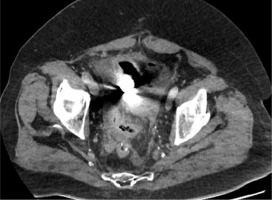
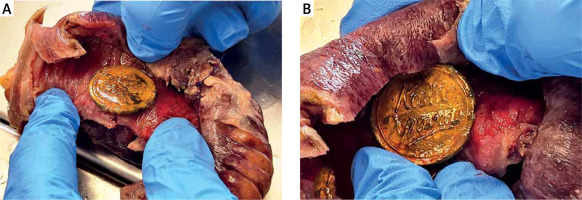
A 73-year-old male patient presented to the emergency department with diffuse severe abdominal pain persisting for 2 days. Upon clinical examination, the patient exhibited diffuse abdominal tenderness with signs of resistance and spasm, particularly in the left lower quadrant. Patient had undergone surgery for left colectomy due to colorectal cancer and subsequently received adjuvant chemotherapy, remaining disease-free to date. Additionally, the patient had a history of an inguinal hernia on the right side. The patient was haemodynamically unstable and oliguric at admission, necessitating vasoconstrictors. The patient’s vital signs revealed a blood pressure of 83/59 mm Hg and a pulse rate of 127 bpm. His blood pressure stabilized prior to computed tomography (CT) by receiving continuous IV fluid infusion. An abdominal CT scan revealed free intraperitoneal air and a foreign body within the gastrointestinal tract (Figure 1). Subsequently, the patient was taken to the operating room for exploratory laparotomy. Intraoperatively, faecal peritonitis and perforation of a segment of the terminal ileum were identified. A partial segmentectomy with simultaneous anastomosis was performed. During the resection of the surgical specimen, a medal trinket was discovered, originating from a New Year’s Eve cake (Figures 2 A, B). Following surgery, the patient was transferred to the intensive care unit, intubated, and mechanically ventilated. He remained hospitalized in the ICU for 8 days with no major postoperative complications. After a 21-day stay the patient was discharged. Despite the relatively common occurrence of ingesting foreign objects, most cases result in the object passing harmlessly through the alimentary tract without complications. Less than 1% of ingested foreign bodies lead to bowel perforation, which underscores the rarity of this outcome [1, 2]. While injuries resulting from ingested foreign bodies can manifest at various points along the digestive tract, the most common sites for perforation are found in the ileal, ileocaecal, and rectosigmoid regions [2–7]. Hence, a thorough understanding of the risks associated with ingested foreign bodies and their potential impact on the digestive system is crucial for both medical professionals and the general public, because it can aid in early recognition and prompt intervention when such cases arise [4, 5]. Foreign bodies that seem to be dangerous because of their shape and size should be effectively removed. There are many options available, including endoscopy, laparoscopy, and laparo-endoscopic removal of foreign bodies. The procedure of choice is endoscopic removal, which is fruitful in the majority of patients [8–10]. In conclusion, the perforation of intestinal structures due to ingested foreign bodies presents a complex and often challenging diagnostic scenario, especially in cases of acute abdominal symptoms, in which the underlying cause may not be immediately apparent. Abdominal CT scans can effectively identify instances of small bowel perforation and may provide valuable indications of the underlying cause [10]. Sometimes the laparoscopic approach before open surgery can be performed safely for the removal of a foreign body. Minimally invasive laparoscopic surgery should be preferred to open surgery due to its advantages [11, 12].
1/2024
vol. 19
List do Redakcji
A case report of a forgotten Christmas gift
- Department of Surgery, General University Hospital of Patras, Patras, Greece
- First Department of Surgery, National and Kapodistrian University of Athens, Laikon General Hospital, Athens, Greece
- Third Department of Surgery, Evangelismos General Hospital, Athens, Greece
Gastroenterology Rev 2024; 19 (1): 99–100
Data publikacji online: 2024/03/13
Plik artykułu
References
Jaan A, Mulita F. Gastrointestinal Foreign Body. [Updated 2023 Aug 28]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2023 Jan. Available from: https://www.ncbi.nlm.nih.gov/books/NBK562203/
Copyright: © 2024 Termedia Sp. z o. o. This is an Open Access article distributed under the terms of the Creative Commons Attribution-NonCommercial-ShareAlike 4.0 International (CC BY-NC-SA 4.0) License (http://creativecommons.org/licenses/by-nc-sa/4.0/), allowing third parties to copy and redistribute the material in any medium or format and to remix, transform, and build upon the material, provided the original work is properly cited and states its license.