Currarino–Silverman syndrome is a rare congenital deformity of the anterior chest wall, with an estimated incidence ranging from 1 in 1,000 to 1 in 10,000 live births and a male-to-female ratio of approximately 4 : 1. The deformity results from premature fusion of the manubriosternal junction and sternal segments, leading to characteristic structural abnormalities such as a high carinate chest, a shortened Z-shaped sternum, anterior projection or absence of the xiphoid process, and deformation of the costal cartilages [1]. Therapeutic management depends on the patient’s age and the severity of the deformity. Treatment of advanced deformities typically requires surgical correction. One of the main operative techniques is the Ravitch procedure, which involves resection of the deformed costal cartilages, repositioning of the sternum, and stabilization. The Ravitch procedure is associated with significant postoperative pain, often necessitating the use of high doses of opioids and non-steroidal anti-inflammatory drugs (NSAIDs). Inadequate pain control can impair respiratory function, delay recovery, and prolong hospitalization, which typically lasts between 5 and 7 days. Therefore, the search for effective and safe analgesic methods that minimize opioid requirements and improve postoperative comfort remains an important aspect of perioperative care. One of these methods is intraoperative intercostal nerve cryoanalgesia [2], first described in 1961 by Cooper and Lee for the treatment of Parkinson’s disease and other neurological disorders [3]. The mechanism of action involves reversible injury to the sensory axons, resulting in temporary interruption of pain transmission without permanent structural nerve damage. The duration of the analgesic effect can be adjusted by modifying the cryoprobe’s parameters [2]. Currently, cryoanalgesia is used in various surgical specialties, including cardiac, thoracic, and orthopedic surgery, and its efficacy in reducing postoperative pain and opioid consumption has been confirmed in numerous studies [2, 4]. In pediatric and adolescent thoracic surgery – particularly in the Ravitch and Nuss procedures – intercostal nerve cryoanalgesia is increasingly used as part of a multimodal postoperative pain management strategy [2, 4, 5].
The aim of this study is to present a case of a patient with Currarino–Silverman chest wall deformity who underwent surgical correction using the Ravitch technique, with intraoperative intercostal nerve cryoanalgesia applied as a modern and effective method of reducing postoperative pain.
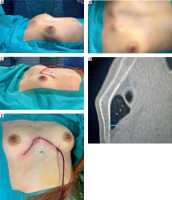
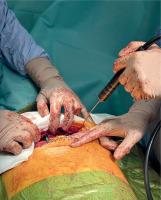
A 17-year-old female patient was admitted to the Department of Pediatric Surgery for operative correction of a congenital Currarino–Silverman chest wall deformity. The patient reported neither pain nor dyspnea, and the deformity was cosmetic. On physical examination, anterior protrusion of the sternum and the anterior parts of the ribs in the mid-chest region was observed, with no signs of mediastinal compression. The patient’s anthropometric parameters were as follows: body weight 44 kg, height 157 cm, and body mass index (BMI) 17.85 kg/m². Laboratory and imaging tests performed as part of the preoperative assessment revealed no abnormalities. On the second day of hospitalization, corrective surgery was performed using the Ravitch technique. After induction of general anesthesia, a transverse submammary incision was made, and the anterior chest wall was exposed. Deformed costal cartilages were resected, preserving perichondrial continuity. Wedge osteotomy of the sternum was performed, followed by stabilization with reconstruction plates (Figure 1). As part of intraoperative pain management, cryoanalgesia of intercostal nerves II, III, and IV was performed bilaterally (Figure 2). Cryoablation was carried out using a cryogenic probe cooled to approximately –70°C, with an application time of 2 minutes per nerve. The goal was to achieve temporary sensory blockade of the dermatomes corresponding to the surgical field. Postoperatively, the patient was monitored in the surgical ward. Multimodal analgesia included ketoprofen, metamizole, paracetamol, and gabapentin. No opioids were required during hospitalization. Pain intensity assessed using the Numerical Rating Scale (NRS) ranged from 0 to 2 points at rest and 2 to 3 points during coughing or movement. The postoperative course was uneventful. No neurological symptoms or local complications related to cryoanalgesia were observed. Surgical wounds healed properly, without sensory disturbances or signs of infection. On postoperative day 4, the patient was discharged in good general condition with recommendations for continued oral analgesic therapy at home and outpatient follow-up after 7 days. The postoperative analgesic required only NSAIDs. Follow-up evaluation revealed no early or late complications related to either the Ravitch procedure or cryoanalgesia. The patient reported no pain or sensory disturbances within the chest area.
Currarino–Silverman deformity represents a rare and distinct clinical entity among congenital deformities of the sternum and costal cartilages [1]. Its pathogenesis is related to premature fusion of the manubriosternal junction and adjacent sternal segments, resulting in the characteristic anterior protrusion of the chest wall. The deformity typically presents with a shortened, deformed sternum, accompanied by structural abnormalities of the costal cartilages. Most patients remain asymptomatic or report only minimal symptoms. However, in some cases, exertional dyspnea, chest tightness, reduced exercise tolerance, palpitations, or retrosternal pain may occur. The deformity may also coexist with congenital cardiac anomalies, including mitral or tricuspid regurgitation and ventricular septal defects [1]. An important clinical aspect is patients’ satisfaction with the cosmetic appearance of the chest, which is usually the primary motivation for surgical correction. Due to the rarity of this condition and the lack of large clinical trials, no standardized guidelines exist for determining the optimal treatment or indications for surgery. Surgical treatment, most commonly the Ravitch procedure, involving resection of deformed costal cartilages and wedge osteotomy of the sternum with stabilization using reconstruction plates, remains the most effective method of correction. Reported postoperative hospital stays vary from 2.9 to 6.5 days [5]. In the present case, the patient was discharged on the second postoperative day – shorter than typically reported in the literature for Ravitch repairs performed without cryoanalgesia. Although causality cannot be definitively established, intraoperative cryoanalgesia likely contributed to the shortened hospitalization. Post-thoracotomy pain remains a major clinical challenge, impacting not only patient comfort but also the risk of pulmonary complications and the overall duration of recovery. Effective pain control is crucial for maintaining adequate ventilation, promoting early mobilization, and reducing respiratory infection risk. Cryoanalgesia has gained increasing popularity in recent years as a safe and effective method of postoperative pain control in thoracic surgery, including the repair of chest wall deformities such as pectus excavatum by the Nuss technique. Studies have demonstrated that intraoperative cryoanalgesia significantly reduces postoperative opioid requirements and shortens hospital stay [6, 7]. The mechanism of cryoanalgesia involves localized application of extreme cold to induce temporary injury of sensory nerves. This results in reversible axonal degeneration (Wallerian degeneration), temporarily interrupting pain transmission without permanent neural damage. Regeneration of affected fibers typically occurs within several weeks, corresponding to gradual recovery of sensation in the treated dermatomes. Rettig et al. reported that cryoanalgesia in patients undergoing the Ravitch procedure reduced mean hospital stay from 6 to 2.3 days compared with epidural anesthesia, while also decreasing opioid use during hospitalization and follow-up. Notably, despite the slightly longer operative time, total hospital costs were lower in the cryoanalgesia group [5]. In the present case, cryoanalgesia provided sufficient pain relief to avoid opioids entirely. Multimodal analgesia with ketoprofen, metamizole, paracetamol, and preoperative gabapentin contributed to stable postoperative pain control. A recent study by Walendziak et al. explored the concept of performing cryoanalgesia 1 day prior to chest wall surgery, suggesting potential benefits; however, further research in larger cohorts is necessary to validate the efficacy and safety of this approach [4]. The principal limitation of our study is that it presents a single clinical case in which established techniques – modified Ravitch repair and intraoperative cryoanalgesia – were applied. Nevertheless, growing evidence supports the view that cryoanalgesia in thoracic surgery shortens hospital stay and reduces the need for postoperative analgesics. Future prospective studies on larger patient populations are warranted to determine whether intraoperative cryoanalgesia during Ravitch repair for Currarino–Silverman deformity significantly decreases hospitalization time, reduces or eliminates opioid requirements, lowers healthcare costs, and improves overall quality of life.
In conclusion, the Ravitch procedure is a safe and effective surgical method for the correction of Currarino–Silverman–type pectus carinatum. The use of intraoperative intercostal nerve cryoanalgesia during the Ravitch procedure may significantly reduce postoperative opioid requirements and shorten the duration of hospitalization.