Introduction
With the advance of minimally invasive techniques in abdominal surgery, laparoscopic cholecystectomy (LC) due to the advantages of small trauma, fast recovery, less postoperative complications, and other features has become the standard procedure for benign gallbladder lesions. However, in some cases, LC may be very difficult and hence converted to laparotomy, causing patients much pain and prolonging the prognosis time [1, 2]. Hence, evaluating the difficulty of LC before operation is extremely important.
Aim
The aims of the study were to explore risk factors of difficult cholecystectomy (DC) and to establish a risk prediction model of DC, in order to reduce the risk of LC.
Material and methods
Participants
We performed a retrospective cohort study of patients who received cholecystectomy in the department of our hospital and divided the difficulty of operation by quartile.
Inclusion criteria: (1) Preoperative transabdominal ultrasound and magnetic resonance cholangiopancreatography (MRCP) clearly diagnosed as gallstone and gallbladder polyp or acalculous cholecystitis. (2) Stone diameter > 1 cm or gallbladder polyps diameter > 1 cm or multiple gallstones.
Exclusion criteria: (1) Complicated with intrahepatic and extrahepatic bile duct stones, Mirizzi syndrome, or acute pancreatitis; (2) complicated with serious basic diseases and difficulty tolerating surgery; (3) intraoperative anaesthesia effect was not ideal; (4) insufficient carbon dioxide pneumoperitoneum; and (5) key device fault.
Group standard
For mature surgeons, the time of operation usually reflects the difficulty of LC. Okamura et al. [3] considered that blood loss volumes in the 75th percentile or above as risk factors for bleeding in open repeat hepatectomy, so we selected the upper quartile (P 75) of operation time as the segmentation point of grouping: Patients with operation time ≥ P 75 were assigned to the DC group and those with < P 75 were assigned to the NLC group. We also compared the differences of intraoperative blood loss, frequency of vomiting in the first 24 h after operation, rate of conversion to laparotomy, drainage tube placement rate, etc. of the 2 groups, which were conducive to further evaluation of the rationality and authenticity of this method in grouping.
Surgery
After all patients received general anaesthesia and endotracheal intubation, a CO2 pneumoperitoneum was established and the pressure of 12 mm Hg (1 mm Hg = 0.133 kPa) was maintained. Then, routine 4-port LC was conducted by our fixed surgical team. In the case of extensive intra-abdominal adhesions, unclear anatomy of gallbladder triangle, ineffective control of bleeding, or accidental bile duct injury, LC must be converted to laparotomy in time to ensure the safety of operation.
Observed indicator
Based on our clinical experience, data that could be evaluated before operation, such as body mass body mass index (BMI), white blood cells (WBC), the frequency of recent cholecystitis, history of abdominal operation, history of abdominal inflammation, etc., were selected as risk factors for analysis. This study was approved by the ethics committee of our hospital.
Statistical analysis
All statistical analysis was performed with Statistical Package for the Social Sciences (version 24.0, SPSS Inc.). Difficulty of operation was divided by quartile method. Quantitative variables that satisfied normal distribution were expressed as mean and standard deviation (SD), which were compared with Student’s t-test and analysis of variance. Quantitative variables that dissatisfied normal distribution were expressed as M(P 25, P 75), which were compared using the Mann-Whitney U test. Qualitative variables were described using the frequency and percentage. The χ2 test and Fisher’s precision probability test were performed to assess the significance of qualitative comparisons. Multivariate logistic regression analysis was used to screen independent risk factors. A prediction model of DC was established and evaluated by Hosmer-Lemeshow test and receiver operating characteristic (ROC) curves. The value of p < 0.05 was considered statistically significant.
Results
The operation time of 201 patients was 20–240 min and the P 75 was 70 min. Ultimately, 148 patients were classified into the NLC group (all completed under laparoscopy), whose ages were 22–89 years and BMIs were 18.26–33.65 kg/m2, while 53 patients were classified into the DC group (50 patients underwent laparoscopy and 3 patients underwent laparotomy), whose ages were 20–85 years and BMIs were 19.11–36.57 kg/m2. There was no significant difference in basic data between the 2 groups (p > 0.05) (Table I).
Table I
Comparison of basic data between the NLC and DC groups
| Group | N | Male | Age [years] | BMI [kg/m2] |
|---|---|---|---|---|
| NLC group | 148 | 43 (29.1) | 50.97 ±15.94 | 25.97 ±3.44 |
| DC group | 53 | 17 (32.1) | 51.06 ±14.64 | 26.40 ±3.71 |
| χ2 or t | 0.170 | 0.036 | 0.765 |
Compared with the NLC group, the DC group had increased intraoperative blood loss, postoperative 24 h vomiting frequency, rate of conversion to laparotomy, rate of drainage tube placement, postoperative first exhaust time, and hospital stay (p < 0.05). There was no significant difference in the incidence of postoperative shoulder pain and incision infection rate between the 2 groups (p > 0.05) (Table II).
Table II
Comparison of perioperative indicators between the 2 groups
| Group | NLC group (n = 148) | DC group (n = 53) | Z, χ2, or t |
|---|---|---|---|
| Operation time [min] | 45.0 (35.3, 52.0) | 81.0 (70.0, 120.0) | 10.803** |
| Intraoperative blood loss [ml] | 5.0 (2.0, 10.0) | 10.0 (7.5, 20.0) | 7.308** |
| Conversion to laparotomy (%) | 0 | 3(5.7) | 0.018▲ |
| Drainage tube placement (%) | 32 (21.6) | 20 (37.7) | 5.284* |
| Frequency of postoperative 24-h vomiting (n) | 1.0 (0, 2.0) | 3.0 (1.0, 4.0) | 5.099** |
| Postoperative shoulder pain (%) | 11 (7.4) | 7 (13.2) | 1.596 |
| Postoperative first exhaust time [h] | 20.17 ±4.16 | 42.45 ±5.19 | 28.179** |
| Hospital stay [days] | 6.5 (6.0, 8.0) | 8.5 (7.5, 10.5) | 5.073** |
| Incision infection (%) | 1 (0.7) | 1 (1.9) | 0.459▲ |
The results of BMI > 25 kg/m2, WBC > 10 × 109/l, history of gallbladder puncture, calculus incarcerated in the neck of the gallbladder, frequency of acute cholecystitis in the last 2 months > 4 times, thickness of gallbladder wall > 0.5 cm, and the maximum diameter of gallstone > 2 cm in the 2 groups were significantly different (p < 0.05) (Table III).
Table III
Results of univariate analysis on DC
| Group | NLC group (n = 148) | DC group (n = 53) | χ2 |
|---|---|---|---|
| BMI > 25 kg/m2 | 52 (35.1) | 35 (66.1) | 15.181** |
| WBC > 10.0 × 109/l | 3 (2.0) | 6 (11.3) | 5.858* |
| History of gallbladder puncture | 6 (4.1) | 10 (18.9) | 9.755** |
| History of ERCP | 7 (4.7) | 7 (13.2) | 3.119 |
| History of pancreatitis | 8 (5.4) | 8 (15.1) | 3.765 |
| Calculus incarcerated in neck of gallbladder | 5 (3.5) | 7 (13.2) | 5.079* |
| Acute cholecystitis in the last 2 months > 4 times | 13 (8.8) | 29 (54.7) | 49.813** |
| Thickness of gallbladder wall | 3 (2.0) | 10 (18.9) | 15.618** |
| The maximum stone diameter > 2 cm | 17 (11.5) | 19 (35.8) | 15.754** |
By constructing the logistic function between the dependent variable of difficulty of operation and the argument of BMI > 25 kg/m2, WBC > 10.0 × 109/l, history of gallbladder puncture, calculus incarceration in neck of gallbladder, cholecystitis attack times, thickness of gallbladder wall, and the maximum diameter of the gallstone, we obtained the following regression equation: Logit (P) = –3.426 + 1.291X1 + 2.4002X2 + 1.5644X4 + 2.7225X5 + 2.4866X6 + 2.3237X7 and the following predictive value equation: P = 1/[1 + e-(–3.426 + 1.291X1 + 2.400X2 + 1.564X4 + 2.722X5 + 2.486X6 + 2.323X7)] (Tables IV and V).
Table IV
Variable assignment table
Table V
Multivariate analysis of risk factors in DC
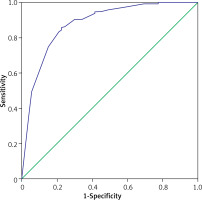
The Hosmer-Lemeshow test was used to evaluate the goodness-of-fit of the logistic regression model, and the results showed that the regression equation was in high matching (χ2 = 1.457, df = 5, p > 0.05). The results showed that the total area under the curve was 0.879, the optimal critical value was 0.686, the sensitivity was 94.3%, the specificity was 52%, and the 95% CI was 0.822–0.933; p < 0.01. It was considered that the model was reasonable and suitable for the prediction of clinical risk (Figure 1).
Discussion
LC, as a mature technology, has become the standard operation for cholecystectomy, but severe complications such as biliary tract injury [4, 5], biliary fistula, and abdominal infection may still occur during and after operation, which may increase the pain and economic burden to patients [6]. Thus, how to effectively predict and evaluate the difficulty and risk before surgery are the focus of our study. By analysing the risk factors of DC and building a prediction model, our study hopes to help clinicians carry out LC more safely and efficiently.
The results of our study show that intraoperative blood loss, rate of conversion to laparotomy, rate of postoperative drainage tube placement, frequency of postoperative 24 h vomiting, time of first postoperative exhaust, and length of hospital stay in the DC group were significantly greater than those in the NLC group, which further reflected the rationality of using P75 to measure the difficulty of cholecystectomy. Considering that the experience of surgeons often directly affects the operation time [7, 8], we selected a fixed and experienced surgical team to perform all operations, to reduce the influence of anthropic factors on operation time. In addition, unsatisfactory intraoperative anaesthesia, poor intraoperative carbon dioxide pneumoperitoneum, and intraoperative machine malfunction were also excluded to ensure the rationality of case selection.
Our study found that BMI > 25 kg/m2, thickness of gallbladder wall > 0.5 cm, and frequency of acute cholecystitis in the last 2 months > 4 times were independent risk factors for DC. We believe that the reasons and possible solutions for these risk factors are as follows:
Obesity. The hypertrophy of abdominal wall in obese patients makes it difficult for routine trocar to reach an ideal position in the abdominal cavity due to its insufficient length, thus affecting the operation process. Obese patients are often accompanied by physiological enlargement of the caudate lobe of the liver and accumulation of adipose tissue in the triangle of the gallbladder, which also result in increased difficulty of exposure of the gallbladder duct and extrahepatic bile duct [9]. Therefore, a longer trocar should be selected for puncture in patients with hypertrophy of the abdominal wall. When the caudate lobe covers the surgical area, the assistant can use noninvasive grasping forceps to raise the caudate lobe. When the gallbladder triangle is filled with adipose tissue, surgeons can open the gallbladder serosa first then use an electric coagulation hook to separate tissue along the pipe line direction and use an aspirator to gently peel back the surrounding tissue, until fully exposing the cystic duct, common bile duct, and hepatic duct.
Thickening of the gallbladder wall. Patients with chronic inflammation, atrophy, and acute inflammation of the gallbladder may have varying degrees of gallbladder wall thickening [10]. Thickening of the gallbladder wall can increase the difficulty of grasping, so it is necessary to select toothed grasping forceps to grasp the gallbladder, or cut the gallbladder wall with an electric coagulation hook and then put the grasping forceps into the incision for grasping.
Repeated attacks of cholecystitis. Repeated attacks of cholecystitis make the gallbladder adhere to the surrounding tissues tightly, making it more difficult to distinguish anatomical relationships and isolate adherent tissues [10, 11]. When similar situations occur, the gallbladder triangle should be fully exposed. For example, when colon and duodenal adhesion are found during the operation, blunt dissection methods such as aspiration can be used for separation.
Our study also found that WBC > 10 × 109/l, maximum diameter of stones > 2 cm, and calculus incarcerated in the neck of the gallbladder were independent risk factors for DC. We consider the following:
Patients with elevated WBC often indicate that the gallbladder is with acute inflammation, which may lead to further congestion and oedema of the gallbladder wall and surrounding tissues, causing great difficulty in separating the gallbladder triangle and adding risk of injury of the extrahepatic bile duct [1, 12]. It is necessary to rationally apply antibiotics to control acute inflammation and apply surgery within 72 h. For patients beyond the window period, conservative treatment or percutaneous transhepatic drainage should be performed first, then LC should be applied after the inflammation is controlled.
Large gallstones may incarcerate in the neck of the gallbladder, which can shorten the gallbladder duct or make it disappear, adding risk of injury of the common bile duct [13]. To solve these problems, the incarcerated stones can be squeezed back into the gallbladder with separation forceps, or the stones can be removed before separation and ligation.
In order to further reflect the value of independent risk factors in evaluating the difficulty of cholecystectomy, we first evaluated the goodness-of-fit of the model, and then used ROC to evaluate its prediction [14, 15]. The results showed that the regression equation logit (P) had clinical value in predicting the difficulty of cholecystectomy.
Conclusions
The major risk factors of difficulty in cholecystectomy were BMI > 25 kg/m2, WBC > 10 × 109/l, frequency of acute cholecystitis in the last 2 months > 4 times, thickness of gallbladder wall > 0.5 cm, maximum stone diameter > 2 cm, and calculus incarceration in the neck of the gallbladder.
The application of this risk prediction model to predict the difficulty of cholecystectomy will help clinicians to carry out LC more safely and efficiently.