Iatrogenic aortic dissection (IAD) is a rare complication of catheter-based coronary procedures. It occurs with a frequency of 0.006% during coronary angiography and 0.098% during interventional procedures [1]. It more often concerns the right coronary artery (RCA) and patients with acute coronary syndrome. In 2000, Dunning et al. divided IAD into 3 types [2]. Class 1 was limited to the aortic sinus, class 2 involved less than 4 cm of the ascending aorta and class 3, the most dangerous, exceeded 4 cm in length. Therapeutic recommendations for IAD are still scarce, but recent reports suggest that even class 3 IAD can be treated conservatively or by placing a stent [1, 3]. We would like to present a case of iatrogenic aortic dissection (Dunning class 3) as a complication of RCA angioplasty.
A 63-year-old woman with a history of unstable angina (UA) treated with percutaneous coronary intervention (PCI) of the circumflex artery with drug-eluting stent (DES) implantation, type 2 diabetes mellitus, hypertension and hyperlipidemia was admitted for the scheduled coronary angiography due to return of anginal symptoms (CCS class III). Prior to the catheterization, an echocardiogram showed a preserved ejection fraction (60%), no regional wall motion abnormalities and correct valve function. Coronary angiography performed through the right radial access revealed 90% stenosis with moderate calcification in proximal and middle segments of the right coronary artery and no significant lesions in the left coronary artery. Whilst engaging the catheter into the right coronary ostium (Amplatz Left 1.0 6F), aortic sinus dissection occurred (Figure 1 A). The patient remained hemodynamically stable and asymptomatic. After immediate cardiosurgical consultation, a decision of a non-surgical approach and continuing angioplasty was made. At that time, the guidewire had not been inserted yet. The catheter was changed to be less traumatizing (Amplatz Right 1.0 6F) and two DES were implanted (Promus Premier 3.0/24 mm and 3.0/28 mm). The first one sealed the entry site of the dissection, while the second stent was implanted distally, after the insertion of the guide extension catheter (Guideliner 6F) to minimize the traumatization of the sinus (Figure 1 B). The pain-free and hemodynamically stable patient was transferred to the intensive cardiac care unit. On admission, transthoracic echocardiography (TTE) demonstrated thickening of the walls of the aorta from the right Valsalva sinus, no pericardial effusion and no aortic insufficiency. Emergent computed tomography (CT) showed intramural hematoma with dimensions 5 × 95 mm, starting at the level of the right coronary cusp and ending a short distance from the brachiocephalic trunk (Figure 1 C). To minimize shear forces and prevent propagation of the dissection, intensive hypotensive therapy, including nitroglycerin infusion and β-blocker, was used. Aspirin and clopidogrel were continued. During a further stay in the ward, the patient was stable and had no dissection symptoms. Two consecutive CTs revealed a small resolution of the hematoma. Twelve days after PCI the patient was discharged. Follow-up CT done 1 month later showed complete resolution of the hematoma (Figure 1 D).
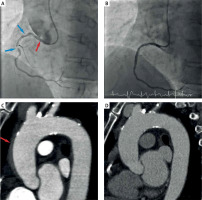
Figure 1
A – Angiography imaging: 90% stenosis in proximal and middle segments of the right coronary artery (blue arrow) and sinus dissection (red arrow), B – final angiography of the treated right coronary artery, C – computed tomography: intramural hematoma with dimensions 5 × 95 mm (red arrow), D – computed tomography: resolution of the hematoma
The management for IAD, especially extensive, is still unclear. This example confirms that even for class III IAD a non-surgical approach with stent deployment can be a proper choice.







