A 57-year-old Japanese male visited our department with a 16-month history of chronic spontaneous urticaria (CSU) that had been turning for the worse in the last 6 weeks. He was taking oral epinastine, lafutidine, and montelukast. He had a history of renal cell carcinoma and diabetes mellitus. At presentation, urticaria control test (UCT) score was 7, and 7-day urticaria activity score (UAS7) was 28, indicating a severe condition. Serum IgE level was 246 IU/ml. Omalizumab (300 mg) therapy was initiated because his urticaria was intractable. However, he had a fever the day after the first omalizumab administration. Since the polymerase chain reaction (PCR) test was positive for severe acute respiratory syndrome coronavirus 2 (SARS-CoV-2), the patient was hospitalized. On admission, the laboratory test showed normal white blood cell count (5300/μl) and elevated C-reactive protein (2.07 mg/dl) and IgE (507 IU/ml). Treatment with favipiravir (3600 mg on the first day and 1600 mg/day for following 4 days) and dexamethasone (6 mg/day) was started on the second day (Day 2) of admission. As the fever persisted, wheals with strong itch began to appear throughout the body (Figures 1 A, B) even with continuous epinastine, lafutidine, and montelukast. Because of persistent fever, exertional dyspnoea, and interstitial pneumonia identified by computed tomography (Figure 2), nafamostat and antibiotics were also administered. The plasma D-dimer concentration was 7.6 μg/ml at this time. His fever subsided on Day 9, and urticarial symptoms disappeared simultaneously. The D-dimer level was below the detection limit when the patient was discharged on Day 16. His urticaria was well controlled thereafter with epinastine, lafutidine, and montelukast. One month after the discharge, UCT score was 15. Since urticarial symptoms recurred 2 months after recovery from coronavirus disease 2019 (COVID-19) with UCT score 4, omalizumab was resumed, which rapidly improved the UCT score to 13 one month later.
Figure 1
Clinical photographs on Day 7 (A) and Day 8 (B) of hospitalization. Wheals were distributed on the trunk
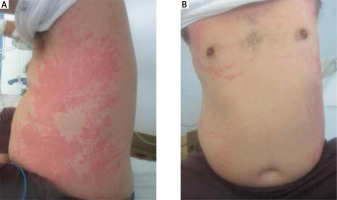
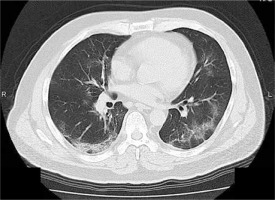
Figure 2
Imaging findings of the lungs. Bilateral areas of ground-glass opacities in a peripheral distribution on the image of computed tomography
In general, CSU can be exacerbated by viral infections. In addition, COVID-19 has been reported to complicate the symptoms of CSU [1]. Urticarial lesions accounted for 8.1–26.6% of cutaneous manifestation of COVID-19 [2]. In particular, it is reported that 10% of COVID-19-associated urticarial eruptions developed before the onset of its classical signs including fever and respiratory symptoms [3]. Furthermore, Kocatürk et al. published data of the patients affected by COVID-19 during the treatment of chronic urticaria, including irritation-induced urticaria lasting more than 6 weeks, at centres registered in UCARE (Urticaria Centers of Reference and Excellence) [4]. Data of 79 patients were collected from 33 of 110 centres worldwide. While 29 (36.7%) patients experienced exacerbation of urticaria in association with COVID-19, the majority (44 patients, 55.7%) was free from deterioration of urticarial symptoms. Worsening of urticaria was more frequently observed in patients hospitalized for COVID-19 than in those without hospitalization. Therefore, it is possible that patients with severe COVID-19 are more likely to show exacerbation of urticaria, which is consistent with the current case.
In our case, urticaria flared up despite the administration of omalizumab immediately before the onset of COVID-19. A possible explanation for this is that only single administration of omalizumab was not sufficient to control his urticaria immediately. Indeed, some of the patients are known to take time to show a substantial response, requiring multiple doses, after the initiation of omalizumab therapy [5, 6]. Another possibility is that the flare-up was provoked by IgE-independent pathogenic process. Urticaria due to viral infection is not necessarily dependent on IgE [7, 8]. Activation of the complement system is proposed to serve as one of the non-IgE triggers [8] because mast cells are activated by C3a and C5a [9]. Another important non-IgE factor should be an enhanced coagulation system. COVID-19 is known to cause microthrombosis through abnormal activation of coagulation pathways, which affects various organs including skin [2]. Since increased coagulation cascade is thought to be involved in the pathophysiology of urticaria [10], COVID-19 may cause or exacerbate urticaria through this mechanism. Indeed, plasma D-dimer was elevated during SARS-Cov-2 infection in our patient. On the other hand, there is a case report in which treatment with omalizumab was successful in COVID-19-associated urticaria [1]. Although the role of IgE in COVID-19-associated urticaria is to be elucidated, resolution of viral infection should be a key for amelioration of urticaria. Our patient had a substantial amount of serum IgE (246 IU/ml) before omalizumab therapy, and its level increased to 507 IU/ml after the first administration. Although such increase is usually linked to the good response to omalizumab [5], the opposite was true for our patient. On the other hand, when omalizumab therapy was re-initiated for the recurrence of CSU after recuperation from COVID-19, it clearly ameliorated his urticarial symptoms. This observation indicates that his recurrent urticaria after the recovery from COVID-19 was largely mediated by IgE.
In the era of COVID-19 pandemic, it should be noticed that acute exacerbation of urticaria may be associated with SARS-Cov-2 infection. Treatment of COVID-19 should be prioritized even in patients with urticaria. Standard basic treatments of urticaria should also be continued in such cases.
Conflict of interest
Hayama K has received a study grant or honoraria for being a speaker from Boehringer Ingelheim, Kyorin, Novartis, and Taiho. Fujita H has received a study grant or honoraria for being a speaker from Boehringer Ingelheim, Kyorin, Novartis, Taiho. Izaki S, Hayashi K, Kurosawa Y, Yamada S, Shimizu T and Gon Y declare no conflict of interest.









