Summary
Chemokine CCL5/RANTES is present in early stages of the inflammatory process in patients with out-of-hospital cardiac arrest, which then significantly decreases during mild therapeutic hypothermia. The MTH leads to a decrease in the inflammatory response measured by IL-1β. The level of IL-1β measured during MTH was significantly associated with long-term all-cause mortality. CCL5/RANTES levels correlate with myocardial injury and BNP levels.
Introduction
The most common cause of sudden cardiac arrest (SCA) is acute coronary syndrome (ACS). In Poland, over 177 000 patients died due to cardiac diseases in 2013, which accounted for 45.8% of all deaths [1]. Out-of-hospital cardiac arrest (OHCA) is associated with a particularly poor prognosis and low survival rates. Moreover, these patients are at risk for neurological damage [2, 3]. Post-resuscitation syndrome includes complex damage of individual organs caused by ischemia-reperfusion injury [4]. To protect against organ damage, mild therapeutic hypothermia (MTH), which is defined as a controlled decrease in body temperature to 32–34°C [5, 6], was recently introduced [7, 8].
An Australian study by Bernard et al. and a European study by the Hypothermia after Cardiac Arrest (HACA) working group have documented that the use of therapeutic hypothermia was associated with clinically significant neurological improvement and a 14% improvement in survival 6 months after resuscitation compared to the control group without hypothermia induction (59% vs. 45%, p < 0.02) [5, 6]. The results of these studies have suggested that current guidelines of the European Resuscitation Council (ERC) and the European Society of Cardiology (ESC) recommend therapeutic hypothermia and/or (recently) target temperature management (TTM) in patients with OHCA, regardless of the rhythm which initiated sudden cardiac arrest [9].
However, it is controversial whether MTH might trigger infectious complications through a pro-inflammatory effect (including sepsis) or by creating a “sepsis-like” syndrome via an increase in pro-inflammatory cytokines, including interleukin (IL)-1β, IL-8, and tumor necrosis factor (TNF)-α [10]. A significant correlation has been demonstrated between chemokine (C-C motif) ligand 5 (CCL5), also known as regulated on activation, normal T cell expressed and secreted (RANTES), IL-1β level, and mortality risk in patients with acute coronary syndromes [11–13]. Chemokine CCL5/RANTES level is a marker of coronary artery disease severity [14, 15]. An expanded panel of inflammatory parameters (CCL5/RANTES and IL-1β level) in association with basic measurements (C-reactive protein (CRP), leukocytes, neutrophils) during therapeutic hypothermia may have potential benefits, including prevention of undesirable effects, for optimization of anti-inflammatory therapy or predicting prognosis in patients with ACS complicated by SCA undergoing percutaneous coronary interventions.
Aim
The aim of the study was to evaluate the activity of chemokines which regulate immune cell vascular chemotaxis, including CCL5/RANTES and IL-1β, and their potential impact on 30-day and 180-day prognosis in patients with ACS complicated by SCA treated with coronary angioplasty and MTH.
Material and methods
The study included 33 unconscious patients (27 male, mean age: 66.1 ±10.8 years) admitted after out-of-hospital cardiac arrest as a result of ACS between July 2011 and June 2016. Inclusion criteria were as follows: ACS complicated by OHCA with return of spontaneous circulation (ROSC) and treated using MTH. Patients needed to be > 18 years of age and underwent percutaneous coronary intervention (PCI) of a culprit artery with implantation of a coronary stent. Patients were excluded from MTH if they had a known coagulopathy or active bleeding. All patients had MTH induction in accordance with European Society of Cardiology guidelines [16]. Written informed consent was obtained from patients after regaining consciousness following cardiac arrest. The Jagiellonian University Ethics Committee in Krakow approved the protocol.
Cardiac revascularization and patient management
All patients underwent early PCI and received optimal medical treatment according to current guidelines [17]. Each patient received periprocedural unfractionated heparin intravenously according to weight and dual antiplatelet therapy via a nasogastric tube. During the procedure, GP IIb/IIIa was administered at the discretion of the interventional cardiologist. A drug-eluting stent was implanted in 26 (78.8%) patients, while a bare metal stent was implanted in 4 (12.1) patients. Balloon angioplasty without stent implantation was performed in 2 (6.1%) patients, while in 1 patient, balloon introduction was unsuccessful. SYNTAX score, as well as TIMI scales (pre- and post-PCI), were assessed in all subjects.
Inflammatory biomarkers
Blood samples were drawn from an antecubital vein on admission (T0), at 12–24 h (T1), and 48–72 h (T2) after PCI and placed in a collection tube. Plasma was centrifuged for 15 min at 1600 x γ at 4°C. Collected serum aliquots were immediately stored at ≤ –70°C for further analysis of CCL5/RANTES and IL-1β. Biomarker serum levels were determined by ELISA (Human CCL5/RANTES Immunoassay no. DRN00B, Human IL1β1 Immunoassay R&D systems, Minneapolis, MN, USA) following the manufacturer’s instructions.
Blood sampling
Baseline blood samples, including biochemical tests, CRP, BNP, coagulation, blood gas analysis, and myocardial injury markers were taken on admission to the hospital (T0), and then at T1 (12–24 h) and T2 (48–72 h). Average core temperatures were as follows: at T0 35.4 ±0.6°C; at T1 32.4 ±0.5°C; and at T2 36.6 ±0.4°C.
Mild therapeutic hypothermia protocol
To induce hypothermia, infusion of cold saline (NaCl 0.9% at 4°C) was initiated during PCI. After PCI and transportation to the intensive care unit, therapeutic hypothermia was achieved through the use of an endovascular cooling device (Coolgard, Zoll Medical Corporation Chelmsford, MA, USA). According to the protocol, cooling was maintained for 24 h with a target temperature of 33°C. After reaching the target temperature, rewarming was performed at a rate of 0.2°C/h. All patients during MTH received intravenous injection of an analgesic opioid and a sedation drug. Additionally, neuromuscular blockade (NMB) was often used in accordance with the protocol of MTH.
Patient discharge and follow-up
The primary endpoint was to establish the pattern of CCL5/RANTES and IL-1β changes at 3 time points, and to determine correlations between CCL5/RANTES and IL-1β along with inflammatory, coagulation, and myocardial injury/heart failure biomarkers.
The secondary endpoint was to analyze the relationship between CCL5/RANTES, IL-1β, and the 30-day and 180-day mortality. Neurological outcome was assessed at discharge according to the Pittsburgh Cerebral Performance Category (CPC) [18, 19]. CPC scores 1 and 2 were defined as favorable neurological outcomes, whereas CPC scores 3, 4, and 5 were associated with a poor neurological outcome.
Statistical analysis
The data are presented as mean with standard deviations or medians with interquartile range. Continuous variables were compared with Student’s t-test for normally distributed variables or with the non-parametric Mann-Whitney U test for non-normally distributed variables. The χ2 test was used to compare proportions of categorical variables. Means of the analyzed parameters across groups were tested by analysis of variance (ANOVA).
Correlations were assessed by the Pearson correlation test or by Spearman’s rank test. Survival analysis was performed using Kaplan-Meier curves followed by the log-rank test. All analyses were performed using IBM SPSS Statistics and Statistica 13.0 software. P-values of < 0.05 were considered statistically significant.
Results
Baseline characteristics of study participants are shown in Table I. The all-cause mortality among study participants at 30-day and 180-day follow-up was 18.2% and 45.5% respectively. Sixteen (48.5%) out of the 33 patients had a favorable neurologic outcome at the 30-day observation. At the end of the follow-up period, 17 (51.5%) patients had a favorable neurologic outcome. Laboratory findings on admission, during, and after MTH are summarized in Table II.
Table I
Characteristics of patients undergoing mild therapeutic hypothermia (MTH)
| Variables | MTH* (n = 33) |
|---|---|
| Age [years] | 66.1 ±10.8 |
| Male sex, n (%) | 27 (81.8%) |
| Systolic blood pressure [mm Hg] | 120 (102–147) |
| Diastolic blood pressure [mm Hg] | 80 (65–91) |
| History of hypertension | 25 (75.8%) |
| Diabetes mellitus | 11 (33.3%) |
| Hypercholesterolemia | 20 (60.6%) |
| Obesity | 13 (39.4%) |
| Active smoker | 10 (30.3%) |
| Prior myocardial infarction | 8 (24.2%) |
| Prior PCI | 2 (6.1%) |
| Prior CABG | 2 (6.1%) |
| Prior stroke | 5 (15.2%) |
| Circumstances of sudden cardiac arrest: | |
| Ventricular tachycardia/ventricular fibrillation | 28 (84.8%) |
| Asystole | 3 (9.1%) |
| Pulseless electrical activity | 2 (6.1%) |
| Basic life support/advanced life support | 23 (69.7%) |
| Time to return of spontaneous circulation [min] | 23 ±16 |
| Preserved pupillary reflex | 23 (69.7%) |
| Glasgow Coma Scale ≤ 4 | 21 (63.6%) |
| Glasgow Coma Scale > 4 | 12 (36.4%) |
| Clinical state at admission to hospital | |
| Cardiogenic shock at admission | 8 (24.2%) |
| STEMI | 20 (60.6%) |
| Course of hospitalization: | |
| Time from cardiac arrest to PCI [min] | 122.1 (60.1) |
| Acute coronary occlusion | 16 (48.5%) |
| Extent of coronary artery disease: | |
| 1-vessel | 14 (42.4%) |
| 2-vessel | 10 (30.3%) |
| 3-vessel | 9 (27.3%) |
| Left main stenosis | 1 (3.0%) |
| SYNTAX score | 20 (6.5–29.5) |
| Surgical revascularization | 0 |
| Bare-metal stents used | 4 (12.1%) |
| Drug-eluting stents used | 26 (78.8%) |
| Only balloon angioplasty | 2 (6.1%) |
| Failed PCI | 1 (3.0%) |
| TIMI flow pre-PCI: | |
| 0 | 18 (54.5%) |
| 1 | 1 (3.0%) |
| 2 | 2 (6.0%) |
| 3 | 12 (36.4%) |
| TIMI flow post-PCI: | |
| 0 | 3 (9.1%) |
| 1 | 1 (3.0%) |
| 2 | 0 (0.0%) |
| 3 | 29 (87.9%) |
| Thienopyridine use: | |
| Clopidogrel | 12 (36.4%) |
| Ticagrelor | 21 (63.6%) |
| Cardiogenic shock (after admission) | 17 (51.5%) |
| Intra-aortic balloon counterpulsation 0 | 3 (9.1%) |
| Left ventricular ejection fraction max. | 44 (14.8%) |
| Pneumonia | 24 (72.7%) |
| Blood transfusion | 12 (36.4%) |
| Renal failure | 23 (69.7%) |
| Stroke | 6 (18.2%) |
| Sepsis | 4 (12.1%) |
| 30-day mortality | 6 (18.2%) |
| 180-day mortality | 15 (45.5%) |
| 30-day favorable neurological outcome (CPC 1-2) | 16 (48.5%) |
| 180-day favorable neurological outcome (CPC 1-2) | 17 (51.5%) |
Table II
Standard laboratory, coagulation parameters, peripheral blood gas analysis, myocardial injury markers and immune system parameters on admission (T0) during mild therapeutic hypothermia (MTH) (12–24 h; T1) and during rewarming after MTH (48–72 h; T2)
[i] ALP – alkaline phosphatase, ALT – alanine transaminase, AST – aspartate transaminase, BNP – B-type natriuretic peptide, CK – creatine kinase, CK-MB – creatine kinase-MB (CK-MB), CRP – C reactive protein, DD – D-dimer, GFR – glomerular filtration rate, INR – international normalized ratio, Hb – hemoglobin, hs-TnT – high-sensitivity troponin T, pCO2 – partial pressure of carbon dioxide, pO2 – partial pressure of oxygen, PLT – platelets, RBC – red blood cell, WBC – white blood cells.
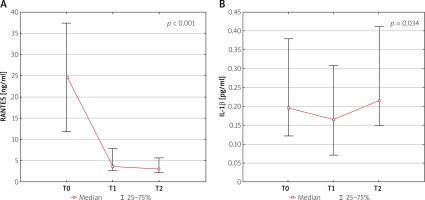
There were significant differences in median serum levels of RANTES as well as IL-1β measured at T0, T1, and T2: 24.69 (Q1:Q3: 11.8–37.5) ng/ml vs. 3.89 (Q1:Q3: 2.6–7.9) ng/ml vs. 2.71 (Q1:Q3: 2.0–5.5) ng/ml; p < 0.001 and 0.196 (Q1:Q3: 0.12–0.38) pg/ml vs. 0.171 (0.07–0.31) pg/ml vs. 0.214 (Q1:Q3: 0.15–0.41) pg/ml; p = 0.034, respectively (Figures 1 A, B).
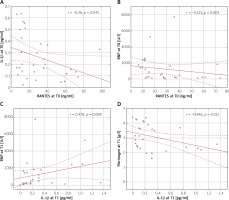
A statistically significant correlation was observed between CCL5/RANTES and IL-1β levels at T0 (r = –0.360; p = 0.045) (Figure 2 A), while there was no statistically significant correlation between these cytokines at T1 and T2 (r = –0.208; p = 0.252 and r = –0.139; p = 0.473, respectively).
CCL5/RANTES level correlated significantly with brain natriuretic protein (BNP) value at T0 (r = –0.521; p = 0.003) (Figure 2 B), while an inverse correlation was observed for IL-1β at T1 and BNP level at T1 (r = 0.478; p = 0.008) (Figure 2 C). IL-1β also correlated with fibrinogen level at T1 (r = –0446; p = 0.012) (Figure 2 D).
There was a significant correlation between IL-1β and SYNTAX score at T1 (r = 0.378; p = 0.033), whereas no correlation between CCL5/RANTES level and SYNTAX score was observed.
Maximum high-sensitivity troponin and CK-MB levels negatively correlated with CCL5/RANTES level at T2 (r = –0.594; p < 0.001 and r = –0.389; p = 0.030, respectively), but not with IL-1β (Figures 3 A, B).
Figure 3
Correlations of RANTES levels at T2 with regard to maximum high-sensitivity troponin and CK-MB levels

Kaplan-Meier survival curves for medians of CCL5/RANTES and IL-1β levels at T0 and T1 were calculated for 30-day and 180-day mortality.
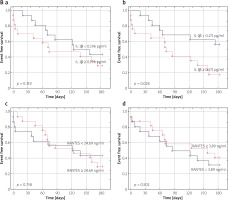
For 30-day survival curves, the levels of IL-1β at T0 and T1 showed a trend to significance with all-cause mortality rate (p = 0.078; p = 0.079, respectively) (Figure 4 A a, b). Levels of CCL5/RANTES at T0 and T1 did not have an influence on 30-day mortality (p = 0.284; p = 0.351, respectively) (Figure 4 A c, d).
Figure 4
A – Kaplan-Meier curves for 30-day mortality stratified according to median levels of IL-1β at T0 (a) and T1 (b) and RANTES at T0 (c) and T1 (d)
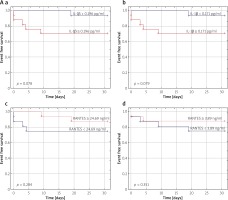
For 180-day survival curves, the level of IL-1β at T1 significantly associated with all-cause mortality (p = 0.028) (Figure 4 B a), whereas IL-1β level at T0 as well as CCL5/RANTES levels at T0 and T1 did not show a statistically significant association with 180-day mortality (p = 0.391; p = 0.758; p = 0.502, respectively) (Figure 4 B b–d).
Discussion
To our knowledge, this is the first prospective study investigating chemokines which regulate immune cell vascular chemotaxis, including CCL5/RANTES and IL-1β, in MTH in patients with cardiac arrest due to ACS treated with PCI.
The main finding of our study is that there are important differences in levels of CCL5/RANTES and IL-1β with regard to time frames. We observed a clear and steady decrease in CCL5/RANTES levels from T0 to T2. This supports the relationship of a chemokine CCL5/RANTES early increase which typically accompanies activation of an intravascular inflammatory response [20].
CCL5/RANTES is mainly produced by T cells, endothelial cells, platelets, and smooth muscle cells and stimulates leukocytes to migrate into inflammatory tissue or into the wall of an injured artery [21]. When released from activated platelets, CCL5/RANTES triggers monocyte migration and arrest to the endothelium in the inflamed or atherosclerotic area [22], and has a significant effect on atherosclerotic lesion size and plaque development. Furthermore, CCL5/RANTES has a role in plaque destabilization and remodeling [23].
In this context, our results suggest that MTH leads to a rapid reduction in CCL5/RANTES levels, which might have a beneficial effect on decreasing the inflammatory response. The same effect was observed for IL-1β during MTH. However, the effect of CCL5/RANTES reduction remained even after patient rewarming, whereas IL-1β levels decreased at T1 and then increased after rewarming of the patient. This might mimic the so-called sepsis-like syndrome, along with an increase in CRP levels, but not in white blood cell count. In line with our findings, MTH was associated with a reduction in immune cell infiltration, apoptosis, IL-1β, and IL-6. Hypothermia reduced myocardial damage and dysfunction after cardiopulmonary resuscitation, possibly via a reduced rate of apoptosis and pro-inflammatory cytokine expression [24].
Of note, it was previously shown that other inflammatory markers including cytokine IL-6 and procalcitonin levels in patients treated with MTH were associated with higher mortality rates measured 24 h after out-of-hospital SCA [25, 26]. The CRP levels on admission were associated with poorer outcomes in a similar group of patients [27]. Our data support these findings, as IL-1β levels were associated with 180-day mortality.
Cavusoglu et al. [28] reported that low baseline CCL5/RANTES levels were an independent predictor of cardiac mortality, with a survival rate of 87.3% in the lowest tertile of CCL5/RANTES values, compared with 94% in the upper 1st and 2nd tertile (p = 0.0298 by log-rank test) in patients referred for coronary angiography [14, 18, 29].
Lipkova et al. observed decreased serum CCL5/RANTES levels in ACS patients, which were associated with the severity of myocardial infarction and progression, with the lowest levels seen in cardiogenic shock patients (cutoff level ≥ 80.4 ng/ml). This strongly suggests a role for CCL5/RANTES as a potential biomarker of cardiogenic shock and acute heart failure in the post-ACS hospitalization phase [30].
In ACS patients with induced MTH, CCL5/RANTES levels did not correlate with 30-day or 180-day mortality. This might be reflected by the fact that the CCL5/RANTES impact on mortality was diminished by a decreased inflammatory process and prohibition of further cardiac remodeling. Of note, CCL5/RANTES levels correlated with cardiac injury and heart failure markers, which still make them potentially valuable, provoking the need for further investigation.
Taken together, this suggests a potentially important role for CCL5/RANTES and IL-1β in patients with ACS and cardiogenic shock. All of the above-mentioned biomarkers correlate with post-MI survival and have an impact on short- and long-term survival [31].
Study limitations
The study group was relatively small and no control group was used due to ethical reasons and the critical status of all patients. However, the overall group size was sufficient to detect correlations. We assessed cytokine levels only via serum gene expression and not through left ventricular tissue gene expression.
Conclusions
The chemokine CCL5/RANTES is present in early stages of the inflammatory process in out-of-hospital cardiac arrest patients, then significantly decreases during MTH. The MTH leads to a decrease in the inflammatory response as measured by IL-1β. The level of IL-1β measured during MTH was significantly associated with long-term all-cause mortality. CCL5/RANTES levels correlated with myocardial injury and BNP levels.