Summary
Until now coronary interventions via the radial artery are usually performed with routine use of spasmolytics. The major finding of our study is that the rate of coronary spasms and occlusions is comparable to rates when those agents are used. Routine use of spasmolytics with evolution of new devices might be limited to selected groups of patients.
Introduction
Radial access dominated coronary interventions across the world and significantly reduced the number of vascular complications [1]. The small number of the observed radial access complications correlates with the experience of the operator and is also related to the type of the access device [2]. The most common complication is the radial artery spasm (RAS) and radial artery occlusion (RAO) [3]. It can be prevented by the appropriate choice of vascular access and minimization of the equipment use.
The use of spasmolytic agents has a strong relation to avoiding vascular access complications. Previous data documented efficacy of various types of vasodilators in preventing radial artery spasm [4–6]. However, with the fast evolution of current devices and the improvement of their flexibility, dimension, deliverability and quality of materials the routine use of spasmolytics should be constantly validated and can be possibly limited only to certain pre-selected groups of patients.
Previous studies analyzed whether use of spasmolytics has a potential to decrease the complications of radial access [7] However, the question arises whether the use of spasmolytic is really necessary during the radial access. The application of vasodilators may not be appropriate in patients with myocardial infarction and low blood pressure, who will benefit from radial access the most. Although the initial results of spasmolytic avoidance are promising, there are just a few reports presenting the safety of the radial access without the application of spasmolytics.
Aim
Therefore, the aim of our study is to assess the feasibility and safety of coronary angiography and percutaneous coronary interventions performed through the radial artery without the routine use of spasmolytic agents.
Material and methods
We conducted a single-center retrospective study. Data were obtained in the First Department of Cardiology of the Upper Silesian Medical Center and represented the period between October 2016 and January 2018. In this period all consecutive patients in whom angiography via the radial artery without routine use of spasmolytic agents was performed were enrolled in the study. It was an all-comers study. The selection of patients was independent from any inclusion or exclusion criteria, and no pre-selection protocol was used. All operators had already stopped using routinely spasmolytic in the radial approach based on their own observations. We analyzed 13% of patients treated via the radial artery in our department in this period (Figure 1).
Radial access technique
All the patients had radial artery pulse palpation without the Allen test performed before the procedure.
All the radial procedures were performed through the right radial artery. None of the patients received premedication. Only 2 ml of lidocaine was injected subcutaneously before the radial artery puncture to adequately anesthetize the puncture site. The radial artery access was achieved by the use of open bore needles, 0.025″ hydrophilic short guidewires and 6 Fr or 5 Fr Balton vascular access sheaths. After the sheath insertion 5 000 IU of unfractionated heparin was injected as a bolus in order to minimize the chance of radial artery occlusion.
In all the patients 0.035″ guidewires were used for advancing the catheters and standard 5 Fr or 6 Fr catheters in all the procedures. Immediately after the procedure the vascular sheath was removed and standard pressure compression bands that were inflated with air until bleeding subsided were used to achieve full hemostasis of the access site.
Spasmolytic agents were only applied during the radial artery spasm. Papaverine, nitrates or verapamil in standard doses were used for that purpose.
Periprocedural assessment
After the pressure band was removed when bleeding resolved completely, not earlier than 3 h after the procedure, every patient had ultrasound assessment of the radial and brachial artery on the next day to assess its maximal and minimal diameter or to detect its occlusion. Every imaging of the radial artery was performed post-procedurally, in cross sectional imaging, by placing the probe 2 cm proximal to the styloid process of the radius, perpendicular to the vessel wall – above the access point. Moreover, every patient was asked to describe pain intensity during the radial procedure on a ten-point scale. Ten points represented the maximal pain intensity and zero corresponded to no pain at all. Occlusion was defined as lack of flow in the radial artery seen in doppler ultrasonography and it was confirmed by simple palpation of the pulse at least 24 h after band removal.
Statistical analysis
Statistical analysis was performed using Statistica 10.0 (StatSoft Poland) software. Continuous variables were presented as mean ± SD and categorical as absolute counts and percentages or as medians with interquartile range (IQR). The type of distribution was verified using the Shapiro-Wilk test. Relationships between variables were checked using the Mann-Whitney U test, χ2 test and analysis of variance (ANOVA). Pearson’s correlation coefficient was used to measure correlations between categorical variables. A p-value of less than 0.05 was considered statistically significant.
Results
Clinical characteristics
Overall 293 patients (M/F 180/113, mean age: 67 ±10) who underwent coronary angiography and coronary interventions through the radial artery approach were analyzed.
Both patients with elective procedures (85/29%) and with urgent interventions (208/71%) in acute coronary syndromes were enrolled in the analysis. Among 293 patients enrolled in the study, 124 (42%) underwent percutaneous coronary intervention with implantation of stent(s).
The following concomitant diseases were present in the study group: systemic hypertension (78%), diabetes mellitus type 2 (26%), hyperlipidemia (57%), and peripheral artery disease (8%). History of previous radial approach was present in 18% of all patients. Detailed characteristics of the study group are presented in Tables I and II. The local Bioethical Commission approved conduction of the study.
Table I
Baseline characteristics of the study population and the subgroups RAS and no-RAS
[i] RAS – radial artery spasm, BMI – body mass index, CAD – coronary artery disease, DMT2 – type 2 diabetes mellitus, HA – arterial hypertension, PAD – peripheral artery disease, HL – hyperlipidemia, MI – myocardial Infarction, PCI – percutaneous coronary interventions, CABG – coronary artery bypass graft.
Table II
Baseline characteristics of the study subgroups RAO and no-RAO
[i] RAO – radial artery occlusion, BMI – body mass index, CAD – coronary artery disease, DMT2 – type 2 diabetes mellitus, HA – arterial hypertension, PAD – peripheral artery disease, HL – hyperlipidemia, MI – myocardial infarction, PCI – percutaneous coronary interventions, CABG – coronary artery bypass graft.
Complications of radial artery access without spasmolytic agents
Among the defined complications of radial artery access, RAS was observed in 55 (18.8%) cases and RAO was diagnosed in 47 (16%) cases. RAS was followed by RAO in 17 cases, which constituted 17 (55%) of all RAS subjects. Only 2 patients had symptomatic occlusion, which required prolonged anticoagulation with complete restoration of patency.
Catheters and radial artery size for RAS and RAO groups
6 Fr catheters were used in 206 patients and 5 Fr catheters were used in 87 patients. There was no difference in the mean diameter of the radial artery between 5 Fr and 6 Fr catheters used for coronary angiography (2.850 (IQR 2.60, 3.21) vs. 2.95 (IQR 2.65, 3.26), p = 0.325). RAS occurred more frequently in 6 Fr as compared to 5 Fr catheters (45 (225) vs. 10 (12%), p = 0.038), and RAO occurred more frequently in 6 Fr (41 (20%) vs. 6 (7%), p = 0.0086).
Clinical characteristics of the study subgroups: RAS vs. no-RAS
The RAS and no-RAS subgroups did not differ in regard to most clinical parameters. History of coronary artery bypass grafting (CABG) was found more frequently in the RAS sub-group as compared to the no-RAS subgroup (13 vs. 4%, p = 0.027) (Table I).
Clinical characteristics of the study subgroups: RAO vs. no-RAO
The RAO and no-RAO subgroups did not differ in regard to most clinical parameters. RAO occurred in younger patients (64 ±10 vs. 68 ±10, p = 0.04) while hyperlipidemia was found more often in no-RAO patients (Table II).
Procedural and peri-procedural data: RAS vs. no-RAS
The occurrence of RAS was significantly higher in prolonged procedures (coronary angiography time 32.6 ±12.8 vs. 29 ±13.5, p = 0.03; total time of coronary intervention time 40 ±23.5 vs. 26.3 ±25, p = 0.0035) and increased proportionally to the number of catheters used (p = 0.08). It was also dependent on time of the local pressure (7.5 ±2.3 vs. 6.5 ±2.8, p = 0.03) (Table III).
Table III
Procedural and peri-procedural data: RAS vs. no-RAS subgroups
Procedural and peri-procedural data: RAO vs. no-RAO
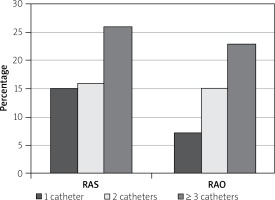
The occurrence of RAO increased proportionally to the number of catheters used (p = 0.01) and was dependent on time of the local pressure (8.6 ±3.5 vs. 6.4 ±2.7) (p = 0.001) (Table IV, Figure 2).
Table IV
Procedural and peri-procedural data: RAO vs. no-RAO subgroups
Regression analysis
Occurrence of RAS was related to the following factors: CABG in case history (R = 0.181, p = 0.027), percutaneous artery angioplasty in LCX (R = 0.263, p = 0.001) or D artery (R = 0.207, p = 0.011). There was also a positive correlation between the occurrence of RAS and the use of 6F catheters (R = 0.197, p = 0.02). Furthermore, the local pressure time correlated with the RAS occurrence (R = 0.244, p = 0.003).
Occurrence of RAO correlated with the following factors: hyperlipidemia (R = 0.181, p = 0.028), CABG in case history (R = 0.203, p = 0.01), in case of atherosclerotic changes (R = 0.72, p = 0.001).
Discussion
The main reason for the increasing popularity of the radial approach is the simplicity of achieving effective hemostasis of the superficially running radial artery and reduction in the complications rate. Radial access compared to femoral is more comfortable for patients, enables quick start-up after the procedure, and shortens the length of hospital stays. Furthermore, studies showed a significant decrease in the frequency of hemorrhagic complications in radial access [8]. In a randomized study, the incidence of arterial contraction was lower through the arterial administration of nitroglycerine or nitroglycerine combined with verapamil [4]. However our study proved that transradial coronary angiography and revascularization is both safe and feasible without routine initial use of spasmolytic agents.
In our study we had to make conversion to a femoral approach because of severe spasm only in 4.5% of patients of 293 patients enrolled in the study. The rate of access conversions remained at the same level irrespective of the use of spasmolytic agents. Our data are in line with the rate of conversion observed in routine application of spasmolytic agents. The metanalysis of 23 randomized studies comparing radial with femoral access in diagnostic and therapeutic coronary procedures mainly with spasmolytic agents reported a trans-radial approach failure rate of 5.9% [9].
Our study showed that the spasm and occlusion rate did not differ in regard to sex. This finding is contrary to a previous observation that women tend to have radial artery spasm more often. It was shown in our study that radial artery occlusion happened more often in younger patients. One possible explanation of the mechanism is that younger patients took periprocedurally smaller amounts of anticoagulation and antiplatelet agents because of fewer comorbidities.
History of CABG was found more frequently in the RAS. To perform coronary artery angiography in patients after CABG, the left radial access is required. Since operators are more familiar with right radial artery access, the left might have required a large number of attempts and thus provoke spasm. Unfortunately, we did not perform such thorough analysis and cannot prove this speculation. Furthermore, more frequent catheter changes are required to perform coronary angiography after CABG and longer procedural time might have also provoked RAS. Larger devices and their quantity may according to optical coherence tomography study lead to microdissections at the radial access site and also be a potent risk factor for radial artery occlusion [10]. As observed in our study, the presence of ultrasonographic evidence of atherosclerosis in the radial artery was more frequent among those who developed spasm or arterial occlusions. Radial arteries with atherosclerosis are more prone to damage and occlusion because of aforementioned dissection. It may be speculated that prolonged pressure promotes thrombus formation and thus results in total artery occlusion. Our finding is in line with previous studies showing that prolonged hemostasis was an independent predictor of radial artery occlusion [11]. Achieving good hemostasis without prolonged compression is a challenge after radial artery procedures. Probably novel, more advanced devices will help to solve this issue.
It was not a randomized study, but an all-comers one without a control group of patients, to whom spasmolytics were not administered during the procedure.
Conclusions
Our study showed that angiography and interventions performed through the radial artery without routine use of spasmolytic agents seem to be feasible and relatively safe. In this approach the occurrence of RAS and/or RAO is related to standard independent risk factors and comparable to data from the literature when spasmolytics were used. Thus, their routine application may be significantly limited or even avoided on a daily clinical basis in selected patients.