Purpose
For early breast cancer patients undergoing breast conservation therapy, accelerated partial breast irradiation (APBI) offers the advantage of shorter overall treatment time for appropriately selected patients [1, 2]. It is an acceptable alternative to external whole breast radiotherapy (WBRT), with reduced toxicity and improved cosmetic outcomes [3, 4]. Out of various techniques available to deliver APBI, multi-channel nylon catheter-based interstitial brachytherapy is the most established technique [5]. Many studies published physician-reported and patient-reported cosmetic outcomes with APBI in comparison with WBRT [6, 7]. Comparison of patients’ quality of life (QOL) is an integral part of outcomes reporting while evaluating different treatment modalities. Various Western retrospective and prospective randomized studies have shown similar cosmesis and QOL outcomes with APBI and WBRT [8-10]. In the absence of randomized data from Indian population, matching APBI and WBRT patients’ cohorts for important factors could improve the quality of comparison of QOL scores. These factors consist of treatment aspects, such as type of primary breast surgery, type of endocrine therapy, receipt of adjuvant chemotherapy, tumor factors, like tumor and nodal stage, and patient factors, including age and menopausal status [11, 12]. Therefore, this study employed a propensity-score matched pair analysis for comparing short-term patient-reported QOL scores after APBI and WBRT in a prospective manner.
Material and methods
This was a prospective observational cross-sectional study, approved by the institutional review board.
Patients’ selection
Women with breast cancer, who had undergone breast-conserving surgery followed by adjuvant radiotherapy, and attending every 6 months follow-up visits at our institute were screened for this study. These patients who were within a follow-up period of 18 to 36 months post-radiotherapy were enrolled in the present study, after obtaining a written informed consent. Patients with mastectomy, bilateral breast cancer, or reconstructive procedures were excluded from the research. Breast-conserving surgery comprised of lumpectomy, with a 1-2 cm clearance for all cases. For all the patients without clinical evidence of nodal involvement, axillary sampling was done, and lymph node negative status was confirmed on frozen section intra-operatively. For patients with clinically positive nodal disease and those with positive nodes on axillary sampling, complete axillary dissection was performed for level I-III axillary nodes.
Treatment details
For patients undergoing WBRT, radiotherapy was started either four to six weeks after surgery (for patients not planned for adjuvant chemotherapy), or two to four weeks after completion of adjuvant chemotherapy. Every patient underwent computerized tomography (CT)-based radiotherapy planning. WBRT was delivered with megavoltage photons using 3-dimensional conformal technique (3D-CRT). Hypofractionated dose schedule of 40 Gy in 15 fractions daily to the entire breast was used, with five fractions a week. This was followed by sequential boost to the tumor bed to a dose of 12.5 Gy in five daily fractions over one week using enface electrons. Ipsilateral supraclavicular region was also treated to 40 Gy in 15 fractions for patients who had pathologically node-positive disease or T3/T4 stage of the disease. No patient received axillary radiotherapy or prophylactic internal mammary irradiation.
APBI was performed with multi-catheter interstitial brachytherapy technique using flexible nylon catheters, either intra-operatively or post-operatively after breast-conserving surgery by open cavity technique. Patients’ selection criteria, procedure of implant, and dosimetric considerations have been described in detail previously [13]. A dose of 34 Gy in 10 fractions or 32 Gy in 8 fractions was prescribed to clinical target volume (CTV), applied twice daily, at least 6 hours apart. APBI began on the third day after intra-operative implant or on the same day as the post-operative implant. If chemotherapy was planned, a gap of two to three weeks was provided between APBI and chemotherapy. For hormone receptor-positive disease, appropriate endocrine therapy was advised as per institutional protocol to all patients.
QOL assessment
After patient’s consent to participate in the study, a single cross-sectional QOL assessment was completed. EORTC QLQ-C30 and BR-23 questionnaires (English and validated translations in Hindi and Marathi) were used for the QOL assessment. QLQ-C30 assesses six function scales (physical, role, emotional, cognitive, social, and global health status) and eight symptom scales (fatigue, nausea/vomiting, pain, dyspnea, insomnia, appetite loss, constipation, diarrhea, and financial difficulties). Breast specific module QLQ-BR23 evaluates four symptom scales (systemic therapy side effects, breast symptoms, arm symptoms, and upset by hair loss) and four functional scales (body image, sexual functioning, sexual enjoyment, and future perspective).
Statistical analysis
Patients treated with APBI were propensity-score matched to a similar cohort of WBRT using nearest neighborhood algorithm with calliper width of 0.2 for covariates known to effect body image significantly, as described previously [14]. These covariates included menopausal status, size of the surgical cavity (< 100 cc vs. > 100 cc), size of the tumor in greatest dimension (pathological tumor size < 2 cm vs. ≥ 2 cm), number of lymph nodes dissected, treatment with any chemotherapy (neoadjuvant or adjuvant), and treatment with hormonal therapy. QOL scores for all the items and scales were linearly transformed to 0-100 points scale, according to the EORTC QOL scoring manual. Mean scores for each domain were analyzed for the entire unmatched cohort as well as compared between the two matched cohorts using Student’s two-tailed t-test. A p-value of < 0.05 was considered statistically significant, and a 10-point difference between the mean scores was considered as clinically significant. Mean QOL scores were also compared with EORTC reference values for QOL scores in stage I-II breast cancer, and with mean QOL scores at 3-years follow-up from the GEC-ESTRO randomized trial of APBI vs. WBRT [10]. All statistical analyses were performed using SPSS version 21.0 (IBM Corp.).
Results
A total of 320 consecutive eligible patients on a follow-up were enrolled into the study from January 2017 to June 2018. Table 1 shows baseline characteristics for these patients.
Table 1
Patients’ characteristics
The patients had received adjuvant RT from January 2015 to November 2016. QOL scores from a single assessment during the time period of 18-36 months after radiotherapy were reported in the present study. The quality-of-life data was collected during the patients’ follow-up visits. Of the total 320 patients, 80 were treated with APBI and 240 with WBRT. In the APBI group, 82% patients received brachytherapy dose of 34 Gy in 10 fractions, while 18% received 32 Gy in 8 fractions. In the WBRT cohort, almost all of the patients (n = 228, 95%) were treated with conventional or 3D-CRT technique using bitangential portals. The most common dose prescription for WBRT was 40 Gy in 15 fractions over three weeks (n = 207) to the entire breast. Sequential tumor bed boost of 12.5 Gy in 5 fractions over one week was delivered using electrons. Median cavity size was 99 cc and 118.1 cc in the APBI and WBRT cohorts, respectively, as measured in simulation CT images at the time of radiotherapy planning. Any aspiration procedure, if recommended, was performed prior to the simulation CT. Median follow-up was 26 months and 24 months for the APBI and WBRT cohorts, respectively.
Using the propensity-score matching, a total of 64 APBI patients were matched with 99 WBRT patients out of the entire study cohort of 320 cases. Details of propensity-score matching have been reported along with analysis of cosmetic outcomes previously [14]. Mean QOL scores for the matched cohorts of WBRT and APBI are shown in Table 2, and scores for the unmatched cohorts are presented in Appendix 1. Statistically significant difference was observed for QOL scores in the role function, cognitive function, pain, appetite loss, and hair loss sub-scales between the matched WBRT and APBI groups. However, none of the differences in these domains of QLQ-C30 and BR-23 reached clinically significant difference of 10 points, except for the hair loss. There was a small difference of 5-10 points favoring WBRT for the role function (97.0 vs. 91.4, p = 0.015), pain (8.2 vs. 16.1, p = 0.017), and appetite loss (3.7 vs. 10.9, p = 0.015) domains. Only a quarter of the patients in the matched cohort (40 of 163; WBRT = 22, APBI = 18) responded to the question of ‘upset by hair loss’, of which nine reported significant bother (‘quite a bit’/‘very much’). Mean score for the ‘upset by hair loss’ sub-scale was significantly higher in the APBI group (51.9 vs. 22.7, p = 0.006). However, hair loss is primarily an adverse effect attributable to chemotherapy, and here, out of the quarter of patients reporting any hair loss, 23% did not receive any chemotherapy. No other factor accounting for hair loss could be identified.
Table 2
Mean quality of life (QOL) scores for matched cohorts
Discussion
Interstitial brachytherapy is an invasive procedure, and differences in some QOL domains as compared to WBRT can be expected in the first year of follow-up after radiotherapy, as the catheter marks fade and tumor bed heals. Certainly, a few longitudinal studies on APBI assessing change in patients’ QOL over time suggested that scores tend to improve over first two years after completion of treatment [8, 15]. Our study included patients who were 18 to 36 months post-radiotherapy, and by this time, the acute and sub-acute toxicities subsided; therefore, QOL could be expected to stabilize. This might explain the absence of clinically relevant differences in scores of all the QOL domains (i.e., < 10-point difference), despite a few of them reaching statistical significance.
If patient’s characteristics were considered for unmatched WBRT and APBI groups, the patients were selected for APBI based on strict recommendations by global professional societies [2, 16], which include post-menopausal women with T1-T2 stage, node-negative breast cancer. Large majority of women not fulfilling these criteria are treated with WBRT, along with more extensive surgery and/or more intensive chemotherapy, depending on the tumor stage. Propensity-score matching between APBI and WBRT groups negates the confounding influence of these factors related to patients’ selection, tumor stage, and treatment toxicity upon the QOL scores. Moreover, it improves the quality of comparison, even though it reduces the number of observations in order to balance the data. The covariates used for propensity-score matching are the ones shown to significantly influence the body image.
The threshold for clinically meaningful difference used in this study was based on the results of QOL studies from many cancer sites including breast cancer, and estimating a 5-10 points change in QOL score as ‘small’ or ‘trivial’, 10-20 points change as ‘moderate’, and > 20 points change as ‘large’ [17-19]. Alternatively, a threshold of half the standard deviation (SD = 0.5) can be used to determine clinically relevant change [20]. Although the former interpretation of small/moderate/large difference could be simplistic, it is more practical, easier to interpret and compare, and therefore preferred for integrating QOL end points in large clinical trials [10, 21]. The present study demonstrates statistically significant differences in scores for the role and cognitive function, pain, appetite loss, and hair loss, but none, except hair loss, reached the 10-point threshold of clinical significance. The difference in ‘upset by hair loss’ domain was not attributable to either of the two radiotherapy modalities, occurring most likely due to small number of respondents.
To put our results in context of early breast cancer patients globally, the mean QOL scores observed in the matched pair cohorts of WBRT and APBI in the present study were compared to the EORTC reference mean QOL scores for stage I-II breast cancer patients, and with the mean QOL scores at 3-years follow-up from the GEC-ESTRO randomized trial of APBI vs. WBRT [10] (Figures 1 and 2). EORTC reference values are available for QLQ-C30 but not for the BR-23 module. Overall, QOL scores in present study were similar or slightly better than the GEC-ESTRO and EORTC reference cohorts, with generally higher function scores and lower symptom scores, except in sexual functioning and sexual enjoyment domains. To note, only 17.6% patients in our study (WBRT = 15, APBI = 9) reported being sexually active. A comparison of patients’ characteristics between the GEC-ESTRO cohort and our institutional APBI group was previously reported [13], and revealed that the pathological tumor size tended to be larger and the proportion of estrogen receptor (ER) positive tumors was lower in our patients. These differences also contributed to an increased use of chemotherapy in our patients’ cohort. Nonetheless, clinical outcomes were satisfactory, with 7-year disease-free survival of 97.5% and overall survival of 89%. High level of patient satisfaction with APBI, as observed previously [14], and similar QOL scores in the present study should encourage further uptake of APBI for suitably selected patients with early breast cancer in India. Additionally, it was impossible to embark randomized evidence in Indian setting, especially using brachytherapy because of the lack of availability of the expertise for breast brachytherapy across the country.
Fig. 1
Comparison of QLQ-C30 mean quality of life (QOL) scores from the propensity score-matched whole breast radiotherapy (WBRT) and accelerated partial breast irradiation (APBI) cohorts of the present study, with the mean QOL scores at 3 years follow-up in the GEC-ESTRO randomized trial of APBI vs. WBRT, and with the EORTC reference mean QLQ-C30 scores for stage I-II breast cancer
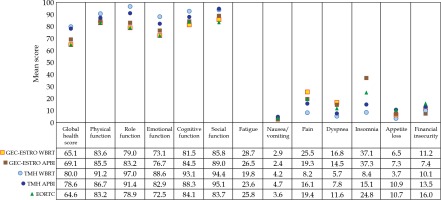
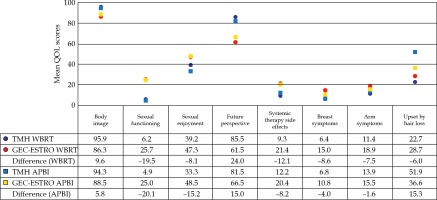
Fig. 2
Comparison of BR-23 mean quality of life (QOL) scores from the propensity score-matched whole breast radiotherapy (WBRT) and accelerated partial breast irradiation (APBI) cohorts of the present study, with the mean QOL scores at 3 years follow-up in the GEC-ESTRO randomized trial of APBI vs. WBRT
Clinical efficacy of APBI has been proven in comparison to WBRT, with high rates of patients’ satisfaction and cosmesis [6, 7, 13, 22]. Also, patient-reported QOL has been observed to be similar or better than WBRT in randomized trials as well as prospective studies [9, 10, 15, 23]. In addition to multi-catheter interstitial brachytherapy, QOL has also been assessed in patients treated with other APBI techniques. In a study comparing QOL between intensity modulated radiation therapy (IMRT)-based APBI to WBRT, QOL scores up to two years post-radiotherapy were better with APBI [23]. Another study showed better QOL scores with APBI using single-lumen and multi-lumen brachytherapy as compared to WBRT [8]. The results from our study are in concordance with the global experience, and confirm good QOL outcomes in Indian patients treated with APBI for localized early breast cancer.
There are some drawbacks to be acknowledged in this study. A single cross-sectional QOL assessment in 18-36 months follow-up period to assess long-term patients’ QOL outcomes is simple and practical, but less desirable than longitudinal assessment at multiple time points. The longitudinal assessment of late toxicity and QOL has been initiated as a part of separate prospective study on recently treated patients, and will be published as soon as the data matures. Patients’ selection for APBI was based on strict recommendations of global professional societies, which include stage T1-T2 post-menopausal women with node-negative breast cancer [2, 24]. Patients not meeting these criteria were treated with WBRT, along with more extensive surgery and/or more intensive chemotherapy, depending on the tumor stage. Propensity-score matching between APBI and WBRT groups minimizes the confounding effect of various tumor and treatment factors upon the QOL scores, and improves the quality of comparison. However, the influence of selection bias and unknown confounding variables cannot be completely eliminated. Unlike in Western countries, where screen-detected breast cancer is common and suitable for brachytherapy, early breast cancer patients treated with APBI have larger tumors and higher grade. Regardless of the above, excellent outcomes have been reported for APBI from our institute [25]. Therefore, indirect comparison has been performed with due acknowledgement of various known/unknown biases.
The relevance of small but statistically significant difference in QOL sub-scales between APBI and WBRT can be debated depending on the definition of clinically meaningful difference. Whether such small differences can influence treatment decisions, when considering overall treatment time, resources, and costs associated with APBI, this is something for every radiation oncologist to consider in their own clinical practice.
Conclusions
Patients with breast cancer undergoing breast-conserving surgery and adjuvant radiotherapy report high QOL scores. The modality of adjuvant radiation (APBI or WBRT) did not have a clinically significant difference in the QOL of patients. Hence, this study supports the use of APBI and higher adoption of this modality in the breast cancer radiotherapy practices in India.










