INTRODUCTION
Syphilis is a sexually transmitted disease caused by Treponema pallidum. In recent years, an increased number of patients with syphilis has been observed. The problem of diagnosis is due to the variety of symptoms. Syphilis is often referred to as the “great imitator” and the “great mimicker" [1]. Neurosyphilis is a term for infection of the central nervous system and can be asymptomatic or resemble any psychiatric, neurological and autoimmune diseases. Negative results of serological tests in serum exclude neurosyphilis [2].
CASE REPORT
A 45-year-old patient was admitted to the Department of Dermatology with a 1-month history of erosions involving the mucous membranes and scalp. He has been treated with nystatin, fluconazole, miconazole and acyclovir without any improvement. The other symptoms were dysphagia and odynophagia and subtle neurological symptoms like tinnitus, mild headaches and spinal pain. The patient denied high-risk sexual behaviors, including anogenital contact. According to the patient, the last sexual intercourse occurred approximately 6 months prior to lesion onset and was heterosexual. Physical examination on admission revealed no abnormalities. Blood test abnormalities included C-reactive protein (CRP) 32.2 mg/l (normal value below 5.0 mg/l) and erythrocyte sedimentation rate (ESR) 22 mm/h (normal value up to 8 mm/h). Chest X-ray, abdominal ultrasound and ophthalmological consultation revealed no abnormalities. The laryngological consultation revealed multiple erosions of the mucous membranes. Pemphigus and pemphigoid autoantibodies were not detected. Also direct immunofluorescence test was negative. Chloroquine and topical corticosteroids were initiated.
After 11 days of hospitalization, new deep erosions appeared in the genital and perianal regions. CRP levels increased to 41.66 mg/l. Antinuclear antibodies (ANA) were detected at a titer of 1 : 5120; however, immunoblot assay was negative. Psychiatric examination revealed high-risk sexual behaviors (men who have sex with men, MSM) and no suspicion of self-inflicted lesions. Following psychiatric examination, the patient admitted that approximately 6 months before the onset of skin and mucosal lesions, he had sexual contact with an unknown man, including orogenital contact. The patient denied a history of a primary lesion.
Serological testing revealed a venereal disease research laboratory (VDRL) test titer of 1 : 16. Other serum tests were also positive: fluorescent treponemal antibody (FTA) test titer of 1 : 1300, fluorescent treponemal antibody absorption (FTA-ABS) test reactive, and Treponema pallidum hemagglutination assay (TPHA) +++. Cerebrospinal fluid (CSF) examination demonstrated marked pleocytosis of 154 cells/μl (normal value < 4 cells/μl), positive Pandy and Nonne–Apelt reactions, and an elevated protein concentration of 64.1 mg/dl. CSF FTA, FTA-ABS, and TPHA tests were positive, while the CSF VDRL test was negative.
Testing for human immunodeficiency virus (HIV), hepatitis C virus antibodies (anti-HCV), hepatitis B surface antigen (HBsAg), herpes simplex virus immunoglobulin M antibodies (HSV IgM), Chlamydia trachomatis polymerase chain reaction (PCR), and Neisseria gonorrhoeae culture was performed; all results were negative.
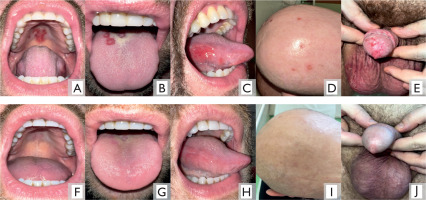
Furthermore, IgG antibodies against Borrelia burgdorferi were positive in the serum and cerebrospinal fluid. Neurological consultation revealed discreet skin hyperesthesia. The magnetic resonance imaging of the brain showed thickening and strong enhancement of the meninges. Based on these findings, a diagnosis of neurosyphilis was established. According to the results of the consultation with the infectious disease specialist, the probability of concomitant neuroborreliosis was low. However, due to the inability to exclude co-infections and the unclear history of Lyme disease treatment in 2014, it was recommended to extend the treatment with crystalline penicillin to 30 days. The patient received crystalline penicillin at a dose of 6 million IU every 6 hours. Since syphilis is the most common spirochetal infection associated with the Jarisch–Herxheimer reaction, and co-infection with Borrelia burgdorferi could not be excluded, prednisone was administered during the first days of penicillin therapy [3]. Following treatment, complete resolution of the skin lesions and improvement in neurological symptoms were observed. The patient was advised to inform his sexual partner about the need for medical evaluation for the diagnosis and treatment of syphilis. However, the patient did not return for follow-up serological testing (Figure 1).
DISCUSSION
In the context of this case report, it is important to recognize that the clinical manifestations of syphilis are highly variable and may present with a misleading or atypical clinical picture. Accurate diagnosis can be challenging due to alternating periods of latency and disease activity. Notably, neurosyphilis may develop at any stage following initial infection [2, 4].
Clinical manifestations of neurosyphilis may include personality changes, cognitive impairment, or behavioral disturbances (33%); ataxia (28%); cerebrovascular events, including ischemic strokes (23%); visual disturbances (17%); urinary incontinence and other urinary tract symptoms (17%); piercing pains (10%); headaches (10%); vertigo (10%); sensorineural hearing loss (10%); seizures (7%) [5]. Clinicians should also be aware of less common manifestations of neurosyphilis, including tinnitus, as illustrated in the present case. In the case of otosyphilis, hearing loss occurs in 90% of cases, tinnitus in 73%, and vertigo in 53% [6, 7].
There are five types of neurosyphilis. Early stages include asymptomatic, meningeal, and meningovascular syphilis, and late stages include syphilitic paresis and syphilitic myelitis. In addition, ocular and auditory symptoms may be present, which are a form of neurosyphilis [5]. The most common is asymptomatic form of neurosyphilis, it occurs in one third of patients [8]. To diagnose neurosyphilis, a positive nontreponemal and treponemal serum test should be confirmed. It should be remembered that nontreponemal may normalize over time and in late neurosyphilis can be negative [1]. The diagnosis of neurosyphilis is difficult due to the lack of one standardized test. Polymerase chain reaction (PCR) is a very sensitive method for diagnosing syphilis from primary ulcers and secondary wet lesions. Unfortunately, PCR is not useful on CSF because of its low sensitivity. A systematic review estimated the sensitivity and specificity of PCR for confirmed neurosyphilis to be 40% to 70% and 60% to 100%, respectively [9]. The Food and Drug Administration (FDA) did not approve PCR for CSF testing in syphilis [10]. The final diagnosis is based on the patient’s history, symptoms, clinical findings, imaging, CSF analysis and results of serological tests in serum and in CSF [11–16]. To diagnose neurosyphilis, it is necessary to perform a CSF examination. If it is not possible to collect a CSF sample, full neurosyphilis treatment should be considered according to the treatment recommendations. This approach was argued as it is better to overtreat some patients than to undertreat others [5]. Due to this, syphilis is called the great imitator and mimicker, the range of differential diagnoses, also in case of neurosyphilis, is very wide.
Differential diagnosis of neurosyphilis includes: meningitis of a different etiology, encephalitis, acute psychiatric diseases, psychoorganic diseases, e.g. Alzheimer’s disease, neoplasms in the central nervous system, vascular diseases, Lyme borreliosis, sclerosis multiplex and other neurodegenerative diseases, abuse of the psychoactive substances, endocrine and metabolic disorders, and electrolyte disturbances [2, 5].
In the presented case, due to mucosal and neurological symptoms and unclear venereal history, Behçet’s disease was initially suspected. According to the Behçet’s disease criteria, ocular lesions, genital aphthosis and oral aphthosis are assigned 2 points each, skin lesions, neurological symptoms, vascular symptoms and a positive pathergy test are assigned 1 point each, a result ≥ 4 points indicates Behçet’s disease [17]. A summary of mucocutaneous symptoms in syphilis and Behçet’s disease is presented in Table 1 [17, 18].
Table 1
Comparison of mucocutaneous lesions in syphilis and Behçet’s disease; features observed in the present case are highlighted in bold [17, 18]
CONCLUSIONS
Given the diagnostic challenges associated with the variable clinical presentation of syphilis, screening appears particularly important in high-risk populations, including young sexually active individuals, people living with HIV, and MSM. When syphilis is diagnosed, comprehensive screening for other sexually transmitted infections (STIs) should be performed. Conversely, syphilis should always be considered and excluded in patients diagnosed with other STIs [19].