Introduction
The health effects of air pollution are increasingly recognized as a major public health concern. Previous studies that were carried out in major world cities proved the harmful effects of air pollutants on the course and prognosis of acute and chronic diseases among adults and children [1–3]. Estimates of the health impacts attributable to exposure to particulate matter (PM) with an aerodynamic diameter of 2.5 µm or less (PM2.5), ozone (O3), and nitrogen dioxide (NO2) concentrations in 2015, were responsible for about 518700 premature deaths originating from long-term exposure in 41 European countries [4]. The epidemiological evidence relating short-term exposure with particulate matter with an aerodynamic diameter of 10 µm or less (PM10), and related metrics: black smoke (BS), black carbon (BC) and total suspended particles, with health effects is substantial [5]. Recently published systematic review and meta-analysis of 110 time series studies have found evidence for adverse health effects of short-term exposure to PM2.5 across a range of important health outcomes and diseases with a considerable variation between different regions of the world [6].
Special attention is focused on the respiratory system, which is the first point of contact with air pollutants. The impact of air pollution on chronic respiratory diseases, such as chronic obstructive pulmonary disease and asthma is well documented [7–9]. The harmful effects of principle air pollutants (PM, O3, CO and NO2) on the exacerbation of asthma, as well as respiratory morbidity and mortality in asthma patients are confirmed by epidemiological studies [10–12].
The global increase in the prevalence of allergic diseases is of great concern, especially in developing countries [13] and strong epidemiological evidence supports a relationship between air pollution and exacerbation of asthma and other allergic diseases [14].
Although the global problem of air pollution is recognized worldwide, there are only a few published studies on the effects of air pollution on human health in Serbia [15, 16].
Aim
The aim of this study was to assess the short-term effect of air pollutants (NO2, SO2, PM2.5, PM10, and BC) concentrations on the exacerbation of the allergic bronchial asthma alone or asthma with coexisting allergic rhinitis (AR) in the Užice region, Serbia.
Material and methods
Study area
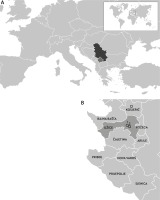
The study was carried out over a 2-year period, from 1st July 2012 to 30th June 2014 in the Zlatibor District, Serbia (Figure 1 A). The main city of the region is Užice with 78040 inhabitants [17], located in the latitude of 43°51˘ N and the longitude of 19°50˘ E. It is situated on both sides of the river Đetinja, with average elevation of 411 m above the sea level, surrounded by the Dinaric mountains Zlatibor, Tara and Zlatar. Besides the city of Užice (including Sevojno), two other surrounding municipalities, Čajetina with 14745 inhabitants, and Kosjerić with 12090 inhabitants [17] were included in this study. It is worth noting that there are three different climates in this region, from moderate-continental to mountain and high-mountain (sub-alpine and alpine) climate. While Užice and Sevojno are centres of heavy industry, the mountain Zlatibor, thanks to the specific continental and Mediterranean air currents, a so-called wind rose, is considered an air spa suitable for the treatment and recovery from many diseases, including asthma. Considering the above, the chosen geographical area is extremely interesting for the assessment of the relationship between air pollution and health.
Figure 1
Location of Serbia in Europe (A) and the Zlatibor District with the location of air quality and meteorological monitoring stations (B)
The study was approved by the Užice Hospital Ethics Committee.
Study population
We obtained routinely collected data of emergency department (ED) visits for allergic asthma from the Užice Health Centre, either from the EDs (ambulances or home care) in Užice, Sevojno, and Kosjerić or from a general hospital in Užice. A medical doctor reviewed the ED records. The admission date, age, gender, place of residence, and ED diagnosis were considered for each patient. The inclusion criteria were: adults aged 18 years and older with the diagnosis of allergic asthma (International Classification of Diseases, 10th revision, code J.45.0) or asthma with coexisting allergic rhinitis (AR). Patients who experienced worsening due to respiratory infections or asthma types other than allergic asthma were excluded from the study.
Air pollution, pollen and weather data
The daily average concentrations of air pollutants (SO2, NO2, PM2.5, PM10 and BC) in micrograms per cubic meter (µg/m3) were measured by three automatic ambient air quality monitoring stations located in Užice, Sevojno, and Kosjerić (Figure 1 B). The concentrations were measured on the event day (0), on the previous day (–1), 2 days before (–2) and 3 days before (–3). Registered daily values of each air pollutant were average levels from all the stations, in order to assess the global environmental situation of the city and its surrounding.
The SO2 concentration was determined by the spectrophotometric method, while the concentration of NO2 was obtained by chemiluminescence detection. The PM monitor based on beta-ray attenuation was used to measure the concentrations of both PM2.5 and PM10. The BCP (black carbon particles) concentration was measured with reflectometers.
The daily meteorological dataset (temperature, relative humidity, and surface air pressure), as well as air allergen data (daily tree, grass, and weed pollen concentrations) were obtained from the automatic meteorological station located at Zlatibor [18]. The following pollens were detected: Pinaceae, Betulaceae, Poaceae, Plantago spp., Urticaceae and Asteraceae.
Statistical analysis
A time-stratified case-crossover design was used to assess the risk of ED admissions for asthma alone and asthma with coexisting AR based on exposure to various air pollutants.
The degree of association between different environmental variables (air pollutants, pollens, temperature, humidity and air pressure) was tested by non-parametric Spearman’s rank correlation.
The multivariable conditional logistic regression models were applied as suitable for the explained design, aim and the type of data. Every seventh day before and after the event day was considered a control. Lagged values were created for all models to assess an early effect: immediate (the event day, lag 0), and delayed (previous 3 days of exposure, lag 1, 2, and 3, respectively). The models were defined for each of the pollutants (NO2, SO2, PM2.5, PM10, BC) for lags 0, 1, 2, and 3, for patients with asthma alone and asthma with coexisting AR. To control potential confounding factors all models included daily weather variables (temperature, humidity and air pressure on lag 0). The results of the analyses were expressed as odds ratios (ORs) with their accompanying 95% confidence intervals (CIs). The ORs were calculated in relation to air pollution concentration based on the daily mean level of each air pollutant presented by the third quintile in the way when the first or fifth quintile was the referent category.
A value of p < 0.05 was considered statistically significant. Statistical analysis was performed using SPSS statistical software (SPSS for Windows, release 21.0, SPSS, Chicago, IL).
Results
A total of 424 ED asthma visits (179 asthma alone and 245 asthma with AR) occurred during the study period (Table 1). Most of these visits (28.1%) concerned young adults aged 18–34 years. There were more visits among females (67.2%) and during the heating season (77.8%), while no statistically significant difference was seen between spring/summer and autumn/winter seasons.
Table 1
Number (%) of emergency department visits for asthma by age groups, sex and season in the Užice region, Serbia (2012–2014)
| Characteristic | Asthma alone | Asthma with AR | Total |
|---|---|---|---|
| Total visits | 179 (100) | 245 (100) | 424 (100) |
| Age group: | |||
| 18–34 | 44 (24.6) | 75 (30.6) | 119 (28.1) |
| 35–44 | 26 (14.5) | 52 (21.2) | 78 (18.4) |
| 45–54 | 32 (17.9) | 47 (19.2) | 79 (18.6) |
| 55–64 | 36 (20.1) | 42 (17.1) | 78 (18.4) |
| ≥ 65 | 41 (22.9) | 29 (11.8) | 70 (16.5) |
| Gender: | |||
| Males | 52 (29.1) | 87 (35.5) | 139 (32.8) |
| Females | 127 (70.9) | 158 (64.5) | 285 (67.2) |
| Season: | |||
| Spring/summer | 90 (50.3) | 116 (47.3) | 206 (48.6) |
| Autumn/winter | 89 (49.7) | 129 (52.7) | 218 (51.4) |
| Heating season*: | |||
| Yes | 36 (20.1) | 58 (23.7) | 94 (22.2) |
| No | 143 (79.9) | 187 (76.3) | 330 (77.8) |
Table 2 provides summary statistics for air pollutants, pollens and weather variables. During the study period, concentrations of NO2 and SO2 remained below the permitted daily limit values (85 µg/m3 for NO2 and 125 µg/m3 for SO2), whilst daily concentrations of PM10 and BC exceeded permitted limit values (50 µg/m3 for PM10 and 50 µg/m3 for BC) proposed by the national Regulation on monitoring conditions and air quality requirements.
Table 2
Daily concentrations of air pollutants, pollen levels and weather variables in the Užice region, Serbia (2012–2014)
Correlations between air pollutants, pollens and weather conditions are shown in Table 3.
Table 3
Matrix of correlation coefficients* between air pollutants, pollen levels and weather variables in the Užice region, Serbia (2012–2014)
Air pollutants were all positively correlated with each other (r = 0.24–0.83). The highest correlation was seen between PM2.5 and PM10 (r = 0.83), and between PM10 and BC (r = 0.75). NO2 was moderately correlated with particulates (r = 0.37–0.46). There was a weak correlation between SO2 and the other air pollutants (r = 0.24–0.33). All pollens were weak-moderately and positively correlated between each other (r = 0.15–0.62), and were negatively correlated with air pollutants (r ranged from –0.17 to –0.52).
Estimated adjusted odds ratios with 95% CI for ED visits for asthma alone and asthma with allergic rhinitis based on 1–3-day lagged exposure to air pollution are displayed in Table 4.
Table 4
Adjusted odds ratios with 95% confidence intervals for the relationship between exposure to outdoor air pollution and emergency department visits for asthma in the Užice region, Serbia (2012−2014)
[i] NO2 – nitrogen dioxide, SO2 – sulphur dioxide, PM2.5 – particulate matter with an aerodynamic diameter of 2.5 µm or less, PM10 – particulate matter with an aerodynamic diameter of 10 µm or less, BC – black carbon, AR – allergic rhinitis. Odds ratios were calculated for the third quintile of selected air pollutants and were adjusted for temperature, humidity and air pressure on the same day. Referent value for PM2.5 and BC was first quintile, while referent value for NO2, SO2 and PM10 was fifth quintile. All significant values are in bold.
Statistically significant associations were observed between ED visits for asthma and 3-day lagged exposure to BC (OR= 3.23; 95% CI: 1.05–9.95), and between ED visits for asthma with coexisting AR and 0-day lag exposure to NO2 (OR = 1.57; 95% CI: 0.94–2.65), 2-day lag exposure to SO2 (OR = 1.97; 95% CI: 1.02–3.80) and 3-day lag exposure to PM10 (OR = 2.38; 95% CI: 1.17–4.84).
Discussion
The present study analysed the impact of air pollution on ED visits for allergic asthma in the adult population of the Užice region. The results suggest a positive association between ambient exposure to PM10, BC, SO2 and NO2 pollutants and ED visits for asthma. The highest association was with BC and PM10. The most immediate effects were seen for NO2, associated with the reporting-day pollutant level.
PM, a complex, heterogeneous mixture whose composition changes in time and space, and depends on emissions from various sources, atmospheric chemistry and weather conditions, includes “fine particles” which are 2.5 mm in diameter or less (PM2.5) and “coarse particles” which have diameters between 2.5 and 10 mm (PM10) [19]. Many epidemiological studies have shown short-term harmful health effects of PM [5]. However, it is likely that not every PM component is equally important in causing health effects [20]. Combustion-related particles, known as black carbon (BC) particles, are thought to be more harmful to health than PM that is not generated by combustion [20]. Historical studies are based on BS, but more recent studies use absorbance (Abs), BC or elemental carbon (EC) as exposure indicators [21]. The highest association in the current study occurred with BC. We found that concentration of BC in the third quintile increased the risk for asthma exacerbation on lag-3, for more than three times (OR= 3.23; 95% CI: 1.05–9.95). The large concentration of BC that exceeds permitted daily limit values, in the Užice region, is a result of household heating during the cold season because most of the heating houses use coal or oil. Previous studies have reported positive associations between BC and ED visits and hospital admissions for asthma [22–24].
PM10 is one of the top air pollutants in Serbia, with all air quality monitoring stations in the country registering exceedances of the permitted daily limit value of 50 mg per cubic meter (µg/m3) [25]. We observed a significant association between 3-day lag exposure to PM10 and ED visits for asthma with coexisting AR (OR = 2.38; 95% CI: 1.17–4.84), which is in accordance with most previous studies of short-term health effects [26–31]. In contrast, several other studies have failed to observe a statistically significant association [24, 32, 33].
According to a large systematic review and meta-analysis of 110 peer-reviewed time series studies, Atkinson et al. [6] pointed to adverse associations between short-term exposure to daily concentrations of PM2.5 and daily mortality and hospital admissions for cardiovascular and respiratory diseases. Zheng et al. [30] and Orellano et al. [34] in their systematic reviews and meta-analyses of 87 and 22 studies respectively, found a significant association between exposure to PM2.5 and asthma exacerbations. However we failed to find any statistically significant association between PM2.5 and asthma ED visits, which is in accordance with a Canadian study conducted by Lavigne et al. [35].
In this study we found a positive association between exposure to NO2, one of the main air pollutants which is typically associated with vehicle emissions, and ED visits for asthma with coexisting AR (OR = 1.57; 95% CI: 0.94–2.65). The harmful effects of NO2 exposure on asthma exacerbation were reported by several studies [12, 22, 24, 28, 33, 34, 36]. Modig et al. [37] found a positive association between asthma onset (OR per 10 mg/m3 1.46, 95% CI: 1.07–1.99) and incident asthma in adults (OR per 10 mg/m3 1.54, 95% CI: 1.00–2.36) and the levels of NO2, which remained statistically significant after adjusting for potential confounders. Several authors [22, 31] found a strong correlation between emergency admissions for asthma and NO2 level only during cold seasons. Zheng et al. [30] in the meta-analysis of 87 time-series studies (including case-crossover studies) of short-term exposure to air pollutants, found that NO2 was associated with significantly increased risks of asthma emergency room visits and hospitalizations (RR = 1.02; 95% CI: 1.01–1.02). Based on results from 26 studies, Zhang et al. [38] found a statistically significant association between NO2 and asthma emergency hospital admissions only in children but not in people aged 15–64.
According to our results, a 2-day lag exposure to SO2 was associated with asthma exacerbation (OR = 1.97; 95% CI: 1.02–3.80), which is in accordance with previous studies on adults and children [24, 27, 30, 31, 39], while other authors have failed to observe such associations [25, 33]. Gharehchahi et al. [40] found a positive relationship between concentration of SO2 and hospital admissions due to respiratory diseases in the elderly, while Galán et al. [29] did not find any relationship between SO2 and asthma emergency room admissions.
There are several strengths of the present study. This manuscript is unique in that it is a novel population studied. Further, the time-stratified case-crossover design in which cases serve as their own control, used in the present study, has been demonstrated as a suitable method for assessing the relationship between air pollution and asthma exacerbation. Also, the reported odds ratios have been adjusted for the possible confounding influence of weather variables. However, there are several methodological limitations. The first one is that the study lacks statistical power to properly evaluate potential sex and age differences and some of non-statistically-significant associations reported (e.g. for PM2.5). The second one is due to the fact that the regional measures of air pollution from fixed-site monitoring stations were taken as the measure of exposure to air pollutants for each individual in this study. The third one is that we did not adjust for the confounding influence of levels of aeroallergens, which could lead to a change in risk.
Conclusions
Taking into consideration all limitations, our study confirms the association between exposure to PM10, BC, NO2, and SO2 pollutants and ED visits for allergic asthma in the Užice region, Serbia. Considering the importance of the geographical location of the study area as a combination of an industrial region and climatic health resort suitable for the treatment of respiratory diseases, the analysis of the short-term effect of outdoor air pollutants to allergic asthma in the Užice region is of great public health importance in establishing relevant public policy in western Serbia. Since most inhabitants in Užice, Kosjerić, and Sevojno use coal for heating, the introduction of a gas pipeline would reduce the concentration of combustion pollutants such as BC and SO2, which could decrease the number of asthma exacerbations. According to WHO recommendations [5], particulate air pollution can be reduced using stricter air quality standards and limits for emissions from various sources, reducing energy consumption, especially that based on combustion sources, changing modes of transport, land use planning, as well as individual behavioural changes (e.g. using cleaner modes of transport and household energy sources). Reasonable efforts to reduce ambient pollution levels and aeroallergen exposures offer the expectation to reduce asthma morbidity and asthma exacerbation in the Užice region.









