Summary
Percutaneous coronary intervention in small vessel disease is challenging due to high rates of target vessel revascularization. In this report of the BASKET-SMALL 2 trial analyzing the results of a drug-coated balloon (DCB) vs. drug-eluting stent strategy in small vs. very small coronary vessels, there was no overall difference regarding safety and efficacy of DCB in different vessel sizes. However, patients treated with DCB showed significantly better results in very small vessels than patients treated with paclitaxel-eluting stents, while similar results were obtained in small vessels.
Introduction
Percutaneous coronary intervention (PCI) using drug-eluting stents (DES) is the treatment of choice for coronary artery disease. However, in certain anatomical subsets, the efficacy and safety of stents are limited. Here, vessel size is an important predictor of events – as a rule of thumb, the smaller the stent, the worse the result after PCI; this is true for all bare metal stents (BMS) [1], first-generation DES [2, 3] and second-generation DES [4, 5]. In this context, the concept of avoiding metal implants in the vessel was introduced in order to improve PCI results. While the use of bioresorbable scaffolds [6] failed to bring better results in treating small coronary arteries, a strategy of implant-free PCI using drug-coated balloons (DCB) was tested in a large-scale clinical trial powered for clinical endpoints and was non-inferior to second-generation DES [7]. DCB are semi-compliant balloons coated with an active drug, e.g., paclitaxel or sirolimus, which usually is embedded in a matrix and rapidly transfers into the vessel wall during inflation. The drug locally acts as an antiproliferative agent in the vessel wall to prevent neointimal hyperplasia and negative remodeling [8]. While DCB mostly are used for the treatment of in-stent-restenosis [9], which is an indication that entered the 2014 guidelines as an official recommendation [10], newer data from randomized controlled trials [11–13] show a good efficacy and safety profile in de-novo stenosis in small coronary vessels.
Aim
The aim of the current analysis is to explore the efficacy and safety of DCB vs. the other devices used, e.g., second-generation paclitaxel-eluting stents and everolimus-eluting stents, in the treatment of different sizes of small coronary arteries within the BASKET-SMALL 2 trial.
Material and methods
Design
BASKET-SMALL 2 was a prospective, randomized, open-label, non-inferiority, multicenter study performed in 14 centers in Switzerland, Germany and Austria between April 10, 2012, and February 1, 2017 [7, 14, 15]. The study was performed according to the Declaration of Helsinki and Good Clinical Practice guidelines. The ethics committees in all participating centers approved the protocol. The present analysis is a subgroup analysis as pre-specified in the protocol.
Participants
All enrolled patients had an indication for PCI in a small coronary vessel (> 2.0 and ≤ 2.75 mm). All treated lesions had to be successfully predilated as outlined in current expert consensus recommendations [16], i.e., with absence of residual stenosis > 30%, high grade dissections (C-F) and TIMI flow < 2. Patients with other, larger lesions > 2.75 mm in the target vessel, in-stent restenosis, contraindication for antiplatelet therapy, life expectancy less than 12 months and unable to give written consent were excluded. Patients were analyzed according to the size of the device used (very small ≤ 2.5 mm vs. small > 2.5 mm). These groups were used based on the available sizes of the devices and the similar group sizes when using this dichotomization.
Randomization and masking
An interactive internet-based system was used to randomize patients in 1 : 1 fashion (DCB vs. DES). As an open label study, the treating physicians and patients were not masked from the method of treatment.
Procedures
After successful predilation, patients were treated with either a paclitaxel-coated balloon (Sequent Please; B Braun Melsungen AG, Melsungen, Germany) or a second-generation DES, i.e., a paclitaxel-eluting stent (Taxus Element; Boston Scientific, Natick, MA, USA) or an everolimus-eluting stent (Xience; Abbott Vascular, Santa Clara, CA, USA). The size of the device was chosen by the operator with a ratio of 0.8 to 1.0 to the visually estimated vessel size, with no differences between DCB and DES; of note, there was no quantitative coronary angiography used for the selection of the device.
The study was started with second generation paclitaxel-eluting stents (strut thickness 81 μm), with the idea that both devices used carry the same active drug. After the paclitaxel-eluting stent was not available anymore in the German market in 2013, the comparator group was changed to an everolimus-eluting stent (strut thickness 81 μm). Accordingly, the sample size was adapted. PCI was done according to the guidelines: The dilatation of the DCB was done for 30–60 s, and the DCB had to be 2–3 mm longer on each side than the balloon used for predilatation. In case of relevant residual stenosis > 30% or flow limiting dissections after DCB, the implantation of DES was allowed. After PCI, dual antiplatelet therapy was prescribed using clopidogrel 75 mg for 4 weeks in the DCB arm and 6 months in the DES arm, and ASS 100 mg in both arms. In case of an acute coronary syndrome, patients received P2Y1 receptor antagonists in the form of clopidogrel, prasugrel (10 mg daily) or ticagrelor (90 mg twice daily) for 12 months. We followed the guidelines when oral anticoagulation was needed [17].
Outcome and follow-up
The primary endpoint was major adverse cardiac events (MACE), while secondary endpoints were target vessel revascularization (TVR), non-fatal myocardial infarction, cardiac death, and all-cause mortality, all at 36 months. Follow-up was done at 6, 12, 24 und 36 months after the intervention using a verbal or written clinical and quality of life questionnaire. All events were adjudicated by an independent events committee.
Statistical analysis
All statistical analyses were performed on the full analysis set of patients who underwent the 1- and 3-year analysis, according to the intention-to-treat principle (i.e. all patients were analyzed on the basis of the treatment they were randomly allocated to). For the two subgroups of very small and small vessels, the baseline variables are summarized. Categorical data are presented as frequencies and percentages (with the effect of the grouping analyzed by Pearson’s χ2 test). For numerical variables, the median and interquartile range or the mean and standard deviation are presented, as appropriate (with the effect of the grouping examined by Student’s t-test or the Wilcoxon-Mann-Whitney test, respectively). Treatment effects on the times to event within 1, 2, and 3 years were tested by Cox regressions (with study center as a stratifying factor to account for differences in baseline hazards between study centers) for the following events: all-cause death, MACE, which is the composite of cardiac death, non-fatal myocardial infarction, and TVR. The Cox regressions were performed within each of the above subgroups, as well as globally when controlling for each grouping variable separately (both models with and without interaction between treatment and grouping variable were fitted).
The assumptions of proportional hazards and homogeneity of treatment effects among study centers in the Cox models were checked (by testing the correlation of the scaled Schoenfeld residuals with time and the interaction of the stratifying factor study center with treatment in the Cox models, respectively) and are tenable. Missing data were not an issue, since the endpoints of patients not experiencing an event were considered as censored on the last observation date. The analyses were conducted using the statistical software package R [18], using “two-sided” statistical tests and confidence intervals. No correction for multiple testing was applied, since the statistical analyses are explorative.
Results
Of the 758 patients who were randomly assigned for treatment, 382 were assigned to the DCB group and 376 to the DES group. Twenty (5%) patients treated with DCB had to be treated with DES due to > 30% rest stenosis or flow limiting dissections.
Overall, 437 (58%) patients were treated with very small devices (diameter ≤ 2.5 mm). Those patients had higher prevalence of hypertension, insulin-dependent diabetes mellitus and peripheral arterial occlusive disease compared with patients treated with small devices. The other clinical and angiographic characteristics were equally distributed between both groups (Table I).
Table I
Baseline clinical and angiographic characteristics according to vessel size
[i] Categorical variables are shown as frequencies and percentages, numerical variables as mean and standard deviation (except for ejection fraction perc. as median and interquartile range); with p-values obtained by Pearson’s χ2 test and Student’s t-test, respectively (Wilcoxon-Mann-Whitney test for ejection fraction perc). Missing values are ignored, for each variable separately, but the percentage of missing values is reported for each variable.
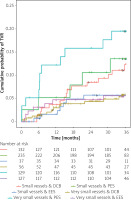
In the very small vessel group, neither rates of MACE (DCB vs DES, hazard ratio (HR) = 0.82, 95% confidence interval (CI): 0.49, 1.39, p = 0.468), cardiac death (HR = 1.36, 95% CI: 0.56, 3.31, p = 0.502), non-fatal myocardial infarction (HR = 0.66, 95% CI: 0.27, 1.57, p = 0.342), TVR (HR = 0.63, 95% CI: 0.31, 1.29, p = 0.209), nor all-cause death (HR = 1.14, 95% CI: 0.58, 2.24, p = 0.697) were different at 3 years. Similarly, in the small vessel group, neither rates of MACE (DCB vs. DES, HR = 1.31, 95% CI: 0.74, 2.32, p = 0.355), cardiac death (HR = 1.07, 95% CI: 0.28, 4.07, p = 0.916), non-fatal myocardial infarction (HR = 1.16, 95% CI: 0.49, 2.76, p = 0.734), TVR (HR = 1.58, 95% CI: 0.77, 3.23, p = 0.208), nor all-cause death (HR = 0.76, 95% CI: 0.30, 1.96, p = 0.575) were different at 3 years. Rates of MACE (Figure 1) and TVR (Figure 2) were similar in all groups with the numerically lowest rates at 3 years in very small vessels treated with DCB and the highest rates in small vessels treated with DCB. Interaction between vessel size and treatment was assessed for the different outcome measures and was not significant for MACE (p = 0.259), cardiac death (p = 0.763), non-fatal myocardial infarction (p = 0.373), or all-cause death (p = 0.495). However, there was a trend for a beneficial interaction between very small vessels and DCB treatment regarding TVR after 1, 2 and 3 years of follow-up (1-year HR = 0.24, 95% CI: 0.05, 1.16, p = 0.077; 2-year HR = 0.37, 95% CI: 0.12, 1.15, p = 0.085; 3-year HR = 0.39, 95% CI: 0.14, 1.08, p = 0.070).
Figure 1
Kaplan-Meier estimates of the cumulative probabilities of MACE during 3 years in the 4 combinations of subgroups and study arms
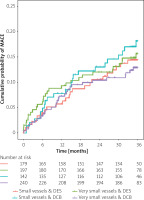
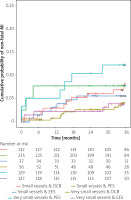
Figure 2
Kaplan-Meier estimates of the cumulative probabilities of TVR during 3 years in the 4 combinations of subgroups and study arms
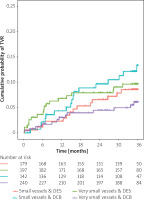
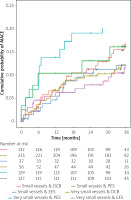
Overall, 95 patients (25% of the DES group, 12.5% of all patients) were treated with second generation paclitaxel-eluting stents (Table II). In the very small vessel size group, rates of MACE at 3 years (HR = 2.03, 95% CI: 1.03, 3.99, p = 0.041; Figure 3), TVR (HR = 3.32, 95% CI: 1.45, 7.59, p = 0.004; Figure 4) and non-fatal myocardial infarction (HR = 2.95, 95% CI: 1.07, 8.11, p = 0.036; Figure 5) were higher in the paclitaxel-eluting stent very small group compared with the other groups. In the small vessel size group there were no statistically significant differences between the groups. There were no significant differences regarding MACE, TVR, cardiac death and non-fatal myocardial infarction between DCB and everolimus-eluting stents in the two vessel size groups.
Table II
Comparison of event numbers and Kaplan-Meier estimates of event rates between devices within each subgroup for all endpoints. Hazard ratios (HR), confidence intervals (CI), and p-values from Cox regressions stratified by study center
Figure 3
Kaplan-Meier estimates of the cumulative probabilities of MACE during 3 years in the 6 combinations of subgroups and devices
Discussion
The main findings of this pre-defined subgroup analysis of the BASKET-SMALL 2 trial are that (1) DCB have a similar efficacy and safety profile irrespective of vessel size, and that (2) the beneficial effect of DCB over second generation paclitaxel-eluting stents regarding TVR, non-fatal myocardial infarction and MACE is more pronounced in very small than small coronary arteries.
Small coronary arteries are the target of interventional treatment in up to 30% of cases. Although current generation DES usually achieve very good results, a higher incidence of restenosis and cardiac events is found in small vessel disease. Geometric considerations are one reason for this finding, since relative lumen narrowing increases with smaller vessels for the same late lumen loss [19]. Therefore, very small coronary vessels ≤ 2.5 mm may be expected to have higher event rates than small vessels > 2.5 mm.
Operative treatment of small coronary arteries was also associated with increased risk of mortality [20].
Our findings concur with published literature. The BELLO trial [12] compared paclitaxel-eluting stents (Taxus Liberté, Boston Scientific, Boston MA) with paclitaxel-coated balloons (IN.PACT Falcon, Medtronic, Inc., Santa Rosa CA) and showed that DCB are associated with less angiographic late loss and similar rates of restenosis and revascularization as a DES. In this trial, there were similar results for smaller vs. larger vessels (< 2.25 mm vs. 2.25–2.5 mm), and there was no interaction between different reference vessel diameters and treatment modality regarding late lumen loss (p = 0.12). The RESTORE SVD China trial randomized 230 patients to paclitaxel-coated DCB (RESTORE, Cardionovum, Bonn, Germany) or zotarolimus-eluting DES (RESOLUTE integrity, Medtronic, Minneapolis MN) in lesions ≥ 2.25 mm and ≤ 2.75 mm and showed non-inferiority of DCB vs. DES regarding 9-month in-segment percentage diameter stenosis [13]. In this trial, there was a nested registry of patients with a vessel size between 2.0 and 2.25 mm; these patients were all treated with DCB. Although there was no formal statistical comparison with the main trial, results in the nested very small vessel size registry were similar as in patients with larger vessels treated with DCB. The PICCOLETO II trial randomized 232 patients with de-novo lesions < 2.75 mm to a paclitaxel-coated DCB (Elutax SV, Aachen Resonance, Germany), or an everolimus-eluting stent (Xience, Abbott Vascular, Santa Clara, California). The DCB group had a significantly lower late lumen loss than the DES group (0.04 vs. 0.17 mm, p = 0.001), while minimal lumen diameter and diameter stenosis showed no difference. After 12 months MACE occurred in 7.5% in the DES group and 5.6% in the DCB group, which was not statistically significant, and there were numerically more myocardial infarctions and vessel thromboses in the DES arm [21]. Finally, in a long-term registry of DCB patients with de-novo coronary artery disease [22], vessel size was not associated with target lesion revascularization (p = 0.642). Taken together, these data concur with the results of our trial and confirm a similar efficacy of DCB in both very small and small vessel size. However, it can be speculated that the phenomenon of late lumen enlargement, which has been described with the use of paclitaxel-eluting balloons earlier, could have played a role here [19]. Effects that have been described in this context are vessel growth and plaque regression induced by paclitaxel; however, in the absence of angiographic follow-up within BASKET-SMALL 2 this cannot be specified further.
Another interesting finding of the present analysis is the significantly higher rates of MACE, TVR und non-fatal myocardial infarctions in patients with very small vessels treated with paclitaxel-eluting stents. Previous data in vessels between 2.5 mm und 4.25 mm were published in the context of the SPIRIT II [23] and III [24] trials. SPIRIT II proved that everolimus-eluting stents are superior to paclitaxel-eluting stents; a post-hoc analysis in vessels < 2.75 mm [25] showed significantly better rates of MACE, target lesion revascularization, and myocardial infarction (p = 0.02). Similarly, in a diabetic population undergoing PCI in a vessel size < 3.0 mm, everolimus-eluting stents proved superior to paclitaxel-eluting stents [26]. In a meta-analysis [27] of SPIRIT II, III and IV that included 1019 patients, a clear benefit of everolimus-eluting over paclitaxel-eluting stents in terms of event-free survival in small vessels was found.
Previously, the safety of DCB was questioned in a population undergoing interventional treatment of peripheral arterial occlusive disease [28]. However, no sign of increased mortality was found in large meta-analyses in the coronary field [29], while the reason for cardiac death was not associated with DCB in a subgroup analysis of BASKET-SMALL 2 [30]. In the current analysis, safety of DCB was similar in very small and small coronary arteries with low rates of death and cardiac death in all treatment groups.
This study provides evidence of a potential benefit of DCB in very small vessels. The majority of interventional cardiologists do not treat these vessels because of the historical non-promising data from the era of BMS and first generation DES. However, most of the published studies evaluating the effect of DCB on native coronary vessels (including BASKET-SMALL 2) were designed with a definition of a small vessel size ≤ 2.75 mm. Nowadays, a major part of current practice is the treatment of patients who are non-operable due to advanced age or comorbidities. Our study shows that there might be a new option for these patients with lesions in very small coronary arteries.
Our subgroup analysis is subject to inherent limitations. One limitation may be the small number of patients in the different subgroups. Another limitation is the missing angiographic follow-up and the quantitative coronary angiography (QCA); however, BASKET-SMALL 2 was a clinical study without pre-specified follow-up angiography. Next, the cut-off between the two analyzed groups was set deliberately at 2.5 mm; however, this was done based on the available devices and resulted in two groups that were distributed equally. As a post-hoc analysis of a randomized controlled trial, we could not perform post-hoc power calculation according to the small sample size in our subgroup analysis. The main trial was powered to detect non-inferiority regarding clinical endpoints at 1 year between DCB and DES.
Conclusions
Efficacy and safety of DCB in the treatment of de-novo coronary small vessel disease are similar irrespective of vessel size. DCB showed significantly better results in the group with very small vessels in terms of TVR, MACE and non-fatal myocardial infarction compared to paclitaxel-eluting stents. Further research in a population with very small native coronary arteries (≤ 2.5 mm) is warranted to elucidate the efficacy of DCB in this group of patients.