Introduction
Type 1 diabetes (T1DM) is a chronic metabolic disease characterised by hyperglycaemia – raised blood plasma glucose level. The disease usually affects children and teenagers and it represents 5–10% of all diabetes cases [1, 2]. In Poland, 6400 children aged 0 to 14 suffer from type 1 diabetes [3].
The aetiology of juvenile diabetes remains to be fully explored. The pathological process involves the dysfunction or destruction or the β cells of islets of Langerhans in the pancreas, which are responsible for insulin production and secretion. The first symptoms of T1DM, such as polydipsia, weight loss and general fatigue, appear suddenly [4].
The basic T1DM treatment is insulin therapy plus proper diet, care and regular adapted physical activity. T1DM patients and their carers who have been properly trained and prepared to cope with the disease, function better in daily life settings.
Diabetes education is usually addressed to diabetic patients and to nurses, who are responsible for carrying out educational programmes at home and in hospital, until the patient switches from a medical therapy model to a home-based therapy model [5]. It was introduced in 1922 as an indispensable element of treating diabetic patients, when Frederick Grant Banting and Charles Herbert Best discovered insulin [6]. In Poland, efforts to obtain educators in the treatment of diabetes, whereby supporting families and patients, have theoretically been undertaken since 2011. This also includes the obtainment of doctors – family doctors, diabetologists, paediatricians and staff of educational institutions [7]. An important role of diabetes education is played by physiotherapists on therapeutic teams, in order to guarantee top quality patient treatment of type 1 diabetes. The Polish physiotherapist Act lists physio-prophylaxis as one of the health services provided within physiotherapy. Its purpose is to promote a healthy lifestyle and to build and sustain physical fitness and endurance for people of various ages in order to prevent disability [8].
Physiotherapists may play an important part in raising the awareness of patients and society as regards T1DM. They can also play an important role in the prevention of concomitant diseases and health promotion in a broader sense. They should also promote physical activity as a way to eliminate risk factors such as obesity and kinesiophobia.
The objective of the paper is to assess the level of T1DM education among physiotherapists versus selected factors.
Material and methods
The poll was conducted between 10 and 28 February 2020 as a questionnaire posted on social media physiotherapy groups. To participate in the poll, every respondent with a license to practice had to give their written consent. The original questionnaire included personal questions – age, sex, residence, education, years of practice, place of work, and a Diabetes education knowledge test (single-select) regarding T1DM. The respondents got one point for a correct answer and zero points for an incorrect answer. The total knowledge test results were classified depending on the total score into: low (0–8 points), medium (9–13 points) and high (14–17 points).
The respondents included 103 physiotherapists from Poland aged 20 to 50, with an average age of 31.7 ±5.5 years. 66 were women (64.1%) and 37 were men (35.9%). The majority of the respondents lived in towns or cities (83.5%) and had a master’s degree (76.7%). The most commonly declared number of years in the profession ranged from 1 to 5 years (47.6%). The answers to the question about the place of work were: hospital ward for 45 respondents (43.7%), individual physiotherapy practice for 25 respondents (24.3%), physical rehabilitation clinic for 20 respondents (19.4%), a university for ten respondents (9.7%), and a nursing home for three respondents (2.9%). A detailed description of the respondents is presented in Table I.
Table I
Description of the physiotherapists filling out the questionnaire (n = 103)
Table II
Results of the diabetes education test demonstrating the knowledge and lack thereof as regards detailed T1DM issues
Table III
Determinants of the diabetes education level for the physiotherapists filling in the questionnaire
Qualitative variables were described based on the number of observations with attribute variant (n) and the corresponding value (%). The distribution normality for the variable was checked with the Lilliefors test and the Shapiro-Wilk test. The Wilcoxon signed-rank test was used to measure the relationship between the variables. The correlation between variables on the ordinal scale was addressed based on the monotonic correlation Spearman’s Rho. The correlation between the variables on the nominal scale was measured with the chi-square test with Fisher’s adjustments and with Pearson’s C and Cramér’s V measures of association.
The analysis was conducted using the IBM SPSS 25.0 software. Associations (correlations) were treated as statistically significant when p ≤ 0.05.
Results
When asked about the sources of T1DM A education, 72 respondents (36,5%) selected websites, 71 – medical literature (36%), 36 – university classes (18.3%) and 18 – a physician (9.1%).
The majority of the physiotherapists filling in the questionnaire (57.3%) provided therapy to adult patients, while 42.7% worked with children. Twenty-five (24.3%) respondents claimed to have a family member or friend suffer from T1DM.
As far as the total score for correct answers was concerned, the knowledge level was medium for the majority (69 (67%)) of the respondents, high for 28 respondents (27.2%) and low for six respondents (5.8%).
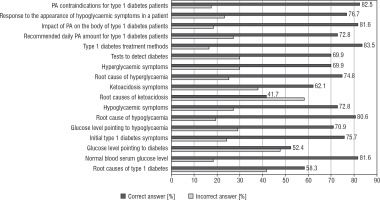
The respondents’ diabetes education, manifested with either knowledge (yes) or lack thereof (no) when it came to specific T1DM-related issues, is presented in Table II and Fig. 1.
The poll has shown a statistically significant relationship between the respondents’ subjective assessment of the level of their T1DM knowledge and the level of knowledge resulting from the number of proper answers in the test. Those who declared substantial knowledge had a higher score (p = 0.029). For sources of knowledge about T1DM, higher scores were achieved by respondents using medical literature (p = 0.07) and university classes (p = 0.042). The other tested variables were not statistically significant (p > 0.05) for the level of knowledge of diabetes. Detailed data are presented in Table III.
A statistically significant correlation was observed between the years of employment as a physiotherapist and the level of T1DM knowledge (r = 0.196, p = 0.047). The respondents that were on the job longer had more answers that were correct. The level of knowledge was not correlated with the age (r = 0.113, p = 0.258) or sex (r = 0.142, p = 0.344) or subjective self-assessment of knowledge (r = –0.04, p = 0.685) of the respondents (Table III).
Discussion
Diabetes has been referred to as the epidemic of the 21st century for several years now [9]. According to WHO data from 2019, 463 million people suffer from diabetes worldwide. The number of patients is anticipated to increase by 115 million by 2030 [10]. Diabetic patients face various challenges, such as gaining knowledge about the disease, developing self-control and coping with the psycho-social problems (risk of depression and rejection) and needing to change their lifestyle. Health care workers ensure that the necessary needs of patients are met, including preparing them for life with the disease and preventing its secondary consequences [11]. According to Kucharski, the Polish health care system is difficult for every patient, and it is another constant challenge for young patients, chronically ill patients and their families [12].
Since T1DM generates high treatment costs that reach 5–10% of the global healthcare budget, a comprehensive therapy is important that also encompasses physiotherapy. This may reduce considerably the number of complications and, by extension, lower the treatment costs [3].
One of the primary therapeutic objectives in Poland is to improve the quality of diabetes treatment. According to the Polish Diabetes Education Association (SED), an important means to this end is to introduce actual (real) educational advice in diabetic care, to give high priority to therapeutic education adapted to diabetic age groups and to finance educational programmes and consultations for patients which can be delivered by nurses, educators, psychologists and physiotherapists from the Polish National Health Fund (NFZ).
T1DM entails many extra duties and restrictions for a child, requires self-discipline and self-control in daily monitoring of glucose levels, specific diet, insulin therapy and control of physical activity [13, 14]. Physiotherapists should especially take care of the educational aspects regarding properly adapted physical activity. Trojanowska et al. assessed the impact of knowledge on the health-related behaviour of children with type 1 diabetes. Their study has shown that such children were inadequately prepared for a healthy lifestyle. The study participants demonstrated a lower level of healthy behaviour, especially in terms of physical activity, self-control, diet and the duration of sleep [15].
Holistically speaking, physical activity is an important stimulator or proper development of children and teenagers and a major factor reducing the risk of cardiovascular diseases, cancers and mortality rates [16–18]. The effect of physical activity on the level of metabolic control in T1DM remains a topic of many discussions. No independent impact of physical activity on improvement of glycaemic control has been successfully demonstrated for T1DM patients. Regular physical activity reduces the demand for insulin, normalises and improves the lipid profile, stimulates the development of muscles and improves the condition and well-being of the patient [18, 19]. T1DM patients often have problems keeping proper body weight and fail to reach even the minimum daily amount of physical activity [20].
There is also an important problem of emotional barriers that limit the physical activity of T1DM patients. They include: fear of hypoglycaemia, loss of glycaemic control and lack of knowledge regarding physical activity [21]. It may be crucial for the patient to receive detailed information on the rules of engaging in physical activity from a physician or a physiotherapist, also in the psychological aspect.
Children are currently encouraged to exercise for at least 60 minutes a day to reduce the risk of vascular complications [21, 22]. Children with T1DM may undertake most types of physical activity, especially if its intensity ranges from 40 to 56% of VO2max or 55–69% of maximum heart rate [23, 24]. In our questionnaire, 72.8% of physiotherapists knew the physical activity amount for T1DM patients, its impact on their bodies (81.6%) and the contraindications (82.5%). Importantly, as many as 76.7% respondents knew what to do if the patients showed hypoglycaemic symptoms.
Contraindications for physical activity in T1DM patients include a blood glucose level above 250 mg/dl (13.9 mmol/l) and the presence of ketone bodies in urine. Exercise is also ill-advised in the case of glycaemia below 70 mg/dl (3.9 mmol/l) [25]. The majority of respondents in our questionnaire knew the root causes of hyperglycaemia (80.6%), hyperglycaemia (74.8%) and their symptoms (72.8% and 69.9% respectively).
One of the contraindications for physical activity mentioned in the knowledge test was ketoacidosis and its symptoms. It is a state of disrupted metabolism of carbohydrates, lipids and proteins, water and electrolyte balance and the acid–base balance resulting from a severe insulin deficiency. It causes hyperglycaemia and increased lipolysis, with ketone bodies in blood and urine. Clinical symptoms of acidosis include but are not limited to: weakness, polydipsia, dryness of skin and of mucous membranes, accelerated heart rate and acetone breath. The risk of acidosis occurs primarily in martial arts and in team sports [19, 26, 27]. 62.1% of physiotherapists in our questionnaire, properly defined ketoacidosis symptoms, while 58.3% did not know the root causes of ketoacidosis.
As far as the sources used to broaden the knowledge about T1DM were concerned, 36% selected medical literature. Only the specified sources entailed significantly higher levels of knowledge about diabetes. Just 18.3% of the respondents relied on university classes in terms of T1DM knowledge. It is an important aspect in the context of creating programme guidelines for medical schools. In the study by Steyl, 60 physiotherapy students had vast knowledge about T1DM [28]. In contrast, the study by Janeczek et al. revealed very poor knowledge of nursing students about type 2 diabetes. The authors pointed to a clear need for broader education of students in the area of diabetes in medical schools [9].
The majority of the physiotherapists in our questionnaire (81.6%) selected the right blood serum glucose level but only 52.4% defined the hyperglycaemia level. The respondents also knew the initial T1DM symptoms (75.7%) and the disease diagnostic methods (69.9%). Diabetes can be successfully controlled through proper treatment and a healthy lifestyle, which has a huge impact on the quality of life of a sick child and on the course of the therapy [15]. Therapeutic education means guiding the patients to change their health-related behaviour in a way that benefits their health. The main purpose of education is to prepare a diabetic patient to lead a lifestyle consistent with their conscious choices, based on self-reliance, knowledge, proper conduct and self-responsibility. It is up to the patients and their families to keep the diet, self-control and engage in adapted physical activity. Clinical trials and observations show that education substantially helps lower the risk of severe and late diabetes complications which end in disability and death [5, 14].
Ramova and Macedonia tested the knowledge of physiotherapists about the complications of diabetes. The majority of the respondents had an average result. The authors noted the need to expand physiotherapy teaching programmes by including the knowledge of diabetes and the physical treatment of its complications [29]. In our questionnaire, 67% of the respondents had medium knowledge about type 1 diabetes, which reflected their subjective assessment of their knowledge. Curiously enough, factors such as education, place of work and their loved ones suffering from T1DM, were found to have no impact on diabetes-related knowledge of the respondents. Only the years working in the relevant field had a positive correlation with the result in the knowledge test.
So perhaps systematic diabetes training should be considered for physiotherapists. After all, it is important to emphasise the important role that a physiotherapist who works closely with the doctor, nurse and patient may play in improving the quality of life of those who suffer from diabetes. Positive effects at all diabetes treatment stages, requires physiotherapists to be knowledgeable about the disease [9].
In the therapy of chronic diseases, therapeutic education supplements and supports the treatment, which is generally designed to primarily bring the life span and quality of life of a sick child to that of its healthy peers [15]. Patients’ access to physiotherapists is an important problem as far as engaging in physical activity is concerned. According to the study by Wojciechowski et al., as many as 48.0% diabetic patients stated that they had no access to physiotherapy services [11].
Physioprophylaxis in the form of physical activity is not only beneficial for the physical aspect of the patient, but it also improves their general well-being and self-esteem and, by extension, their quality of life. Physiotherapists on the treatment team play an important role in education of T1DM patients. They should be the promoters of a healthy lifestyles, based essentially on regular physical activity. The majority of those tasks require up-to-date and professional knowledge of T1DM.
Conclusions
Physiotherapists may play an important role in the process of education and treatment for diabetes. However, achieving this goal (thesis) requires a comprehensively high level of cognitive and practical competence in the understanding of type 1 diabetes. In the research results presented, the majority of physiotherapists presented an average level of knowledge about diabetes, which was mostly determined by the number of years working in the profession. The age and sex of the respondents had no significant impact on the level of their diabetes-related knowledge. Confronting the above-mentioned data of the examined group of physiotherapists, with the demand for educated and experienced health educators (including their level of competence), reveals the progress in achieving this role. However, it should be noted that the growing number of patients suffering from type 1 diabetes and the progress in T1D prevention and treatment technologies, indicate a real need to adjust the content of the curriculum at physiotherapy studies and training institutions for working physiotherapists, to obtain up-to-date and comprehensive specialist knowledge of diabetes.