Introduction
Fatty acid-binding protein (FABP) is a family of cytoplasmic proteins, which bind long-chain fatty acids and other hydrophobic ligands. Their basic role is an uptake of fatty acids, their transport and metabolism [1–3]. In addition, they act as signalling molecules, thereby regulating inflammatory pathways [1–3].
Since the discovery of FABP in 1972, nine members of this FABP family have been identified. They are highly expressed in various tissues: in a liver (L-FABP), intestines (I-FABP), heart (H-FABP), adipocytes (A-FABP), epidermis (E-FABP), ileum (IL-FABP) FABP), brain (B-FABP), myelin (M-FABP) and testes (T-FABP) [4, 5]. FABPs represent from 1% to 5% of all soluble cytosolic proteins, and their number may increase with higher supply of lipids in these cells [6].
Epidermal-fatty acid-binding proteins (E-FABPs), also known as FABP5, are expressed most abundantly in the granular layer of the epidermis, where lipid synthesis takes place to build the correct epidermal barrier [3]. They also occur in other tissues: tongue, adipose tissue (adipocytes and macrophages), dendritic cells, mammary gland, brain, kidneys, liver, lungs and testes [1, 2, 7].
E-FABPs are a marker of the so-called transiently amplifying cells (TACs) [8]. TACs are formed from stem cells in the epidermis, they undergo mitotic divisions many times and they become differentiated. According to the classic stem cell division theory, they are divided by asymmetric mitosis, yielding one daughter (stem) cell and one TAC. Psoriatic keratinocytes overexpress E-FABP compared to normal skin cells and they are associated with an increase in the amount of TAC, which leads to acanthosis [9]. Inhibition of E-FABP in psoriatic keratinocytes significantly reduces their differentiation, while increasing the number of psoriatic markers, such as survivin and cytokeratin K16. This confirms the important role of this molecule in the process of differentiation of epidermal cells [10]. In addition, the reduction of E-FABP expression reduces their sensitivity to “psoriatic trigger factors” [10].
Recently, studies which used various genetic models, have shown that FABP play a key role in the uptake and utilization of fatty acids in metabolic processes (in the muscles), and are involved in the regulation of gene expression (adipose tissue and macrophages), protecting cell membranes against toxicity of lipids and their derivatives [11].
The presence of E-FABP on adipocytes in adipose tissue and their overexpression in psoriasis may explain the association of this disease with disturbances in lipid metabolism. The ratio of A-FABP to E-FABP in adipocytes isolated from adipose tissue from mice is about 99 : 1, whereas on macrophages, about 1 : 1 in physiological conditions [1, 2, 7]. In turn, E-FABP expression is increased on adipocytes, but not on macrophages, in transgenic mice with a deficiency in A-FABP [1, 2, 7]. These mice fed a high-fat diet, in addition to the increased E-FABP expression in adipose tissue, show a decrease in insulin sensitivity. However, the lack of E-FABP in these mice leads to a small increase in insulin sensitivity [12].
Methotrexate (MTX) is a widely used drug in the treatment of psoriasis with anti-inflammatory, anti-proliferative and immunosuppressive effects. Currently, there is a lot of evidence for its anti-atherosclerotic role. MTX, both in people with psoriasis and other rheumatic diseases, reduces the risk of coronary heart disease, and also reduces the risk of mortality due to cardiovascular disease (CVD) by 70% compared with patients who have not been treated with this drug [13].
Low doses of MTX (15–20 mg/week) taken in the long term cause a reduction in cardiovascular risk in treated patients [14]. This is associated not only with the reduction in proinflammatory interleukin (IL)-6 and the production of C-reactive protein, but above all it is associated with the mechanism of regulation of reverse cholesterol transport [14]. It consists of increasing expression of cholesterol 27-hydroxylase and ATP transporter of membrane complex A1–ABCA1 (ATP-binding cassette transporter-A1), releasing adenosine and stimulating its A2 receptor, a natural COX-2 inhibitor [15, 16]. A2A stimulation suppresses inflammation directly and reduces the expression of adhesion molecules, such as intercellular adhesion molecule 1 (ICAM-1) and vascular cell adhesion molecule (VCAM), associated with atherosclerosis progression [17].
Material and methods
The study group consisted of men, aged between 18 and 60 years with a severe course of plaque psoriasis (PASI > 10) without comorbid psoriatic arthritis (n = 11), treated at the Outpatient Clinic and at the Department of Dermatology, Sexually Transmitted Diseases and Clinical Immunology in Olsztyn. Patients with chronic and acute inflammatory diseases other than psoriasis, neoplastic diseases, previous cardiovascular complications, heart, kidney and liver failure were excluded. Patients had not been treated for psoriasis for at least 4 weeks and topically for 1 week before the enrolment.
The control group (n = 5) comprised men, healthy volunteers, with no personal or family history of psoriasis, concomitant autoimmune and inflammatory diseases. Skin samples of the healthy abdominal skin of volunteers were obtained from surgical wastes obtained after removal of pigmentary lesions.
Patients with psoriasis were treated with MTX at a dose of 15 mg/wk for 12 weeks in the form of subcutaneous injection and received 5 mg folic acid on the second day after taking MTX.
We have determined the main research goals:
Evaluation of E-FABP expression in biopsy speciments from the lesion and perilesional skin in patients with psoriasis before and after 12 weeks of treatment with MTX compared to the healthy skin of volunteers.
Evaluation of the expression of E-FABP and apolipoprotein A1 and B levels in serum of psoriatic patients before and after 12 weeks of MTX treatment compared to healthy ones.
Clinical samples
E-FABP expression and apolipoprotein A1 and B levels in blood serum were assessed by ELISA in psoriasis patients before and after treatment with MTX and they were evaluated in comparison to healthy subjects.
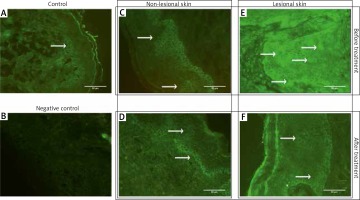
Assessment of E-FABP expression in biopsy speciments was performed by immunofluorescence method. We obtained two 3-mm punch biopsies per patient: one from the centre of the psoriatic plaque (abdominal region), one from non-lesional skin (at least 2 cm from the target lesion), and one from healthy volunteers (abdominal region), using local anaesthesia (2% lignocaine). Biopsy speciments were taken before and after 12 weeks of treatment from psoriatic patients. Frozen skin sections were sliced (Leica 3050, Germany, FSE Cryotome Thermo Scientific, USA) into 4–6 μm slices. Immunodetection was performed with anti-E-FABP antibodies staining using fluorescein-labelled goat antibodies. The labelled tissues were photographed using a C-5060 Camera (Olympus, Japan) mounted on a light microscope (CH30/CH40, Olympus, Japan). The images were subjected to semiquantitative analysis. The level of immunoreactivity was measured with ImageJ software (image processing and analysing in Java, USA). Quantitative analysis was performed using the automatic threshold.
The permission of the Bioethical Committee of the Warmia and Mazury University was obtained (26/2016).
Results
The median PASI prior to treatment was 15.39 ±6.55, while the post-treatment value was 6.0 ±4.43. As a result of treatment, PASI was reduced by 38.98% (p < 0.05).
Evaluation of E-FABP expression in skin sections
E-FABP expression was recorded in both the control group (healthy skin) and in psoriatic patients biopsy speciments from the lesions and perilesional skin).
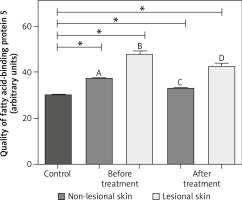
The expression of E-FABP differs in individual experimental groups (p < 0.01):
it was lower in the control group in comparison with the expression in lesional, psoriatic and perilesional skin, both before and after treatment,
it was lower in the perilesional skin than in healthy skin from volunteers,
after treatment, the expression decreased in both psoriatic and perilesional skin (Figures 1, 2).
Evaluation of E-FABP expression in blood serum
E-FABPs were detected in the serum of healthy subjects and patients with psoriasis. Their level was higher in healthy patients (482.855 ±240.550 pg/ml) compared to the patients, but not statistically significantly. However, after treatment, a statistically significant reduction was observed (427.916 ±93.26 pg/ml vs. 240.1277 ± 77.25 pg/ml, p < 0.01) in relation to the group of patients before and after treatment.
Evaluation of apolipoprotein A1 and B in blood serum
Apolipoprotein A1 (Apo A1) levels did not differ in the control group (7.965 ±0.936 ng/ml) and the group of patients, both before and after treatment (7.31 ±0.79 ng/ml vs. 8.00 ±1.08 ng/ml), the levels were at the limit of the test sensitivity. In contrast, apolipoprotein B (Apo B) levels did not differ statistically between the healthy group (1447.126 ±311.11 ng/ml) and patients before treatment, while they were the lowest after treatment (1081.67 ±117.83 ng/ml vs. 808.306 ±103.72 ng/ml; p < 0.01) (Figure 3, Table 1).
Table 1
Evaluation of parameters before and after 12 weeks of MTX therapy in comparison to healthy people
| Parameter | Control | Psoriatic patients before MTX | Psoriatic patients after MTX | Effect of MTX |
|---|---|---|---|---|
| PASI | 0 | 15.39 | 6.0 ±4.43 | 38.98% ↓* |
| E-FABP in sera | 482.855 ±240.550 | 427.916 ±93.26 | 240.127 ±77.25 | ↓* |
| ApoA1 in sera | 7.965 ±0.936 | 7.31 ±0.79 | 8.00 ±1.08 | – |
| ApoB in sera | 1447.126 ±311.114 | 1081.67 ±117.83 | 808.306 ±103.72 | ↓* |
Discussion
Methotrexate has been used for many years in psoriasis treatment. However, the exact mechanism of MTX in psoriasis condition is still poorly understood. Our research showed that it has an effect on decreasing the E-FABP expression, which is probably due to its antiproliferative activity, thus reducing the amount of TAC cells marked by FABP. The effect of MTX on hyperproliferation in psoriasis is due to the activation of intrinsic apoptotic pathway of psoriatic keratinocytes [18–20]. E-FABPs are involved in the process of keratinocyte differentiation, but the mechanism is not completely clear [21]. In addition, expression of CD4+ T cells revealed on E-FABP promotes maturation of the Th17 line and inhibits Treg. This results in the increased production of IL-17, which directly stimulates hyperproliferation of keratinocytes [22].
It is very difficult to discuss obtained results, because so far no similar reports on the effect of MTX on the expression of E-FABP (PA-FABP) have been published. Several papers showed only the importance of FABP5 in the process of keratinocyte differentiation in psoriatic patients [10, 23]. However, there are only individual reports assessing the expression of this molecule after treatment in psoriasis.
Kuijpers et al. [24] evaluated E-FABP expression using immunohistochemistry and Northern blot analysis. The expression of E-FABP mRNA in lesions was strong, while in healthy skin it was absent. After 4 weeks of topical treatment with hydrocortisone 17-butyrate 0.1% twice daily for 4 weeks, a significant clinical improvement accompanied by a marked decrease in E-FABP mRNA was achieved, while the staining pattern for E-FABP at the protein level was not changed. The change in E-FABP expression is slower than clinical improvement. The authors speculated that it results from the necessity to rebuild the lipid barrier after the lesions and the role of these receptors in the transport of extracellular fatty acids [24].
In Miyake et al. [25] study, E-FABP expression in skin-stripping was significantly higher in lesions than in uninvolved skin and the uninvolved skin of patients had higher levels than the skin of healthy individuals. E-FABP levels were similar in different areas of the body except the face, where the expression was significantly higher, probably because of the higher expression in the sebaceous glands. E-FABP expression decreased after treatment with TNF-α inhibitors (adalimumab and infliximab) or narrow-band ultraviolet B irradiation in patients with improvement in PASI [25, 26]. Interestingly, no significant correlation was detected between PASI and skin-stripping E-FABP levels [25].
The relationship between E-FABP expression and lipid metabolism is interesting, but still not explored. Zhang et al. [27] demonstrated the relationship of E-FABP expression in skin lesions in obese mice induced by a high-fat diet. This diet led to accumulation of a particular type of CD11c macrophages, stimulated by IL-1β and IL-18 production, resulting in metainflammation and insulin resistance. Furthermore, E-FABP-deficient mice were completely resistant to diet-induced skin lesions [27].
E-FABP expression increases in response to increased lipid transport, which may be associated with abnormal proliferation and differentiation of psoriatic keratinocytes. E-FABPs induce keratinocyte differentiation by enhancing the transcriptional activity of peroxisome proliferator-activated receptors (PPAR) by transporting fatty acids directly to PPARs [28, 29].
Currently, the beneficial effect of MTX treatment on the metabolic indicators improvement is emphasized. In a study by Toms et al. [30], 400 patients improved lipid parameters and fasting glucose levels without improving insulin sensitivity after treatment. Other authors have not observed a beneficial effect on the metabolic parameters e.g. LDL and HDL in RA [31, 32]. In contrast, Navarro-Millán et al. [33] observed an increase in total cholesterol, LDL and HDL cholesterol in the 24th week of MTX treatment, and Georgiadis et al. [34] revealed a significant increase in these parameters after a year of constant MTX doses in rheumatoid patients. Our studies to evaluate lipid parameters in 24 psoriatic patients with PASI > 10, treated with 12-week MTX 15 mg subcutaneously, showed increased triglycerides by almost 20% (p < 0.0465) with a small decrease in HDL by 0.72% in treated patients [20]. The results of these studies are surprising and difficult to analyse, especially since the association of MTX with the mechanism of regulation of reverse cholesterol transport has been proven. Some researchers suggest that lipid elevation is offset by a decrease in the amount of Apo B and an increase in Apo A1, as in the case of treatment with anti-TNF-a in patients with rheumatoid arthritis [34, 35]. Apo B have been proposed as markers to evaluate the atherogenic damage [36]. In our study we obtained a favourable result of the decrease in Apo B level. Based on the available evidence, the European Association for Cardiovascular Prevention & Rehabilitation emphasises that Apo B is a similar marker of the cardiovascular risk as LDL-C, with lower laboratory mistakes, particularly in patients with hypertriglyceridemia [37]. In addition, the cardiovascular risk associated with Apo B is higher in younger people compared to older people [36]. It has a great importance in reducing the cardiovascular risk in young patients with psoriasis, especially those with a severe course.
Our study is the first to evaluate the effect of MTX on serum apolipoproteins in psoriatic patients, and the lack of other reports makes it difficult for us to compare results.
Perhaps E-FABPs will be a therapeutic target for psoriasis with accompanying metabolic disorders such as obesity, diabetes, and atherosclerosis. It can also be a useful marker used to monitor psoriasis activity and treatment outcomes [25].