Atopic dermatitis (AD, eczema), is a chronic skin disease caused by incorrect reactions of the immune system. Common symptoms are defined using Hanifin and Rajka diagnostic standards. In AD the skin barrier is defective, pruritus threshold is lowered and there is higher sensitivity to various stimuli. For these reasons there are lots of factors such as environmental allergens, psychological stress, perspiration, chemical irritants, temperature fluctuations, exposure to wool and lanolin, which can exacerbate atopic dermatitis [1]. Moreover, there is a connection between viral infections and aggravation of AD which probably occurred in the presented case [2, 3].
Coronavirus disease caused by SARS-CoV-2 is still undergoing extensive research regarding the clinical presentation in various patients. This virus is constantly evolving, there are new mutations and because of that, complete clinical manifestation has not been fully discovered yet. The main symptoms resemble influenza with headache, dry cough, loss of smell, low fever, sore throat, nasal congestion, fatigue, myalgia, arthralgia, nausea and diarrhoea. Most patients are asymptomatic or oligosymptomatic. There is still little known about the skin manifestation connected with SARS-CoV-2 [3].
A 23-year-old woman has been suffering from atopic dermatitis since infancy. This condition was diagnosed using Hanifin and Rajka diagnostic criteria at the age of 10. She fulfils four out of four major criteria. There is a positive family history (her father has allergic rhinoconjunctivitis), pruritus, typical localization and chronic character. The patient has been using an emollient preparation, topical glucocorticosteroids and calcineurin inhibitors so far with a moderate effect. The patient does not suffer from either atopic or chronic disease.
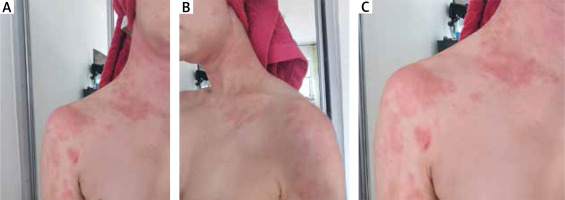
Control of the disease had been satisfying for approximately 5 years without need for hospitalization. In February 2021, a strong exacerbation occurred. Five days earlier, the patient had contact with a person infected with coronavirus who was presenting with symptoms of infection and later confirmed the presence of antibodies. Unusual was the fact that skin lesions included places where they usually had not appeared before. They were located over a large area and were significantly more severe – skin was reddened all over the neck, décolleté, nape, dorsal parts of the hands, wrists and in the knee fossa (Figures 1 A–C).
Later there was lichenification and cracking of changes. The pruritus was described by the patient as significant, but it did not cause sleep disturbances. The day after lesions had arisen, the patient lost sense of smell and the day after that, loss of taste occurred. Other symptoms included weakness, muscle and joint pain, low-grade fever (38°C) that lasted for about 3 days. After a period of self-isolation and waiting for the spontaneous resolution of the lesions, the woman reported to a dermatologist. It took place 4 weeks after the changes occurred. The doctor recommended hospitalization that took place in the 5th week after the appearance of the changes. The patient was admitted to the Department of Dermatology, Venerology and Allergology, Wroclaw Medical University.
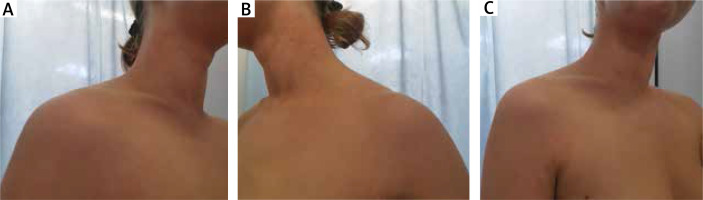
In laboratory analyses insignificant neutrophilia, slightly raised erythrocyte sedimentation rate, ketonuria and a raised rate of total IgE antibodies was detected. Treatment in hospital included: hydrocortisone injections, topical prednisone in ointment twice a day, emollients twice a day, clemastine per os twice a day and UVB 311 nm phototherapy. During the hospitalization 4 sessions of irradiations were carried out. After 4–5 days of treatment the lesions resolved, but after stopping the injections the lesions began to return. Changes were present at discharge. After hospitalization, the prednisone ointment was prescribed. The patient was still undergoing UVB treatment. 18 irradiations have been carried out, and ultimately there will be 23 of them in total. Daily care is provided on an ad hoc basis using emollient products (Figures 2 A–C).
The pathophysiology of AD is complex and multifactorial – the development and symptoms are related to environmental, immunological, non-immunological and genetic mechanisms [4]. There is a predisposition to overproduction of immunoglobulin E, increased type I immune response to many allergens and increased Th2-type cytokine production such as IL-4, IL-5 and IL-6. As a result of predominance of Th2-type lymphocytes, the activity of Th1-type lymphocytes (mainly responsible for producing interferon γ and protecting against infection) is reduced. Based on that, patients with atopic dermatitis may have a higher risk of upper respiratory tract infections [5].
Coronavirus SARS-CoV-2 infection also can provoke immunological overreactivity. Several studies claim that a “cytokine storm” occurs then. This phenomenon is understood as overproduction of various inflammatory mediators especially IL-1, IL-8, TNF-α and as in AD – IL-6 [6]. Very few patients develop skin conditions during the infection. They are 72% chilblain-like and 28% erythema multiforme-like. In most cases skin lesions appear a few days after the respiratory symptoms and are located on distal parts of digits [7].
It is worth underlining that there was no case like this before. The patient has atopic dermatitis in a state of remission and possibly the COVID-19 disease has affected the immunology system in a way that exacerbation of underlying pathology was stronger than ever before. Possibly it is connected with the fact that in both conditions there is incorrect, higher production of cytokines and that leads to similar immune effects. The release of COVID-19-induced cytokines may have been perceived by the organism as another AD exacerbation. In this case unusually the skin manifestations preceded the respiratory symptoms, were located differently and had different appearance, which may suggest that these skin lesions were an exacerbation of atopic dermatitis and not a cutaneous manifestation of COVID-19. The usually applied treatment plan for AD proved to be successful although that may not be the case in other patients.
There is still a lot to uncover about COVID-19, its influence on other diseases, especially the autoimmune ones and possible consequences for the patient in the long run. Medicine does not know a lot about factors surrounding SARS-CoV-2 infection which are crucial to fully understand the way it affects human organisms and the skin as well.