We report a 36-year-old man with a history of hypertension who presented with angina and dyspnea on exertion. Previously performed cardiac magnetic resonance imaging (MRI) demonstrated a delayed enhancement image localized subendocardially in the area of left coronary artery (LCA) distribution. Myocardial perfusion imaging with single-photon emission computed tomography performed before the hospitalization showed perfusion defects, both on stress images and rest images, correlated with abnormal wall motion (Figures 1 A, B). At admission, physical examination revealed a heart rate of 60 beats/min and blood pressure of 130/90 mm Hg. No pathological cardiac murmurs were detected. Echocardiography showed the left ventricular ejection fraction of 52%, hypokinesis of the apex and the anterior wall, and mild mitral regurgitation. Therefore, coronary angiography was performed, and it revealed a tortuous and dilated right coronary artery (RCA) with extensive collateralization to the LCA, as well as a tortuous and dilated LCA (Figure 1 C). Selective visualization of the LCA from the aorta was impossible to obtain. The clinical image indicated anomalous origin of the left coronary artery from the pulmonary artery (ALCAPA), also known as Bland-White-Garland syndrome. ALCAPA is a rare congenital coronary abnormality associated with sudden death, which in symptomatic patients obligatorily requires surgical intervention [1, 2].
Figure 1
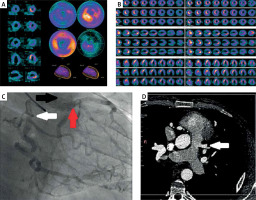
A, B – SPECT/CT scan was obtained using Technetium 99m (99mTc) sestamibi in a 2-day examination schedule. The patient underwent the standardized Bruce protocol for stress induction. The exercise test was terminated early, because the patient achieved 83% of maximum, age-adjusted, predicted heart rate. In both stress and rest images uptake of 99mTc sestamibi was similar, indicating irreversible perfusion. SPECT/CT scan showed extensive areas of severe perfusion defect in anterior, inferior, apical wall and moderately decreased radiotracer activity in lateral area. Hypokinesis of the left ventricle (rest 39%; stress 30%). Generalized dyskinesia except for the mid inferoseptal and basal inferoseptal areas. Single area of increased radiotracer uptake in the apical inferior and apical septal region. C – Coronary angiogram obtained with injection of dye into RCA reveals dilated and tortuous RCA (white arrow) with plenty of collateral arteries, through which the blood flows into the dilated LCA (red arrow); also the LCA opacifies the main pulmonary artery (black arrow). D – CT angiogram shows the origin of the dilated LCA from the main pulmonary artery (white arrow)
The coronary computed tomography angiography confirmed the ALCAPA. There was no visible connection between the LCA and the aorta. The LCA was directly visualized arising from the main pulmonary artery (Figure 1 D). Due to the rapid shunt of the blood from the RCA and the LCA, both of the vessels were tortuous and dilated. Similar observations were described in adult ALCAPA patients [2]. The patient’s blood flowed from the RCA to the LCA by the dilated collateral arteries along the external surface of the heart or within the interventricular septum, and then to the main pulmonary artery (MPA).
Surgical correction was performed to restore a two-coronary-artery circulation system. The preferred method in adults, also used in this case, is coronary artery bypass grafting (CABG) with closure of the anomalous left main coronary artery [2]. Surgical repair of the ALCAPA is safe and successfully eliminates symptoms of myocardial ischemia, reducing the risk of malignant arrhythmias and sudden death [2, 3].
With a growing number of guidelines recommending the use of the CCTA like suspected coronary artery disease in patients with low-to-intermediate cardiovascular risk, a higher absolute number of patients with newly diagnosed ALCAPA is expected [4]. Thus, it is necessary to be aware of ALCAPA syndrome to provide the correct diagnosis and treatment.







