INTRODUCTION
Multiple sclerosis (MS) is a disorder that damages the central nervous system chronically and progressively [1]. The results of epidemiological studies in Iran indicate that the prevalence and incidence of MS in Iran are increasing, and people in 21 of the 31 provinces in Iran are at high risk of developing MS. Also, in two recent studies the prevalence of MS in Guilan province was reported to be 33 [2] and 36 [3] per 100,000 people in an ascending trend. MS has neurological, cognitive, emotional, and behavioral manifestations [4]. As this disease is progressive and chronic it causes early disability in individuals, which, if not treated promptly, impairs their quality of life [5]. Furthermore, stressful life events cause MS symptoms and exacerbations of them, primarily mediated by immune function and autonomic imbalance [6]. Moreover, the periventricular region, frontal lobes [7], temporal lobes [8] and right temporal regions [9] are involved in people with MS (PwMS). The fact that MS affects neurotransmitter systems and structures (like the amygdala, basal ganglia, and cerebral cortex [10]) involved in the processing and perception of emotions [11] supports the notion that symptoms of anxiety and depression, as well as the decline in psychological well-being observed among PwMS, have a biological etiology [12]. Accordingly, the results of previous studies show that PwMS in Guilan province suffer from a variety of psychological disorders compared to their healthy counterparts [13, 14]. Given all this evidence, a concentration on factors determining the psychological well-being in PwMS can be very consequential [15].
Studies note that self-compassion is a psychological factor affecting well-being [16]. Self-compassion is defined as a desire to improve health and well-being, complemented by a personal initiative to effect necessary life changes. The self-compassionate person has to face and experience his suffering without avoiding effort. Within this context, one interprets suffering and imperfection as part of the experience of life and does not blame oneself for suffering, imperfection, and an unpleasant condition [16]. MS has a variety of disabilities and forms of suffering for people with the disease that can play an instrumental role in reducing the quality of life and increasing psychological injury [17]. Self-compassion can be considered an essential source of coping in the lives of these patients and can facilitate their acceptance of suffering and disability [18]. Therefore, given the background, it is quite clear that self-compassion plays a notable role in increasing coping skills and the adaptation of PwMS to the condition. However, little is known about the function self-compassion and the role of resilience as a potential mediating mechanism in these patients.
SELF-COMPASSION AND RESILIENCE IN PEOPLE WITH MULTIPLE SCLEROSIS
Resilience is defined as a potent process of positive adaptation to misfortune [19]; it implies that, despite all the difficulties and sufferings that exist, one can successfully deal with a situation [20]. Individuals with MS who are more resilient are more likely to adapt to their disease by making fundamental changes in their lives [21]. Other studies have stated that self-compassion has a positive relationship with resilience [22-24]. However, a study has been conducted specifically in PwMS that supports self-compassion as a vital factor which is correlated with resilience [18]. From all previous studies, it is concluded that resilience is an appropriate source of protection for PwMS. Moreover, studies have shown that self-compassion can play a crucial role in the resilience level of people [25]; however, no study exploring the association between self-compassion and resilience – and also the mediating role of resilience among PwMS in non-Western countries – has been found.
RESILIENCE AND PSYCHOLOGICAL WELL-BEING IN PEOPLE WITH MULTIPLE SCLEROSIS
Resilience is another feature affiliated with psychological well-being [26]. Many studies support the effect of resilience on psychological well-being [27-29]. Since MS commonly occurs in young adults between the ages of 20 and 40, it may affect personal growth in numerous areas that are extremely important to young people at this age [30]. The review of studies suggests that individuals’ potential reactions may be affected by different levels of resilience. In other words, people who are more resilient report less psychological harm and enjoy greater psychological well-being [31]. Psychological well-being refers to living life in a complete and satisfying way and to the development and self-realization of the individual [32]. In other words, psychological well-being is a component of QoL that refers to the way individuals evaluate their lives [33], and provides a much fuller picture of an individual and their overall well-being [34]. It consists of cognitive and affective dimensions [33]. Resilience is a protective factor in PwMS [25] that counteracts the negative effects of stress and increases well-being [35]. From all previous studies, it is inferred that resilience is an effective source of coping for PwMS that can play an important role in the psychological well-being of these patients.
Currently, there is little research on the potential mediation of resilience in the relationship between self- compassion and psychological well-being, especially among PwMS. Therefore this study investigated the potential mediating effect of resilience on the relationship between these two variables. Doing such research by considering the mediating variable can be effective in improving treatment approaches [36]. This study aims to fill the research gap identified in investigating the mediating role of resilience in the relationship between self-compassion and psychological well-being in PwMS. The results of this study can be useful in reviewing rehabilitation and treatment programs.
METHODS
Study group and design
This cross-sectional study was conducted in Guilan province in Iran in 2021, exclusively on people who were registered with the Guilan MS Society (GMSS) and user support services. GMSS has registered 2,500 patients, of whom 410 PwMS participated in the study and took the online survey (created by Porsline). Sample size using the formula of Chow et al. [37] and the extracted findings (σ = 13.06; 1-a = 0.05; 1-β = 0.90; d = 2.1) from the pilot implementation of Ryff ’s Psychological Well-Being Scales (PWB) (criterion variable) was calculated in 410 PwMS in Guilan province.
Measures
Demographic questionnaire: The questionnaire contained information including age (year), disease duration (months), marital status, type of MS, and level of education.
Ryff ’s Psychological Well-Being Scales (PWB): This tool has 120, 84, 54, and 18 item versions [38]. The current study used the 18-item version, with six subscales of self-acceptance, autonomy, environmental mastery, purpose in life, positive relations with others, and personal growth. In addition, each of them is measured with three questions. The items are answered on the basis of a 6-point Likert scale, from 1 = “Completely disagree” to 6 = “Completely agree”. The range of scores on this scale is between 18 and 108, and higher scores indicate higher levels of psychological well-being. In Iranian students, the validity of this scale was investigated by confirmatory factor analysis, and its reliability was calculated with the internal consistency method. Cronbach’s α for subscales varied between 0.57 and 0.76. Cronbach’s α for the total scale was 0.71 [39]. In the present study, the internal consistency of 18 items was calculated to be 0.71 Cronbach’s α.
Connor-Davidson Resilience Scale (CD-RISC): This scale was designed by Connor and Davidson [40]. It has 25 questions and five subscales of personal competence, tolerance of negative effects and strengthening effects to stress, positive acceptance of change, self-control, and spiritual influences. Measures are based on the Likert scale of five degrees (“Not true at all” = 0 to “True nearly all the time” = 4). The range of scores in this questionnaire is between 0 and 100, and the higher a score is, the higher the degree of resilience it indicates [40]. In the Iranian sample, the validity of this questionnaire was confirmed by confirmatory factor analysis, and Cronbach’s α coefficients were between 0.70 and 0.80 for the subscales and 0.82 for the whole scale [41]. In the present study, internal consistency was calculated to be 0.78 Cronbach’s α for all questions.
Self-Compassion Scale Short Form (SCS-SF): In order to make the completion of the questionnaire quicker, the SCS-SF was designed [42]. This scale consists of 12 items and six subscales: self-judgment, self-kindness, isolation, common humanity, over-identification, and mindfulness, each of which is measured by two items. This scale is rated based on a 6-point Likert scale from 0 = “Almost never” to 5 = “Almost always”. The range of scores on this scale is between 0 and 60, and high scores indicate greater self-compassion [42]. This scale has high validity in Iranian students, and its six-factor structure has been confirmed. It was proved to have good internal consistency with Cronbach’s α, at 0.79 [43]. Cronbach’s α calculated for the current sample was 0.79.
Procedures
Participants joined this study between August and September 2021 using the convenience sampling method from the GMSS. Data collection started after gaining permission from the Research Ethics Committee of Guilan University of Medical Sciences (IR.GUMS.REC.1400.218). Membership in the GMSS with a registered mobile phone number and signing informed consent were the criteria for entering the study. The informed consent form, along with the research tools, was designed in the online survey system (Porsline), and then the link was sent via SMS to all participants. One week after sending the link to the survey form a follow-up SMS was sent to people who had not previously responded and would like to participate in the survey. Sampling ceased after the completion of 410 survey forms. The participants were aware of our goals and all the ethical principles of the Declaration of Helsinki were respected by researchers at all stages of the research. There was no financial incentive to participate in the study, and respondents took part in the survey voluntarily and anonymously. In addition, no physical or psychological harm was suffered by any of them.
IBM SPSS and Amos software version 24 were used for the data analysis. Descriptive data were analyzed with frequency, percentage, mean and standard deviation. The normal distribution of data was assessed based on skewness and kurtosis statistics. The Pearson correlation coefficient test was used to evaluate the correlation of SCS-SF with PWB and CD-RISC. After ensuring the content validity of the research questionnaire, to more accurately measure its validity the structure was also examined using structural equations modeling and confirmatory factor analysis. Unlike conventional statistical tests, which are confirmed or rejected by a statistic, structural equation modeling introduces some indices. In the present study, the chi-square, chi-squared significance level (p-value), root index of estimated error estimation (RMSEA), normal chi-squared (c2/DF), fit index normalized (NFI), incremental fit index (IFI), adaptive fit index (CFI), Tucker-Lewis index (TLI), and relative fit index (RFI) were used to investigate the fit of the structural equation model. MacCallum et al. suggest that < 0.08 values of the root index of the approximate error estimate indicate an acceptable fit between the hypothesized model and the observed data [44]. Moreover, Schumacher and Lumex accepted values of 1 to 5 for c2/DF [45]. This index represents a derivative of the normalized fit index, and like the adaptive and normalized fit indexes, values of the relative fit index range from zero to 1.00, and values close to 0.95 indicate a good fit [46]. The incremental fit index is the same as the normalized fit index, except that the degrees of freedom are calculated [47]. Finally, the Tucker-Lewis index ranges from zero to 1.00, with values near 0.95 indicating an acceptable fit for large samples [46]. Bootstrapping was used to investigate the mediating role of CD-RISC between SCS-SF and PWB and to find the direct effects of variables.
Data analysis plan
In order to examine the conceptual model of the study, the maximum likelihood method was applied with the Amos software. Before verifying hypotheses and examining the relationships among the research variables, we checked whether there were significant differences between men and women and between age groups in the levels of the variables studied. The independent t-test did not show significant differences between men and women in the level of self-compassion (t(408) = –0.256, p = 0.777), psychological well-being (t(408) = 0.162, p = 0. 871) or resilience (t(408) = 0.203, p = 0.839). A one-way analysis of variance (ANOVA) did not show significant differences between age groups in the level of self-compassion (F(2, 407) = 1.184, p = 0.307), psychological well-being (F(2, 407) = 1.181, p = 0.308) or resilience (F(2, 407) = 1.272, p = 0.281). Since no significant difference was found between men and women and between age groups, there was no need to control for demographic variables in the analyses. Finally, the adequacy and fit of the models were assessed. The results of the model fit evaluation have shown that CFI, NFI, IFI, and TLI are all between 0.90 and 1. In addition, RFI was obtained greater than 0.60, approximate error (RMSEA) was less than 0.08, and the normal χ2 (χ2/DF) was less than 5. Hence, on the basis of these results all three structures have a good fit.
RESULTS
As noted, in this study, 410 PwMS participated in an online survey. Their demographic findings are presented in Table 1.
Table 1
Demographic information of the participants
Participants were 37.07 ± 8.09 years old (M ± SD). The M ± SD disease duration was 66.63 ± 76.56 months. Most participants were female (n = 310; 75.6%) and married (n = 235; 57.3%), with RRMS type (n = 280; 68.3%) and with associate’s or bachelor’s degrees (n = 170; 41.5%).
Table 2 presents the descriptive findings of the variables, skewness and kurtosis indices, and Pearson correlation coefficients between them.
Table 2
Descriptive statistics and correlation between study variables (n = 410)
| Variables | M | SD | Skewness | Kurtosis | 1 | 2 | 3 |
|---|---|---|---|---|---|---|---|
| 1. PWB | 75.46 | 13.86 | –0.22 | –0.06 | – | ||
| 2. SCS-SF | 35.78 | 8.62 | 0.16 | –0.29 | 0.65** | – | |
| 3. CD-RISC | 58.73 | 19.00 | –0.24 | –0.21 | 0.78** | 0.66** | – |
As shown in Table 2, the skewness and kurtosis indices for all three variables are within the range of +2 to –2, which indicates a normal distribution. The results also indicated that psychological well-being has a positive and significant correlation with self-compassion (r = 0.65; p = 0.001) and resilience (r = 0.78; p = 0.001). Also, there was a positive and significant correlation between psychological resilience and self-compassion (r = 0.66; p = 0.001).
The p-value alone is not a valid criterion for assessing model fit; therefore, other indices are used to assess scale fit. The goodness-of-fit results in terms of the structure of self-compassion show that RMSEA, c2/DF, NFI, IFI, CFI, TLI, and RFI are 0.053, 2.164, 0.931, 0.962, 0.961, 0.941, and 0.896, respectively. As reflected in the goodness of fit results, RMSEA, c2/DF, NFI, IFI, CFI, TLI, and RFI were each 0.036, 1.535, 0.917, 0.996, 0.996, 0.961, and 0.896, respectively. In addition, the goodness-of-fit results related to resilience structure showed that RMSEA, c2/DF, NFI, IFI, CFI, TLI and RFI were 0.047, 1.900, 0.902, 0.951, 0.951, 0.944 and 0.888, respectively (Table 3). As shown in Table 3, the results of the goodness-of-fit of the research model show that IFI, NFI, CFI, and TLI are greater than 0.90 and close to 1. Also, RFI is greater than 0.60; approximate error (RMSEA) is less than 0.08, and normal c2 (c2/DF) is less than 5. The IFI, NFI, CFI, and TLI indices range from zero to one, and the closer they are to one, the better the model fit. When the RFI is greater than 0.60, the approximation error (RMSEA) is less than 0.08, and the normal c2 (c2/DF) is less than 5, the model fit is also good. Based on these results, it can be concluded that all three structures have a suitable fit. In addition, the construct validity of all three structures is confirmed by the data obtained.
Table 3
Fit indicators of the proposed model c2
| Model | χ2 | df | p-value | χ2/df | NFI | IFI | CFI | TLI | RFI | RMSEA |
|---|---|---|---|---|---|---|---|---|---|---|
| Proposed | 131.228 | 50 | 0.000 | 2.626 | 0.958 | 0.974 | 0.974 | 0.965 | 0.945 | 0.063 |
| Level fitting | – | – | – | 1-5 | > 90 | > 90 | > 90 | > 90 | > 60 | < 0.08 |
Bootstrapping was used to investigate the direct and indirect effects of variables within the proposed model, resulting in the data presented in Table 4.
Table 4
Estimate of the direct and indirect effects
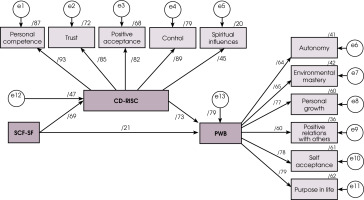
As can be seen in Table 4, the results of the significance test of the path coefficients show that all direct path coefficients are significant (t ≥ 1.96). The results of the coefficients of the direct effects of the variables on each other show that self-compassion is related to resilience and psychological well-being. A direct effect of self-compassion on psychological well-being was detected (β = 0.21, 95% CI: 0.12-0.30). Moreover, a direct effect of self-compassion on resilience was also obtained (β = 0.69, 95% CI: 0.62-0.74). There was a significant direct effect of resilience on psychological well-being (β = 0.73, 95% CI: 0.63-0.81). In addition, the study’s indirect effect results suggest a significant indirect effect of self-compassion on psychological well-being, with resilience playing a mediating role (Figure I). In other words, in addition to confirming the direct relationships between the variables studied, the mediating role of resilience in the relationship between self-compassion and psychological well-being was also confirmed (p ≤ 0.05).
DISCUSSION
Positive psychology is a scientific endeavor to improve well-being, so that individuals can have meaningful lives [48]. In this regard, the present study was conducted to investigate the mediating effects of resilience on the relationship between self-compassion and psychological well- being in PwMS in Iran. The main conclusion of this study was that resilience significantly mediates the relationship between self-compassion and psychological well-being.
Our results are consistent with previous studies that have shown that high self-compassion is associated with higher levels of resilience [22]. Additionally, previous studies have shown that higher levels of resilience lead to greater psychological well-being [27-29], and that higher levels of resilience contribute to better adaptation to disease [21]. Previous studies have also shown that a high level of resilience is associated with a reduction in psychological symptoms (e.g., anxiety, stress, and depression) [31, 49]. Finally, the research literature supports the mediating role of resilience in the relationship between self-compassion and quality of life in PwMS [18] and the mediating role of resilience in the relationship between self-compassion and psychological well-being in counselors [24]. As well as the congruence of our results with previous studies, this study takes things a step further by confirming that resilience plays a significant role in the relationship between self-compassion and psychological well-being in PwMS in Iran.
Overall, our findings suggest that self-compassion and resilience may lead to improvement of psychological well-being by increasing adaptability to unexpected conditions. Self-compassion is a crucial coping strategy that can enhance people’s psychological well-being [50]. Because this approach helps them be kind to themselves, more aware of their living conditions, and face problems without negative judgment [16], we can expect that individuals with multiple sclerosis who have high self-compassion may be more resilient in the face of illness and suffering. As a result, resilience helps the individual move beyond unpleasant events and return to the desired state by developing positive emotions [51]. In addition, resilience can lessen the effects of stress and improve health and well-being by increasing acceptance [52]. A theoretical view supports the mediation of resilience, and it is believed that it is a source of protection against stress [53]. A medical perspective states that decreased negative emotions and increased self-compassion are linked to increased levels of oxytocin in the brain, which in turn reduces amygdala activity [54]. A person with MS with a high level of self-compassion has greater psychological well-being than one with a low level of self-compassion [55]. Self-compassion and resilience are potential protective capacities for PwMS in Iran, and play a crucial role in their psychological well-being.
Despite providing evidence of the resilience-mediated relationship between self-compassion and psychological well-being in PwMS in Iran and filling a research gap in this area, our study has limitations. The first limitation: the study was conducted in Gilan province, whereas Tehran and Isfahan are classified as higher-risk areas for this disease [56]. Future studies could lead to extensive sampling nationally, especially in high-risk areas, to increase the generalizability of results. The second limitation: the sampling unit in this study was patients who were registered in the GMSS and had a mobile phone number to send the link to the questionnaires to. However, some patients decline to join the association for some reason. Thus, it is suggested that future researchers do their sampling from the medical centers. The third limitation: this research was conducted within the framework of a correlation design, based on which causality cannot be achieved. Therefore, we recommended that future researchers conduct experimental and longitudinal research to reach a causal relationship. The fourth limitation: in this study, we used self-reported questionnaires that can be answered with a bias of social desirability and lucky answers. A better understanding of resilience and self-compassion for psychological well-being can be obtained by using exploratory interviews, which is necessary to design qualitative and mixed research studies. Fifth: as a result of the COVID-19 pandemic and the consequent social distancing, the desired data was collected electronically (online survey). For data collection, we suggest using paper, pencils and face-to-face interviews if the situation improves.
CONCLUSIONS
The results of the present study have several practical uses, as it highlights the importance of self-compassion and resilience as two protective factors in promoting the psychological well-being of PwMS. The results of these studies may be used to revise educational and treatment programs to empower PwMS. For PwMS, these educational and therapeutic programs may be delivered in person or online through workshops. It is recommended that psychotherapists promote psychological well-being in PwMS by emphasizing self-compassion and resilience, in addition to standard interventions such as Compassion-Focused Therapy and Compassionate Mind Training.
In this study, resilience was investigated as a mediating factor in the relationship between self-compassion and the psychological well-being of PwMS in Iran. It has been shown that improving adaptability to real-life situations may, directly and indirectly, enhance psychological well-being by increasing self-compassion [57]. Self-compassion is an individual’s preparedness to acknowledge their illness as an element of being human and realize that everyone struggles with problems at some point in their life [58]. In other words, a higher level of self-compassion is associated with a higher level of resilience and psychological well-being.
In this case, Iranian therapists must provide interventions to increase the self-compassion and resilience of these people to tackle cultural issues that limit or undermine self- compassion and resilience.