clipping were visible. Additionally, a small amount of fluid was detected in the abdominal cavity around the splenic margin. A CT scan of the pelvis did not show any abnormalities. A hematology consultation revealed no evidence of lymphoproliferative or myeloproliferative disorders. During an internal medicine consultation, a suspicion of a hospital infection was raised. On auscultation, crackles were heard on the left side, and decreased breath sounds were noted in the basal region on the right. It was recommended to initiate treatment with piperacillin/tazobactam. Infectious disease diagnostics were negative for syphilis, Cryptococcus, Aspergillus, and Candida. In the following postoperative days, a gradual deterioration of the patient’s general condition was observed. Staphylococcal sepsis and pneumonia were diagnosed. The patient was transferred to the ICU for further treatment due to a drop in blood pressure and sudden circulatory failure. During the ICU stay, antibiotic therapy was continued according to the protocol for managing patients with Staphylococcus aureus bacteremia. The patient required drainage of the left pleural cavity, as well as additional drainage of the right pleural cavity. Ultrasound of the jugular veins revealed a past thrombosis in the left internal jugular vein, collateral circulation, and a thrombus at the junction of the right subclavian vein.
Following angiology consultation, lymphangiography was recommended to identify the source of chylous leakage. On December 2nd, the histopathological results of the lesion from the lower lobe and the pleural biopsy were received. The findings revealed inflammatory-related atypia, fibrosis, and emphysema. Immunohistochemical (IHC) staining showed calretinin (+), CK 5/6 (+), BAP (+), and MT AP – inconclusive.
On February 4th 2025, MR lymphangiography without contrast was performed. The examination revealed signs of thoracic duct injury with the formation of multiple pathological, encapsulated lymphatic collections in the right posterior mediastinum and the right pleural cavity, as well as evidence of leakage into the left pleural cavity. The next day, redrainage of the right pleural cavity was performed, evacuating approximately 1000 ml of fluid. A significant improvement in the patient’s general condition and resolution of dyspnea were observed. However, in February 2025 due to continued persistent chyle accumulation and malaise, the patient underwent further thoracic duct ligation in Germany. Afterwards, further MR lymphangiography with contrast was performed. The preliminary diagnosis was made, establishing the presence of generalized lymphatic anomaly (GLA). GLA is a rare disorder caused by abnormal formation and proliferation of lymphatic vessels, which can infiltrate multiple tissues and organs. It may affect visceral organs, mediastinum, soft tissues, and bones, making diagnosis and management challenging due to its rarity and overlapping clinical features with other conditions [2]. Imaging plays a crucial role in both evaluating and managing GLA. MR lymphangiography, an advanced imaging technique, is especially useful for visualizing abnormal lymphatic anatomy and assessing lymph flow dynamics. Particularly T2-weighted imaging is performed using intranodal, intrahepatic, or intramesenteric approaches. MR lymphangiography allows for noninvasive evaluation of lymphatic flow and valvular function in major lymphatic ducts, helping determine disease extent and guide treatment planning [3]. Currently the patient is in a better condition, and continues to be under the observation of the lymphatic clinic. He is experiencing shortness of breath and fatigue, but his condition is now stable.
In our case, effective treatment was not possible. Conservative treatment, which consisted of parenteral nutrition combined with pleural drainage, yielded persistent massive chyle evacuation (up to 1 l/day). When conservative methods do not succeed, suitability for surgical intervention should be reviewed. Therefore, VATS was performed, but no obvious cause of chylothorax was identified. Thus, thoracic duct ligations were performed. In cases of traumatic chylothorax, the success rate is very high (up to 85%) [4]. Regrettably, after the first surgery, drainage remained at a similar level. Possibly, the second MR lymphangiography with contrast solved the treatment problem since it revealed the etiology. A further challenge in this case was that the etiology of chylothorax could not be definitively established. Traumatic causes account for the majority of cases, with iatrogenic injury being the most frequent [5]. In this patient, traumatic etiology was not identified. The only previous surgical procedures were performed in the abdominal cavity. However, between procedures chylous ascites appeared. Further traumatic causes were considered unlikely: raised intra-abdominal pressure, vertebral fracture, central venous access. Malignancy (lymphoma, carcinoma), the most frequent non-traumatic cause, was excluded. Increased venous pressure due to heart failure, which may be another possible etiology of chylothorax, was also excluded [6].
Chylothorax occurs very seldom, but it must not be ignored due to its dangerous implications. Determining the etiology is crucial for proper treatment of this condition. A plausible cause of chylothorax was found during the first MR lymphangiography, which revealed thoracic duct injury in the right posterior mediastinum with leakage into the left pleural cavity. Only after further ligation surgery and MRI lymphangiography was the diagnosis of GLA established. The present case highlights the diagnostic and management challenges of chylothorax.