A 47-year-old man, smoker, was transferred to the Department of Cardiology Catheterization Laboratory at the National Heart Foundation (NHF) Hospital & Research Institute [1] in Dhaka, Bangladesh, from a remote hospital after streptokinase failure to reperfuse anterior ST-elevation acute myocardial infarction (STEMI).
The patient had presented in a local hospital with a severe retrosternal pain of 6-hour duration (transportation > 2 h). A diagnosis of anterior STEMI was made. The patient received i.v. morphine (8 mg) and intravenous streptokinase (STK, 1.5 million units i.v.) as the first-line reperfusion therapy in most areas of Bangladesh. Other medications were oral aspirin (300 mg), loading dose of generic clopidogrel (300 mg), and high-dose (80 mg) generic atorvastatin, all of which are now manufactured in the country.
Due to on-going severe chest pain in absence of any reperfusion signs (such as reperfusion arrhythmia or ST segment resolution), 2.5 h after STK administration, ground transportation to Dhaka was arranged for endovascular rescue. The patient arrived at the NHF cathlab 16 h from the chest pain onset, during the annual NHF Hospital & Research Institute Interventional Cardiology Conference. Admission ECG showed persistent ST segment elevation in the anterior leads; echocardiography demonstrated left ventricular (LV) anterior wall akinesia with normal muscle thickness and hypercontractility of the inferior segments (overall LV ejection fraction of 35%) in absence of any significant valvular or other pathology. The patient consented to be treated as a live case transmitted to the main auditorium, with interactions from the panel and participants (physicians, cathlab nurses, and cardiac technicians).
Coronary angiography showed a proximal left anterior descending (LAD) coronary artery occlusion (Figure 1 A). Unfractionated heparin was used for peri-procedural anticoagulation. After vessel wiring, thrombus aspiration was performed using Export 6F (Medtronic) aspiration catheter (Figure 1 B, arrow, effectively removed red and white thrombi in the basket, inset). For educational purposes it was interactively discussed that technically suboptimal coronary thrombectomy, including incomplete/non-axial guiding catheter engagement, may cause, through a “drag-and-drop” effect, coronary and cerebral embolism and stroke [2, 3]. However, it is methodologically incorrect to assign to thrombectomy strokes occurring 48 h to 6 months after thrombectomy-assissted primary percutaneous coronary intervention (PCI) (note 37 late strokes in the thrombectomy arm vs. 23 late strokes in the PCI alone arm of, respectively, 5033 and 5030 patients in the TOTAL study [4]) making the study conclusion essentially flawed (for the TASTE study fundamental design flaw, including enrollment limited to patients who would not require or benefit from thrombectomy in the operator’s opinion [5]). Because thrombus embolism aggravates myocardial injury [2, 3, 6, 7], aspiration thrombectomy should remain an essential consideration in primary angioplasty in acute myocardial infarction [5, 7–9], similar to the fundamental role played by thrombectomy in acute ischemic stroke interventions [10]. This should be paired with optimal stent use to achieve best outcomes in vessel lumen reconstruction and long-term clinical outcomes.
Figure 1
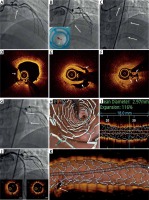
Angiography and optical coherence tomography imaging in a novel thin-strut bioresorbable-polymer sirolimus-eluting stent use in thrombus aspiration-assisted coronary angioplasty in acute myocardial infarction. A – proximal left anterior descending (LAD) occlusion (arrow). B – thrombus aspiration (second run, note contrast stagnation) using Export 6F (Medtronic) aspiration catheter (arrow); note white and red thrombi removed from the infarct-related artery, as shown in the aspiration system’s basket (B, inset). C – OCT run (Ilumien Optis Imaging System, Abbott) visualized residual red thrombus (D), ruptured plaque (E), and white thrombus (F). A novel thin-strut bioresorbable-polymer sirolimus-eluting stent (G, Alex Plus 3.0 × 18 mm, Balton, Poland, arrows) was implanted directly with a single inflation at 10–12 atm (30 s) with an optimal angiographic result and lack of any distal embolism (J). OCT demonstrated an optimal reconstruction of the lumen in absence of any dissection and in absence of any in-stent thrombotic or plaque material (“fly-through” image in H, the achieved vessel/stent diameter and stent expansion parameters in I, apposition in J (insets)) whereas 3D reconstruction (K) demonstrated a fully preserved side-branch access – another important feature of the stent design
Thrombolysis in myocardial infarction residual thrombus grade [7] was 2 out of 5. After i.v. nitroglycerin administration, optical coherence tomography (OCT, Ilumien Optis Imaging System, Abbott) run was employed to understand [11] the residual thrombotic material and plaque (Figures 1 D–F). A novel thin-strut bioresorbable-polymer sirolimus-eluting stent (Alex Plus 3.0 × 18 mm, Balton, Poland) [12–15] was implanted (direct stenting, 10–12 atm/30 s). Control angiography (Figure 1 J) showed lack of any residual stenosis and lack of distal embolism; there was TIMI-3 (TIMI Myocardial Perfusion Grade 2/3) [3]. OCT demonstrated an optimal reconstruction of the lumen in absence of any dissection and in absence of any in-stent thrombotic or plaque material (Figures 1 H–J), and it showed fully preserved side-branch access (Figure 1 K). Indeed, this stent has overall similar acute procedural results compared to other best-in-class stents [12–15], while optimal healing [16] and clinical outcomes of the device in all types of PCI including primary PCI in STEMI [13], are consistent with Alex Plus use as a modern workforce stent [14, 15]. Alex Plus is a Cobalt-Chromium new generation coronary stent with an innovative coating for a consistent and controlled drug delivery. Bioresorbable polymer layers release sirolimus in a time-controlled process of slow biodegradation (lasting ≈ 8 weeks), with optimal healing paired with an effective inhibition of neointima formation [16]. Favorable stent healing coverage occurs already at 1 month [16]. In addition, this stent type may have advantages in some specific indications such as the treatment of in-stent-restenosis [12].
Three days later the patient was discharged home in a good clinical condition. Prior to discharge, he received lifestyle modification education (inclusive of tobacco cessation patient-tailored personal plan) that is an important part of the NHF mission. NHF was founded in Bangladesh in 1978 at the initiative of National Professor Brig. (Rtd.) Abdul Malik to (i) promote cardiovascular health, educate and motivate people for prevention of cardiovascular diseases, (ii) provide in-hospital and out-patient services to patients suffering from cardiovascular diseases and associated conditions, (iii) train cardiovascular doctors, nurses, technicians and paramedics, and (iv) undertake and promote local high-quality research in cardiovascular diseases [1, 17]. NHF is a member of the World Heart Federation and it plays a very active role in the Stent-For-Life [18] initiative in Bangladesh, fostering progress in cardiovascular prevention, medical staff and patient education, and introducing novel cardiovascular therapies in the country. Systematic NHF endeavors to improve the STEMI patients access to guideline-indicated therapy, including access to affordable state-of-the-art biodegradable-polymer thin-strut stent technology taken together with the routine operator training in a leading institution in the country, offer an important benefit to the individuals with cardiovascular disease and to the society in a fast-developing country.







